Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Haylee Boyens, Medical Student, University of Auckland, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, December 2014.
Introduction Early signs Causes Clinical features Investigations Treatment Prognosis
Gangrene is the localised death of body tissue. Dry gangrene is due to prolonged ischaemia (infarction) or inadequate oxygenation or lack of blood flow. Ischaemia affecting proximal blood vessels usually affects the lower limbs. Ischaemia of the peripheries may cause gangrene of fingers and toes.
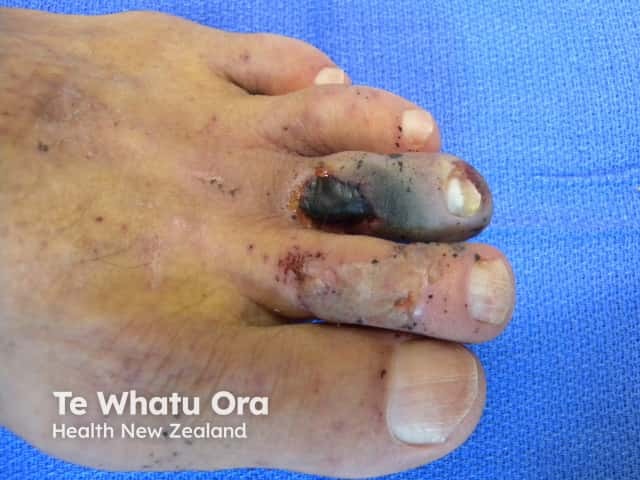
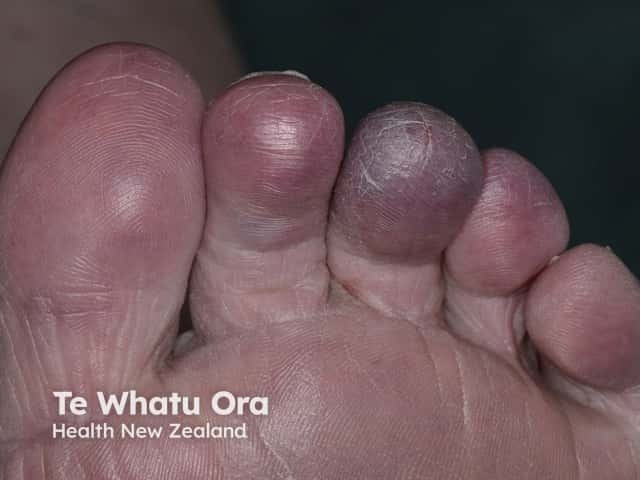
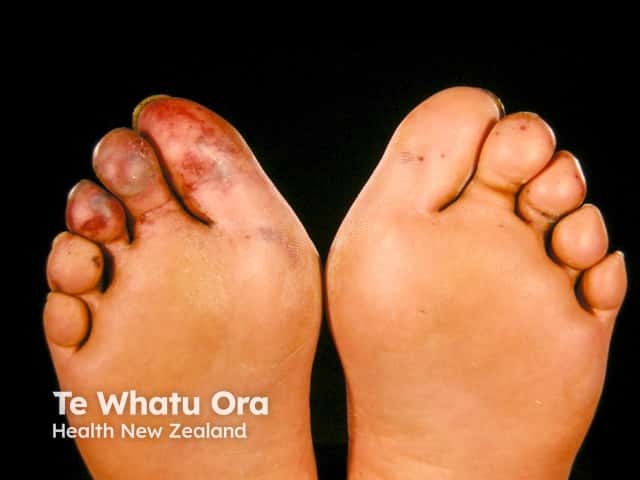
Dry gangrene due to ischaemia
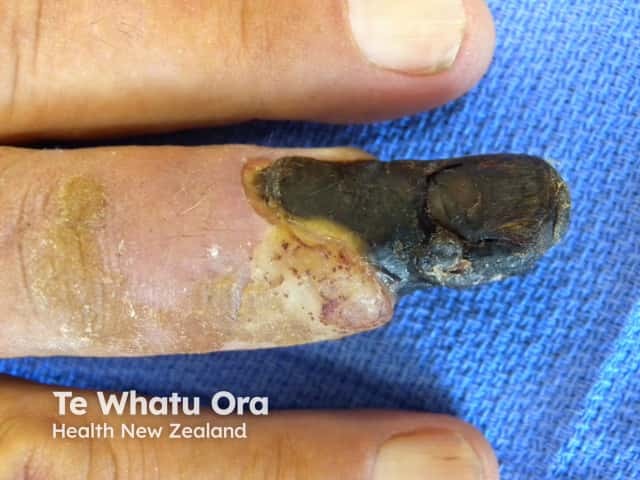
Dry gangrene due to ischaemia
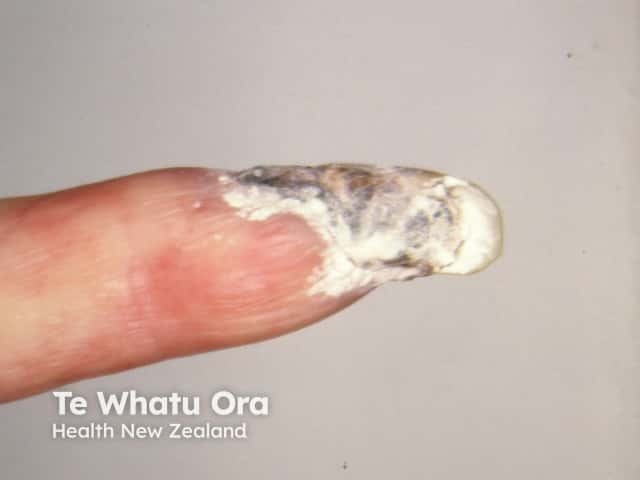
Dry gangrene due to ischaemia
Proximal severe acute ischaemia presents as a pale, paralysed pulseless limb. This is a surgical emergency because it may progress to extensive gangrene if the obstruction is not rapidly removed.
