Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Megan Lam, Michael G. DeGroote School of Medicine, McMaster University, Canada. DermNet NZ Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, April 2020. Minor amendment: Dr Ian Coulson, Dermatologist and Editor-in-Chief, March 2024.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
An epidermoid cyst is a benign cyst derived from the infundibulum or upper portion of a hair follicle, encapsulated in a thin layer of epidermis-like epithelium. Epidermoid cysts are typically filled with keratin and lipid-rich debris [1,2].
Synonyms for an epidermoid cyst include:
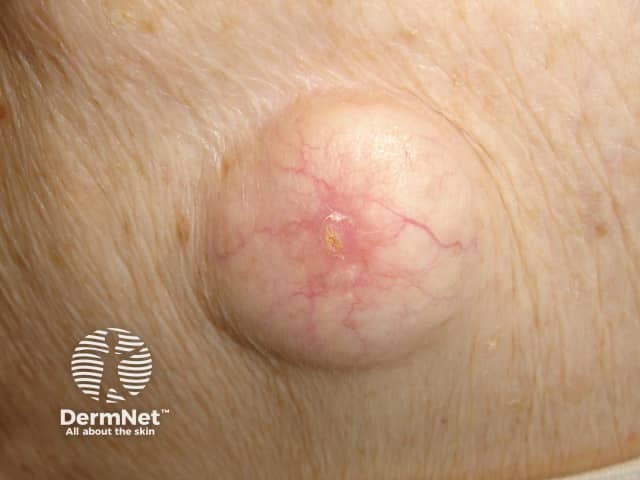
Epidermoid cyst
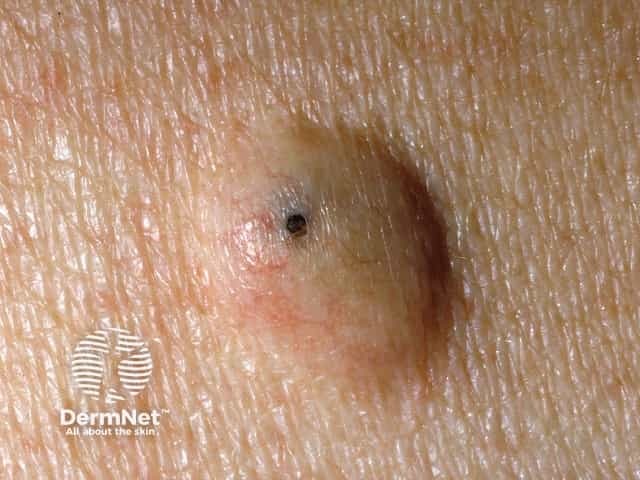
Epidermoid cyst with an obvious punctum
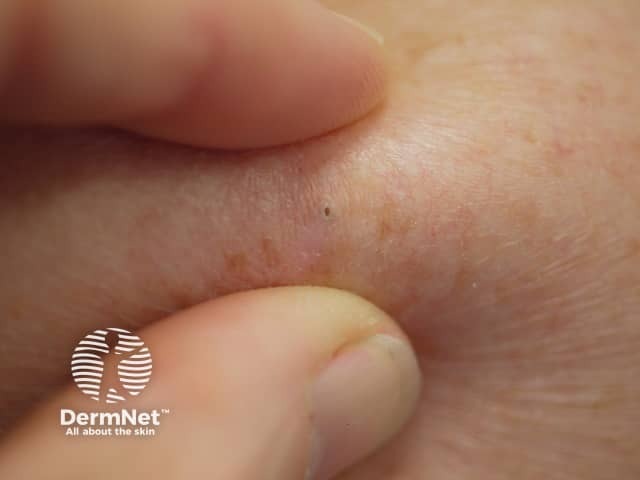
Palpating an epidermoid cyst - note this accentuates the punctum
Epidermoid cysts most commonly occur in adults, particularly when young-to-middle aged. They occur twice as frequently in men than in women [3]. They may occur frequently in acromegaly. Multiple small epidermoid cysts on the cheeks are seen associated with solar elastosis in Favre-Racouchot syndrome.
