Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated February 2016.
Introduction - cysts
Introduction - pseudocysts
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Prevention
Outlook
A cyst is a benign, round, dome-shaped encapsulated lesion that contains fluid or semi-fluid material. It may be firm or fluctuant and often distends the overlying skin. There are several types of cyst. The most common are described here.
Cysts that are not surrounded by a capsule are better known as pseudocysts. These commonly arise in acne.
Cysts are very common, affecting at least 20% of adults. They may be present at birth or appear later in life. They arise in all races. Most types of cyst are more common in males than in females.
The cause of many cysts is unknown.
An epidermoid cyst is also called a follicular infundibular cyst, epidermal cyst, and keratin cyst.
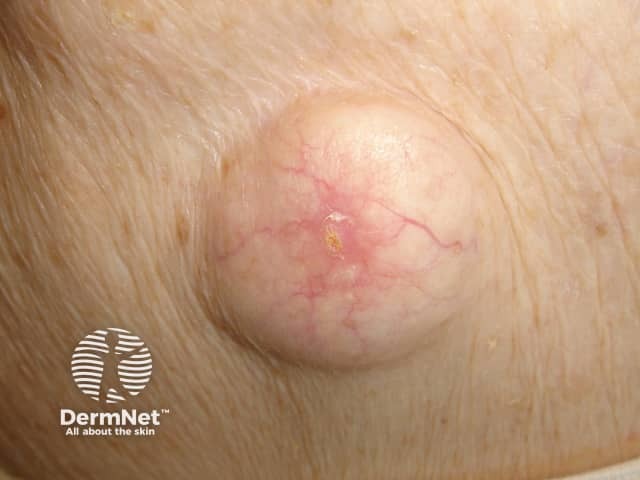
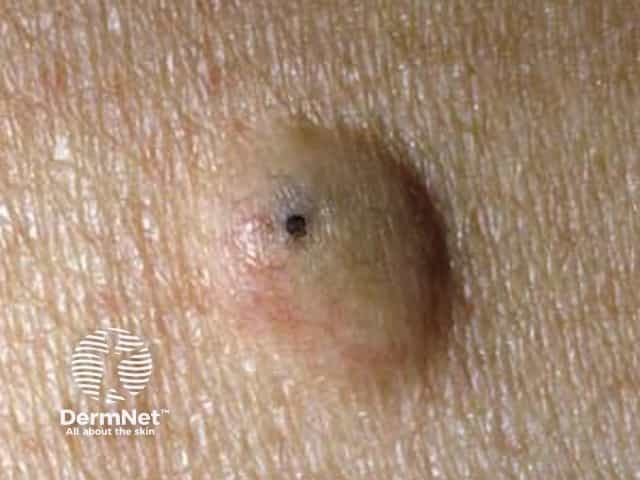
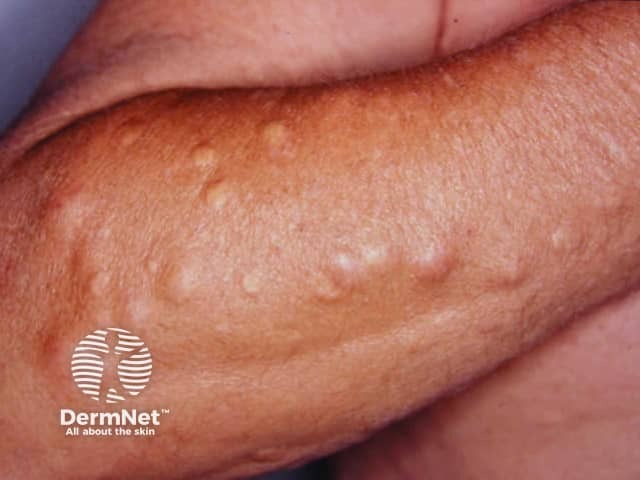
Gardner syndrome
See more images of epidermoid cysts.
A trichilemmal cyst is also called pilar cyst.
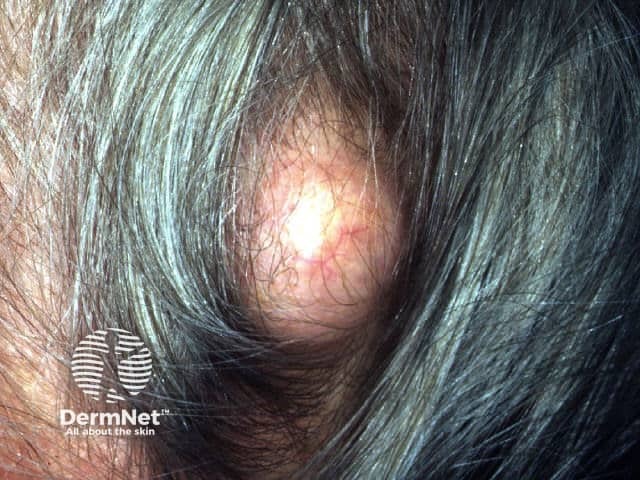
Pilar cyst
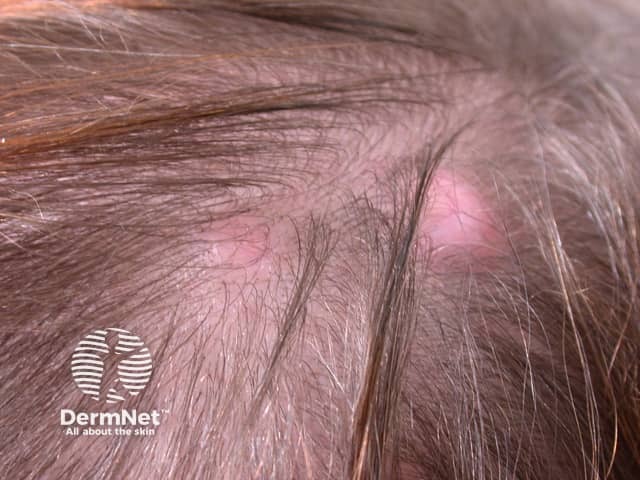
Pilar cysts
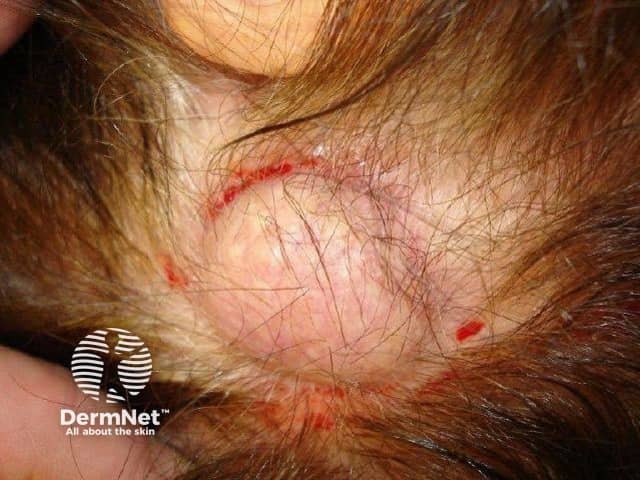
Pilar cyst
See more images of epidermoid cysts.
