Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Marie Hartley, Staff Writer, 2010. Updated by Dr Ian Coulson, Dermatologist and Editor-in-Chief, March 2024.
Acromegaly is a chronic (slowly progressive) condition caused by excess growth hormone in adulthood.
Growth hormone is normally produced by the pituitary gland, a tiny gland located at the base of the brain. The pituitary gland produces a number of different hormones and is controlled by a region of the brain called the hypothalamus. The hypothalamus produces growth hormone-releasing hormone (GHRH) which in turn stimulates the pituitary gland to produce growth hormone. Growth hormone is essential for physical growth in children and adolescents, as it stimulates another hormone, insulin-like growth factor-I (IGF-I). IGF-1 causes the body tissues to gradually enlarge in normal childhood growth but also results in the changes seen in acromegaly.
In more than 98% of patients with acromegaly, the condition is caused by a pituitary adenoma (a non-cancerous tumour of the pituitary gland), which secretes excess growth hormone and/or IGF-1. Rarely acromegaly is caused by a growth hormone- or GHRH-producing tumour located in a distant organ, such as the lung or pancreas.
Acromegaly is a rare condition with around 3–4 new cases per million population per year. It is generally diagnosed in middle-aged people. However, the symptoms are initially quite subtle and may have been present for many years before the diagnosis is made.
Pachydermoperiostosis can mimic acromegaly but is not associated with growth hormone excess.
Excess growth hormone in adulthood does not increase height because the growth plates in adult bones have fused. Children and adolescents are able to grow upwards due to open cartilage growth plates at each end of long bones. After puberty, the growth plates fuse and no further lengthening of the bones is possible. Gigantism is a related condition, where patients are remarkably tall due to excess growth hormone while growth plates are open during childhood.
Initial symptoms of acromegaly can be caused by the physical effects of the tumour on surrounding tissues (eg, headaches, visual disturbances) or by the consequences of overgrowth of bones, cartilage, tissues, and organs.
Skin changes associated with acromegaly include:
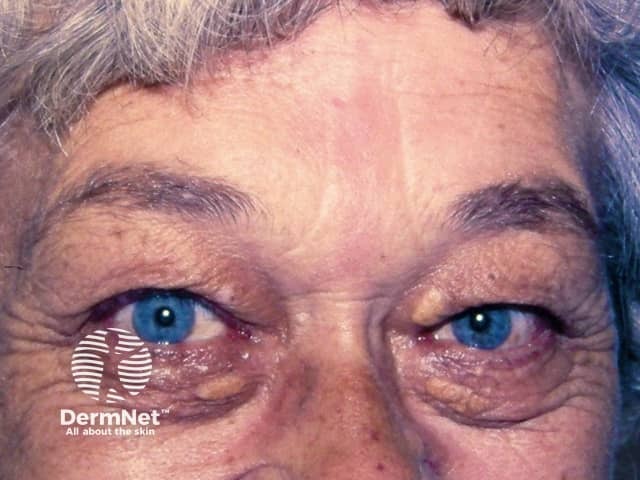
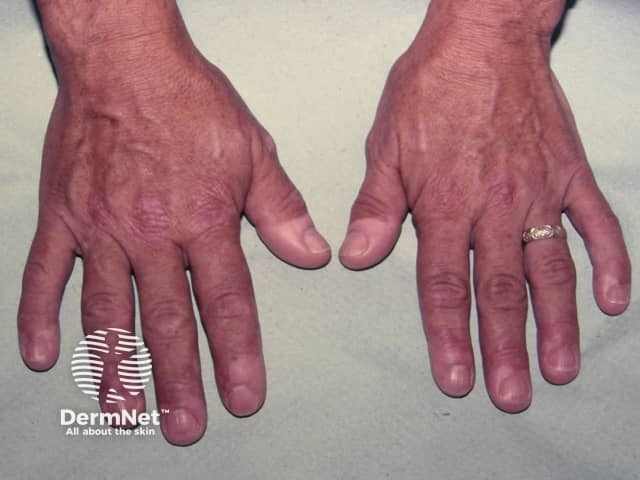
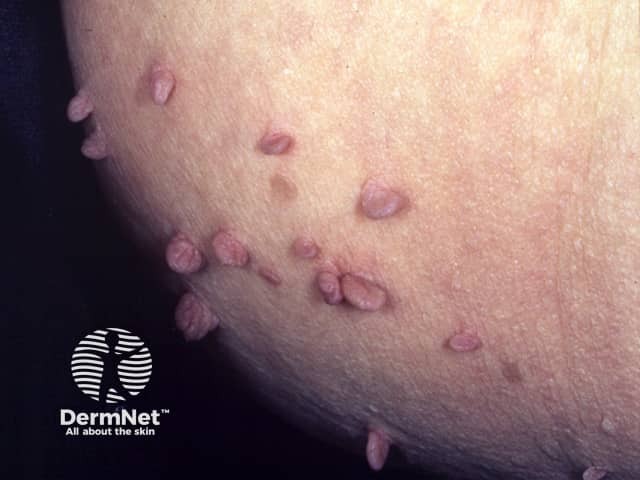
Skin tags
Other clinical features of acromegaly include:
Complications include:
There are three general approaches to the treatment of acromegaly:
Often a combination of treatment approaches are used, for example surgery can quickly relieve pressure on surrounding structures caused by large pituitary adenomas. However, over the long-term, only around 60% of patients achieve normal levels of growth hormone and IGF-I after surgery. Therefore medication or radiation may also be required for residual disease or relapse.
Long-term follow-up is required to check for relapse and potential cardiovascular, respiratory, and malignant complications.