Genetic disorders which may increase the risk of developing multiple epidermoid cysts include [1]:
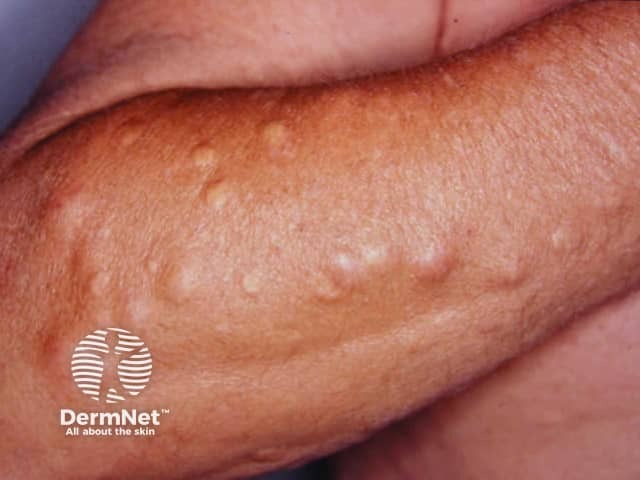
Gardner syndrome
An epidermoid cyst generally results from an occluded pilosebaceous unit.
On non-hair-bearing areas of the body, such as the buttock, palm of the hand, or sole of the foot, an epidermoid cyst may be due to traumatic implantation of epidermal cells into the dermis where keratin accumulates within an epithelium-lined sac [2].
The clinical features of an epidermoid cyst include [4]:
Epidermoid cysts are most common on the central trunk (eg, chest and shoulders) and face but can occur almost anywhere on the body. Epidermoid cysts are common the scrotum and vulva. They may be solitary or multiple, and are generally asymptomatic.
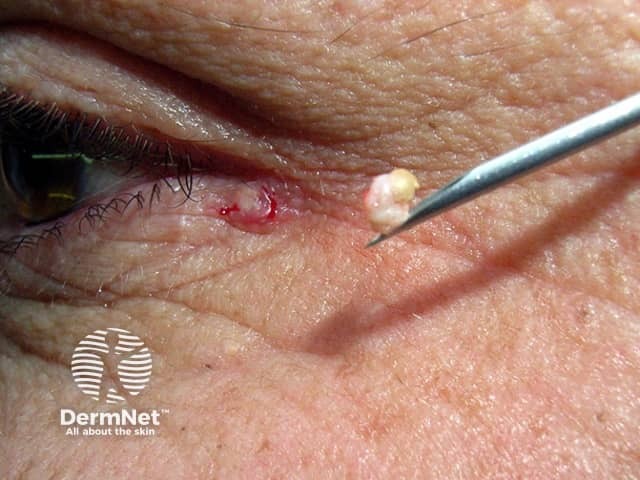
The contents of a s small lid epidermoid cyst incised with a green needle
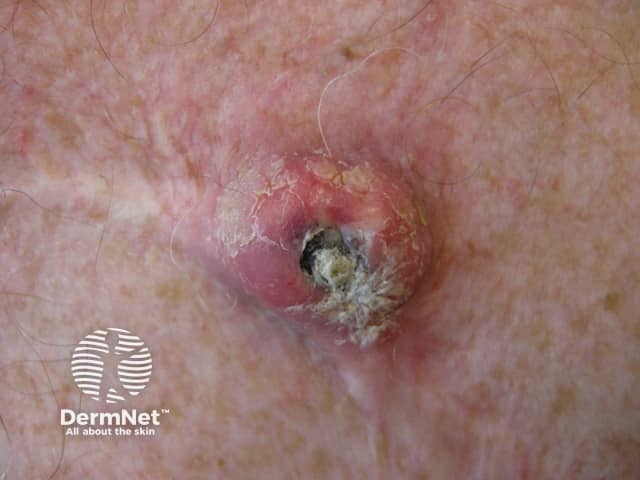
A recurrent epidermoid cyst - note the scar from a previous incomplete excision
Rupture of the cyst contents into the dermis results in swelling, redness, and tenderness. This can be due to trauma or bacterial infection, commonly by Staphylococcus aureus, Escherichia coli, and group A streptococcus [1].