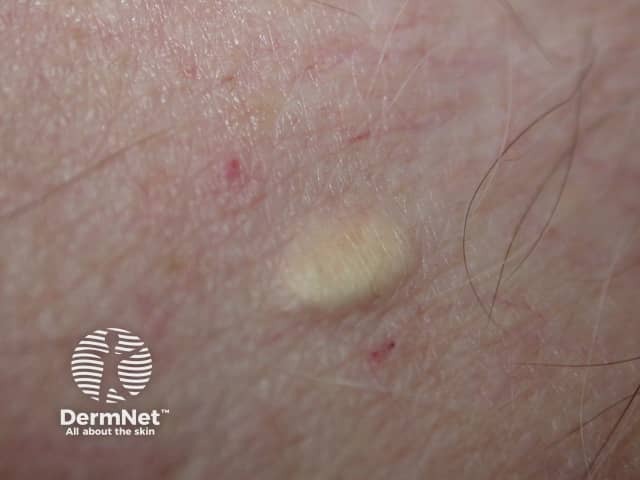
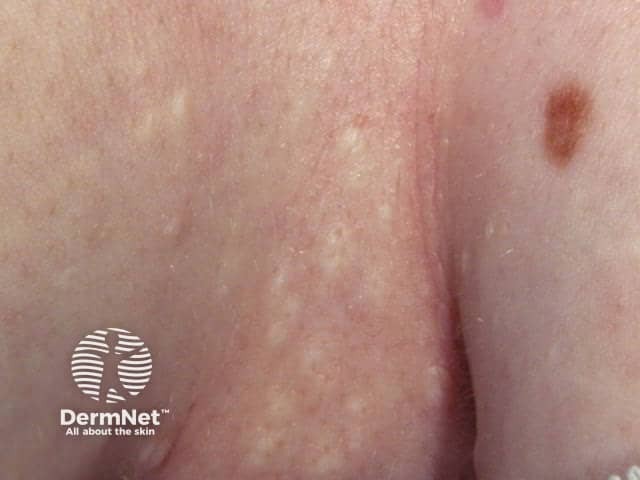
Steatocystoma multiplex
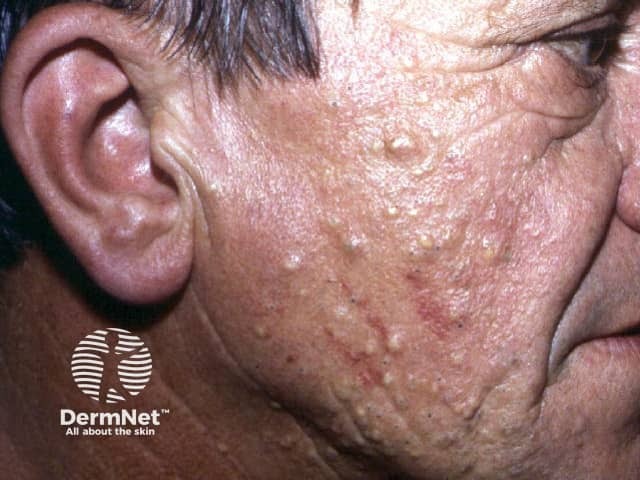
Steatocystoma multiplex
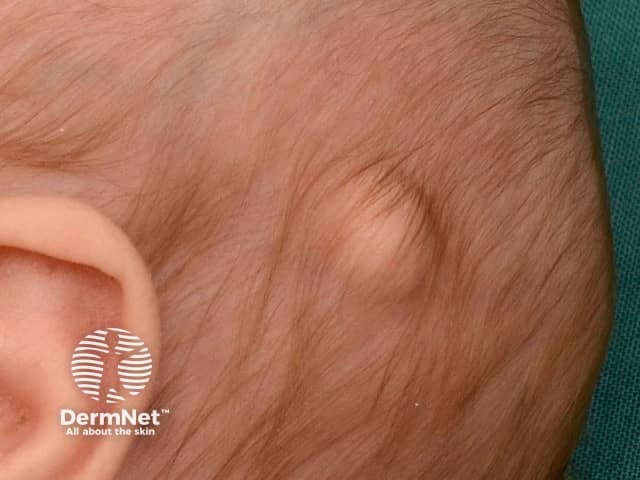
Dermoid cyst