Distal peripheral vascular obstruction presents as blue, grey or purple patches, blisters or ulcers at the ends of the digits. See blue toe syndrome.
Ischaemia in other sites may also result in localised necrosis of the skin and deeper tissues.
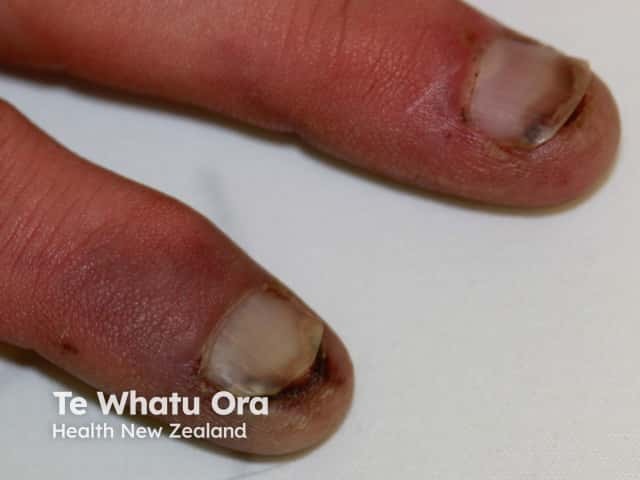
Ischaemia is due to an acute or chronic interruption in blood supply and is often due to a combination of both.
Acute ischaemia may be due to:
Emboli are particles that flow through the bloodstream until they lodge at an arterial junction or narrowing. Emboli may be composed of:
Large emboli lodge at the femoral artery bifurcation (43%), the iliac arteries (18%), the aorta (15%), and the popliteal arteries (15%). Small ones are deposited in the fingers and toes, palms and soles.
Vascular obstruction may also be due to hyperviscosity syndromes or abnormal circulating proteins such as cryoglobulins or macroglobulins.
Thrombosis is a blood clot arising within a blood vessel. Predisposing factors include:
Whatever the primary cause of ischaemia, thrombosis due to sluggish blood flow can make it worse.
Chronic ischaemia may be due to:
Chronic peripheral arterial disease is most often due to atherosclerosis. This is a build-up of cholesterol, fibrin and other proteins within the arterial wall, causing the vessel to narrow and eventually become completely blocked. This process is also called arteriosclerosis obliterans.
Risk factors for peripheral arterial disease include:
Peripheral arterial disease may also be due to:
The veins may fail to clear blood from the tissues because of valve dysfunction (varicose veins) and obstruction from deep venous thrombosis (DVT) or thrombophlebitis. High pressure within the veins (venous hypertension) results in movement of proteins and fibrin into the soft tissue. This leads to fibrosis, dysfunctional capillary formation and fat necrosis (lipodermatosclerosis). When severe, these processes may cause ischaemia and gangrene.
Signs of peripheral vascular disease depend on which tissues are ischaemic and its severity. A patient may present with:
When a patient presents with peripheral ischaemia or gangrene of unknown cause, a thorough physical examination is undertaken to evaluate the vascular system including the heart and the peripheral pulses. An electrocardiogram (ECG) assesses cardiac function. Blood pressure is measured by Doppler ultrasound of both lower limbs and both upper limbs to calculate the Ankle Brachial Index (ABI).
Imaging to evaluate peripheral vascular disease may include:
Blood tests assess blood count, kidney function, electrolytes, lipid profile, coagulation status and inflammatory markers such as D dimer and C reactive protein.
Treatment of gangrene varies depending on location and cause but is centred around radical surgical debridement +/- amputation. Surgical procedures may also include:
Medical treatment may include:
Prognosis of ischaemic gangrene depends on the extent of disease, the underlying cause and the timing of appropriate treatment.
There will be scarring, and there may be some reduction in function, especially if significant debridement or amputation has been necessary. Recurrence of ischaemia is likely due to medical comorbidity, especially diabetes.