Surgical excision can lead to bleeding, secondary bacterial infection, and scarring. If the cyst has ruptured, or the capsule is not removed in its entirety, the cyst may recur.
Cutaneous squamous cell carcinoma may very rarely arise within an epidermoid cyst [5].
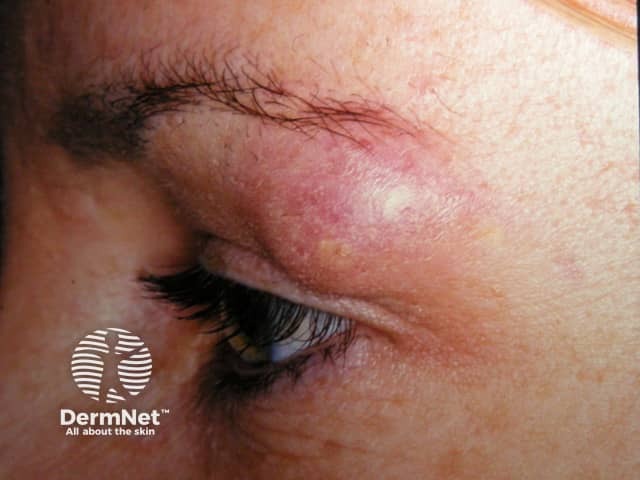
An inflamed cyst on the lid
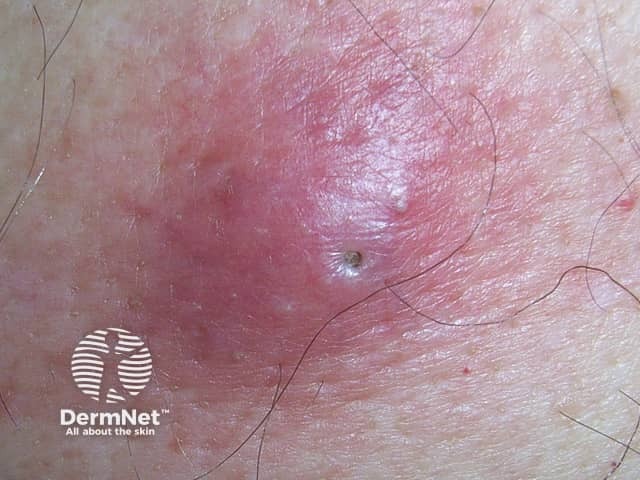
An inflamed cyst accentuating the punctum
The diagnosis of an epidermoid cyst is usually made clinically.
Biopsy is usually not required but the lesion may be excised for cosmetic reasons or due to complications. Histological features of an epidermoid cyst include [1]:
Ultrasound can be used in the initial evaluation of a soft tissue mass but is not usually required for a typical epidermoid cyst.
Differential diagnoses for an epidermoid cyst include:
Most small uncomplicated epidermoid cysts will not require treatment.
The most effective treatment for an epidermoid cyst is complete surgical excision with an intact cyst capsule. Removal of the entire cyst lining decreases rates of recurrence [6]. This can be difficult to achieve following cyst rupture. Histological examination of the surgical specimen is recommended due to the small risk of malignant transformation and misdiagnosis [6].
In cases of infection, initial antibiotics, incision and drainage may be indicated.
Epidermoid cysts are typically benign and slow growing, rarely undergoing malignant transformation. Occasionally, they resolve spontaneously without intervention [1].