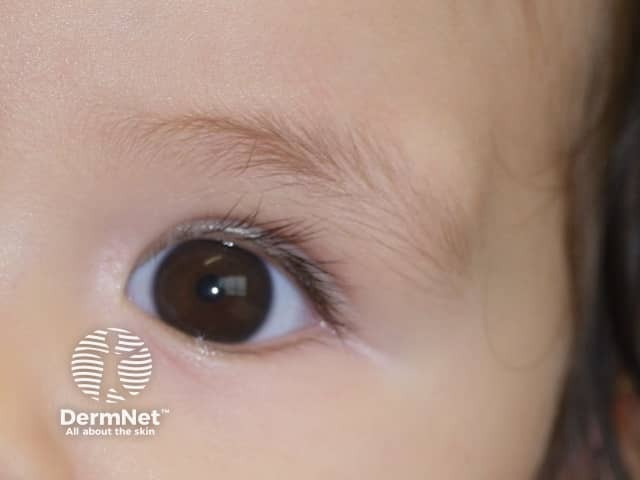
Dermoid cyst
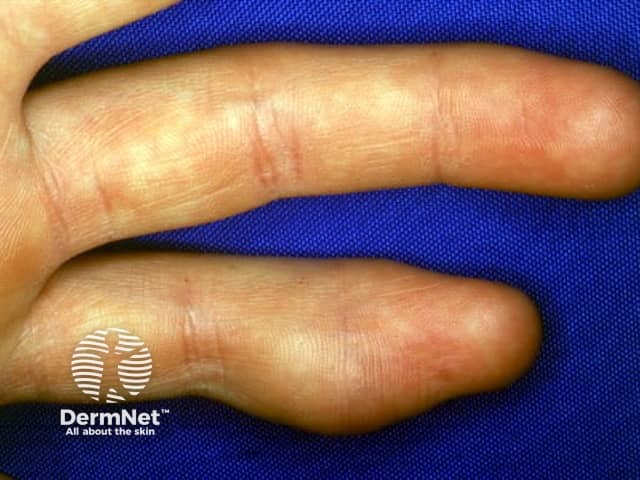
Dermoid cyst
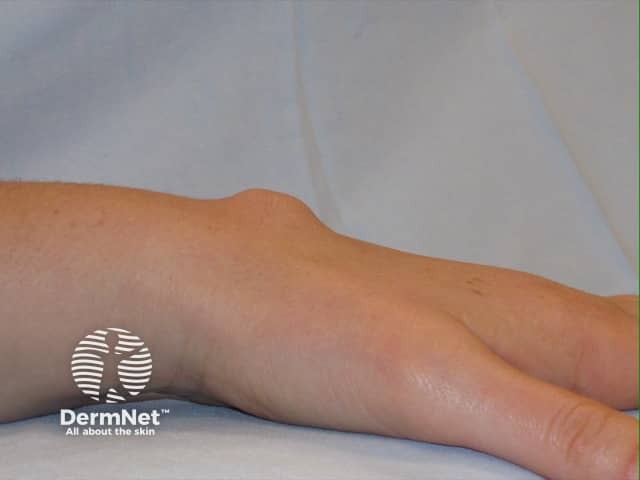
Ganglion cyst
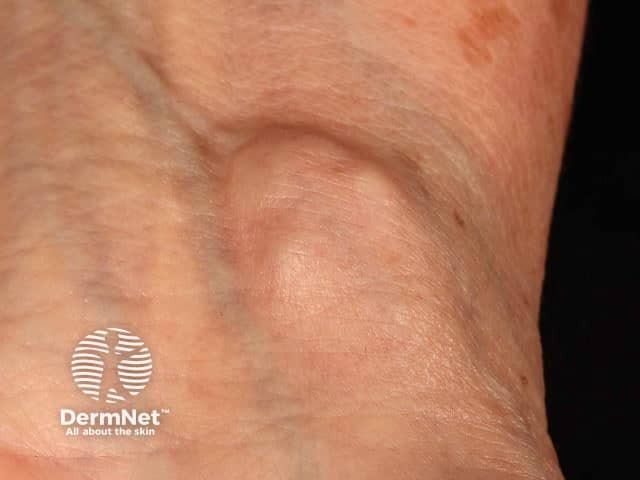
Ganglion cyst
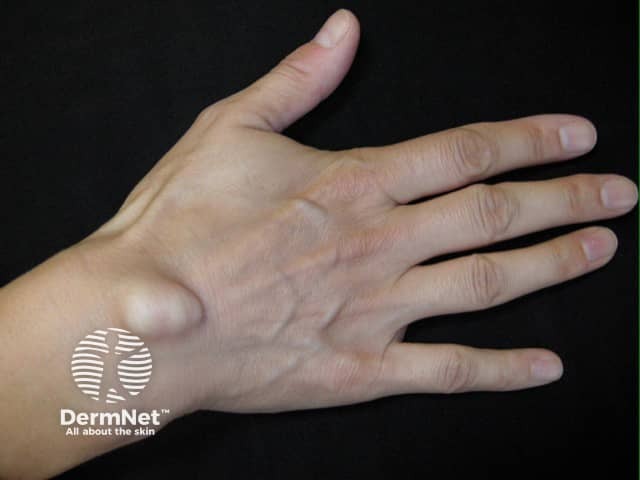
