Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Todd Gunson, Dermatology Registrar, Greenlane Clinical Centre, Auckland, New Zealand, 2007.
Introduction - cholesterol
Introduction - cholesterol embolus
Causes
Demographics
Clinical features
Diagnosis
Treatment
Other embolism-causing substances
Cholesterol is a sterol (a combination of steroid and alcohol). It is a fatty, waxy substance found in the membrane that surrounds every cell of the body. It is an essential component of tissues in animals, plants and fungi.
Cholesterol in humans is mainly manufactured by the liver, but some is of dietary origin. It is transported in the bloodstream in small low-density and high-density lipoprotein particles (LDL and HDL cholesterol). High levels of cholesterol, particularly LDL, promotes the development of atherosclerotic plaques in arteries. These cause narrowing of the arteries in coronary artery disease and central or peripheral vascular disease
A cholesterol embolus is a deposit of cholesterol lodged inside a blood vessel of the skin or an internal organ. This prevents the flow of blood through small calibre arteries and causes malfunction or death of the tissue supplied by the affected blood vessel. The process is also called atheroembolism.
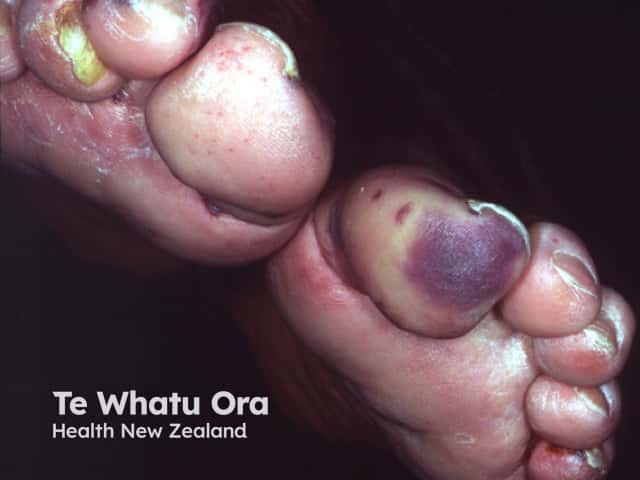
Cholesterol emboli
Cholesterol emboli originate from ulcerated arteriosclerotic plaques, which can release cholesterol fragments (emboli) into the bloodstream. This may occur spontaneously, but most often occurs after a procedure that disrupts the plaque surface. Studies suggest it may occur within hours to days following up to 1% of vascular procedures, such as:
Trauma to the abdomen can rarely precipitate this syndrome by disrupting arteriosclerotic plaques within the abdominal aorta.
Drugs that are used for thrombolysis (to reopen a clotted vessel following a heart attack or stroke) or anticoagulation (to thin the blood) may also predispose to embolisation of cholesterol from unstable plaques. This occurs because the overlying blood clot dissolves, or an arteriosclerotic plaque bleeds. The risk is thought to be very low, but it has been occasionally reported within days or up to several months after commencing anticoagulant therapy.
Those who have atherosclerosis are at risk of cholesterol emboli. This includes patients with ischaemic heart disease or peripheral vascular disease, as well as those with risk factors such as diabetes, high blood pressure, smoking, obesity, older age, and high levels of cholesterol in the blood.
Classic constellations of symptoms are:
The skin is affected in over one-third of patients resulting in livedo reticularis, gangrene, cyanosis (‘blue toe syndrome’ secondary to lack of oxygenated blood supply), ulceration, painful red nodules, and purpura (purple patches).
Cholesterol fragments blocking blood vessels to other organs may result in specific symptoms and signs:
Non-specific symptoms such as fever, myalgia (muscle ache), headache, and weight loss may be present. Myocardial infarction (heart attack) and stroke do not usually result from cholesterol emboli.
A high index of suspicion is required especially in a patient with known atherosclerosis who has developed the typical skin changes, kidney failure, abdominal pain or diarrhoea, following a vascular procedure.
Definitive diagnosis is made from a skin biopsy or a biopsy of other involved tissue. The histology of cholesterol emboli should show diagnostic cholesterol crystals or clefts within the blood vessel wall, along with thrombi (blood clots). The clefts are spaces left by the crystals that have been washed out by the tissue fixation.
Blood tests show an eosinophilia in up to 80% of affected patients. Other changes that may be seen include:
The best strategy is the prevention of arteriosclerosis with control of vascular risk factors.
Once cholesterol emboli have occurred, procedures to prevent further embolisation such as removal or stenting of unstable atheromatous plaques may be considered. Drugs such as statins, iloprost, pentoxifylline, and systemic steroids have been reported to have limited success to minimise organ damage.
Cholesterol is the most common cause of the cutaneous embolic syndrome. However other causes include:
Medscape Reference: