Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Anila Kapadia, Dermatology Registrar, York Teaching Hospital NHS Foundation Trust, United Kingdom. Advisor to the content: Dr. Calum Lyon, Consultant Dermatologist, York Teaching Hospital NHS Foundation Trust, United Kingdom. Copy Editor: Clare Morrison. June 2014.
Introduction
Clinical features
Difference from epidermoid cyst
Histological findings
Treatment
A trichilemmal cyst, also known as a pilar cyst, is a keratin-filled cyst that originates from the outer hair root sheath. Keratin is the protein that makes up hair and nails. Trichilemmal cysts are most commonly found on the scalp and are usually diagnosed in middle-aged females. They often run in the family, as they have an autosomal dominant pattern of inheritance (ie, the tendency to the cysts can be is passed on by a parent to their child of either sex, and the child has a 1 in 2 likelihood of inheriting it).
Trichilemmal cysts may look similar to epidermoid cysts and are often incorrectly termed sebaceous cysts. Trichilemmal cysts present as one or more firm, mobile, subcutaneous nodules measuring 0.5 to 5 cm in diameter. There is no central punctum, unlike an epidermoid cyst. A trichilemmal cyst can be painful if inflamed.
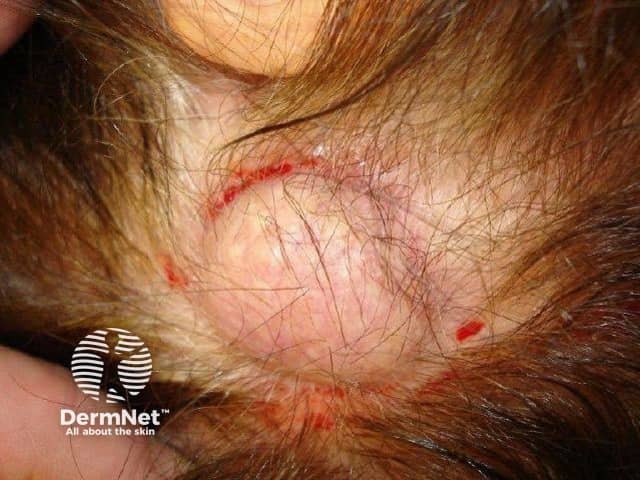
Image from Dr Calum Lyon
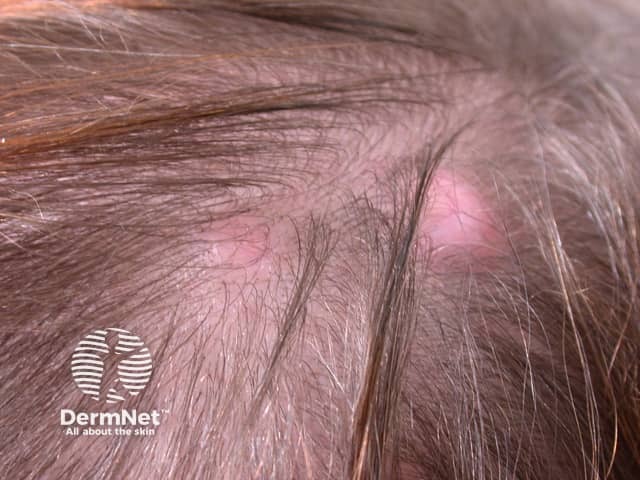
Pilar cysts
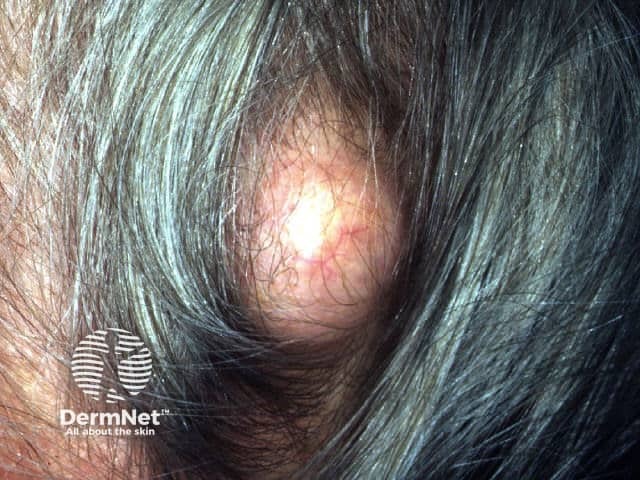
Pilar cyst
The pathology of a trichilemmal cyst is characteristic. The wall of the cyst is stratified squamous epithelium (skin) that has a palisaded outer layer, which resembles the that of outer root sheath of a hair follicle. The inner layer does not have a granular layer. The cyst shows very dense pink keratin on haematoxylin and eosin staining.
It is not necessary to remove trichilemmal cysts if they are not causing symptoms. However, incision and drainage under local anaesthesia provide comfort, and elective excision before rupture prevents scarring.
Surgical treatment involves either of the following methods:
Acute inflammation after rupture is often misdiagnosed as a bacterial infection. Antibiotics are of little value unless an actual infection is present.