Ganglion cyst
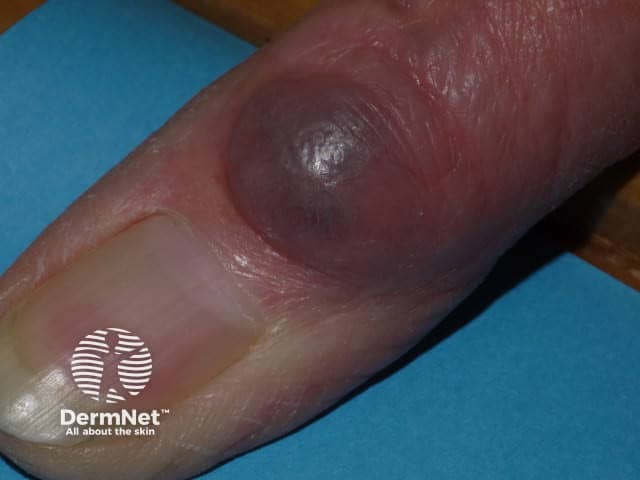
Digital myxoid cyst
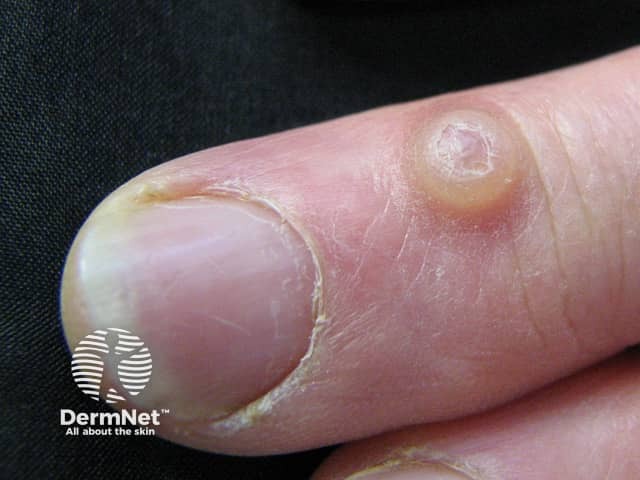
Myxoid cyst
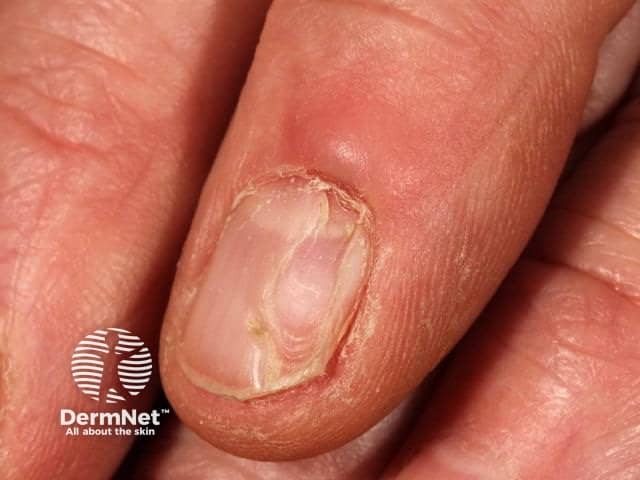
Digital myxoid cyst
See more images of digital myxoid pseudocysts.
