Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Selene Ting, Medical Registrar, Counties Manukau District Health Board, Auckland, New Zealand. Copy edited by Gus Mitchell. March 2021
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Pustular psoriasis of pregnancy, also known as impetigo herpetiformis, is a rare variant of generalised pustular psoriasis that occurs in pregnancy.
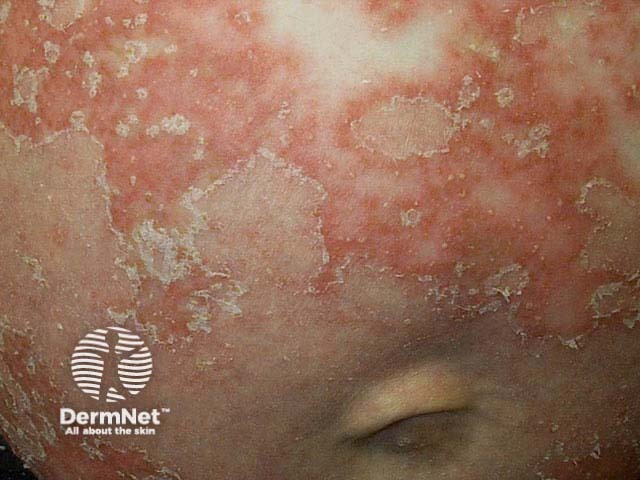
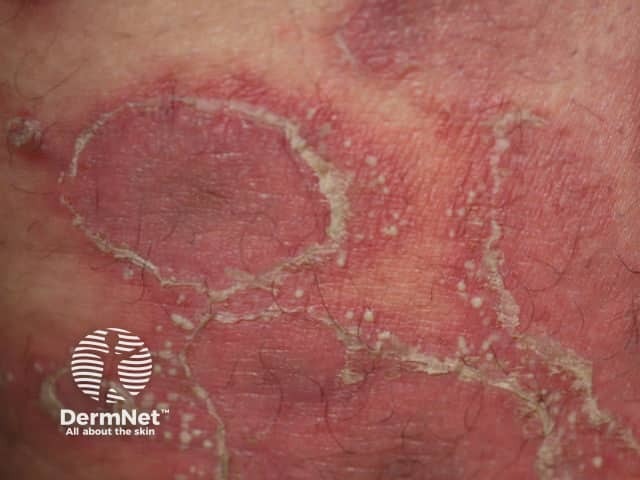
Generalised pustular psoriasis
Pustular psoriasis of pregnancy typically appears in the third trimester of pregnancy and resolves rapidly after delivery, although the timing of onset can range from the first trimester to the immediate post-partum period. It can recur in subsequent pregnancies, often at an earlier stage. Pustular psoriasis of pregnancy has also been reported with oral contraceptive use and the menstrual cycle. Many women who develop pustular psoriasis of pregnancy have a personal or family history of psoriasis.
The pathogenesis of pustular psoriasis of pregnancy is unclear. Postulated triggers on a predisposing genetic background such as IL36RN gene mutation include:
Pustular psoriasis of pregnancy presents as symmetrical annular or polycyclic erythematous patches and plaques, with the formation of sterile pustules at the periphery, beginning in skin folds and spreading to the extremities and trunk. The pustules rapidly merge to form large plaques with desquamation and red-brown pigmentation. The face, palms, and soles are usually spared. The oral mucosa is sometimes involved with pustules that leave circinate or erosive lesions on the tongue or buccal mucosa.
Pustular psoriasis of pregnancy is often accompanied by constitutional symptoms which may include fever, malaise, nausea and diarrhoea, arthralgias, tachycardia, delirium, and seizures.
Pustular psoriasis of pregnancy should be considered in a pregnant woman with a spreading pustular skin rash and constitutional symptoms. Investigations may include:
Early delivery should be considered in severe disease as pustular psoriasis of pregnancy can be life-threatening yet typically resolves rapidly postpartum.
Pustular psoriasis of pregnancy usually settles quickly after delivery of the baby, although some changes of psoriasis may persist long-term.
Pustular psoriasis of pregnancy can recur with subsequent pregnancies, and may present earlier in the next pregnancy and in a more severe form.
Pustular psoriasis of pregnancy carries a poor prognosis for mother and/or fetus if untreated.