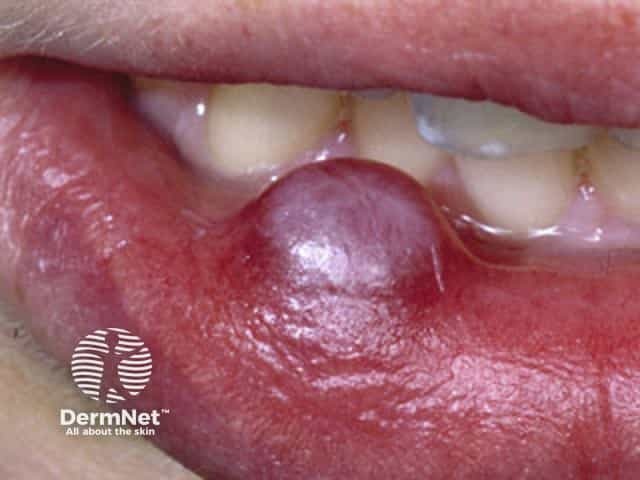
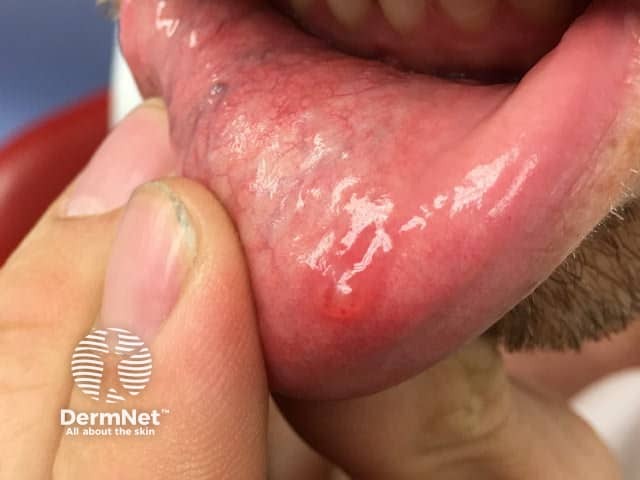
Mucocoele of the lip
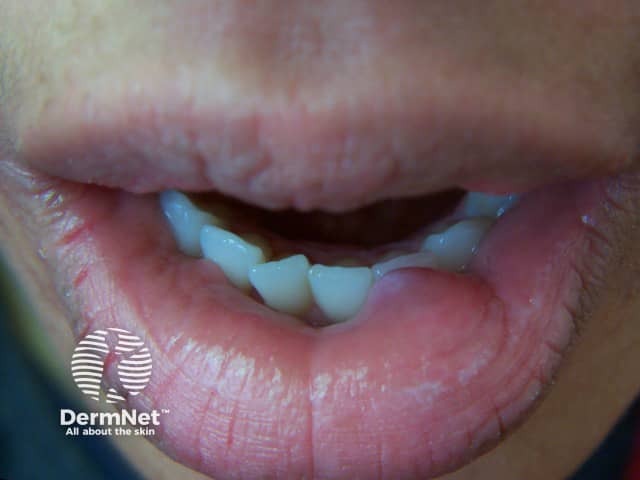
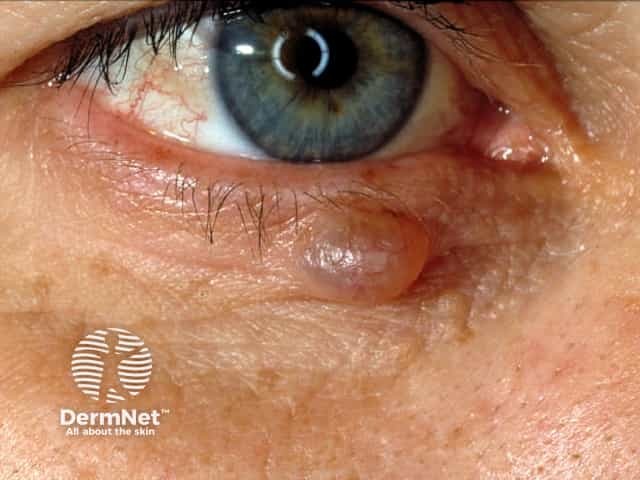
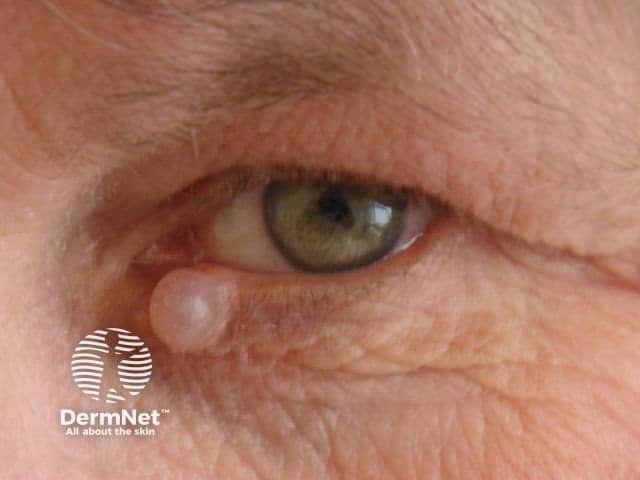
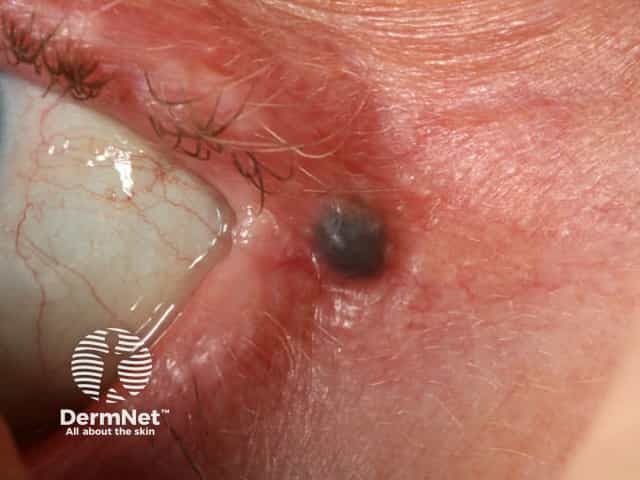
More images of hidrocystoma of the eyelid.
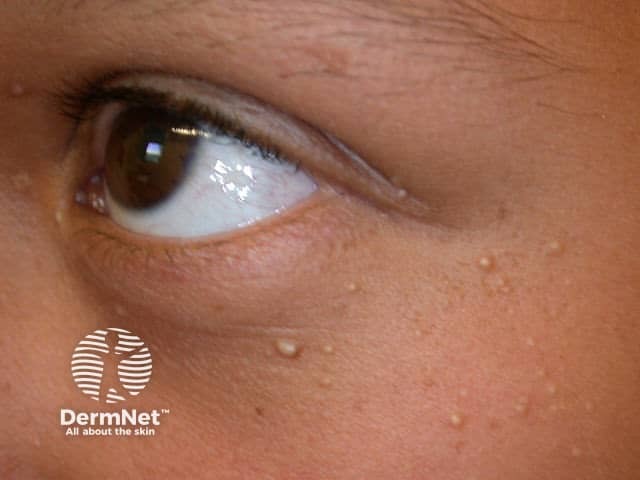
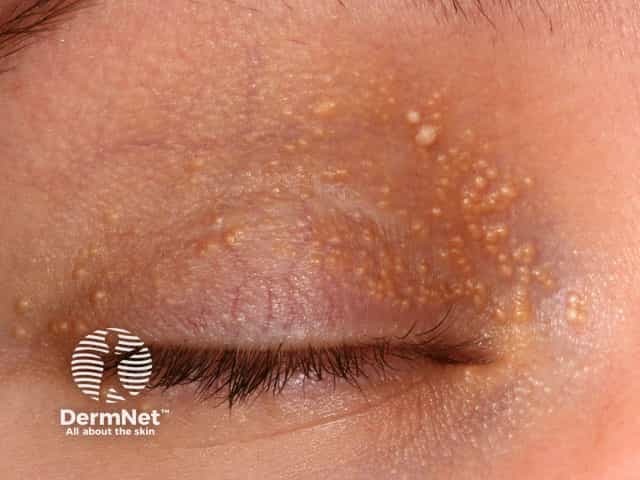
Eyelid milia
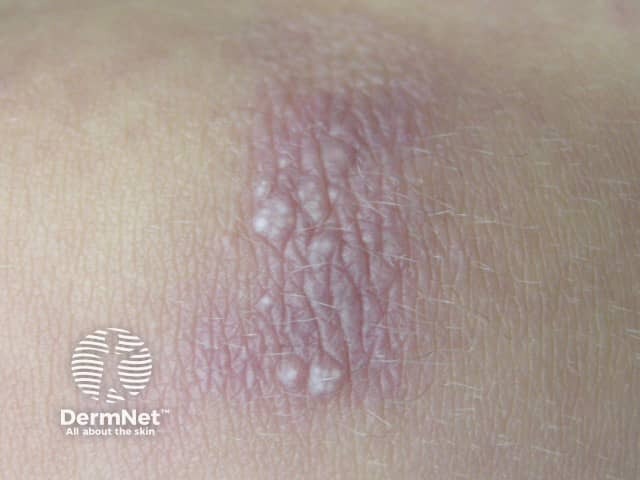
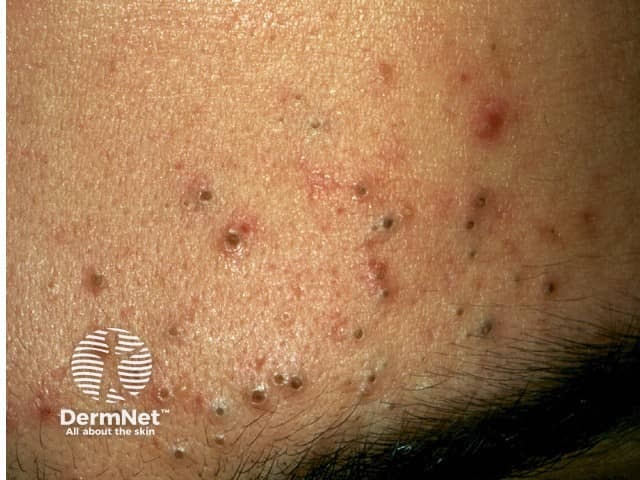
Open comedones
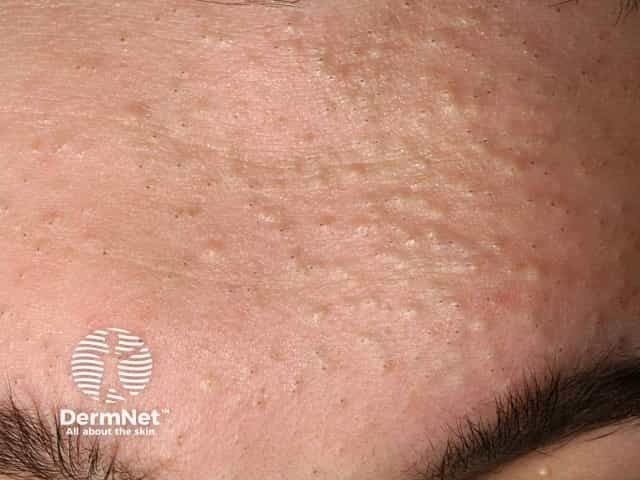
Closed comedones
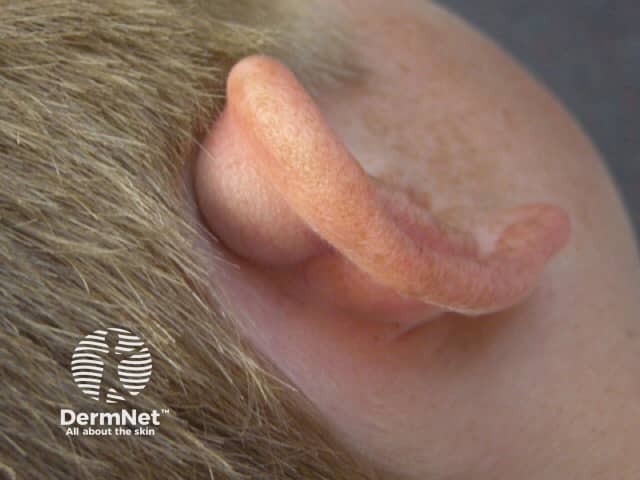
Auricular pseudocyst
Cysts have typical clinical characteristics. When a cyst is surgically removed, it should undergo a histological examination. The type of lining of the wall of the cyst and the cyst contents help the pathologist classify it.
An asymptomatic epidermoid cyst does not need to be treated. In most cases, an attempt to remove only the contents of a cyst is followed by recurrence. If desired, cysts may be entirely excised. Recurrence is not uncommon, and re-excision may be surgically challenging.
Inflamed cysts are sometimes treated with:
Unknown.
Cysts generally persist unless surgically removed.