Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley Dermatologist, Hamilton, New Zealand, 1999. Reviewed by Vanessa Ngan, Staff Writer, February 2014. DermNet Revision August 2021
Introduction
Demographics
Causes
Clinical features
Complications
Differential diagnoses
Diagnosis
Treatment
Outlook
Nodulocystic acne is a severe form of acne affecting the face and upper trunk, characterised by nodules and cysts that typically resolve with scarring.
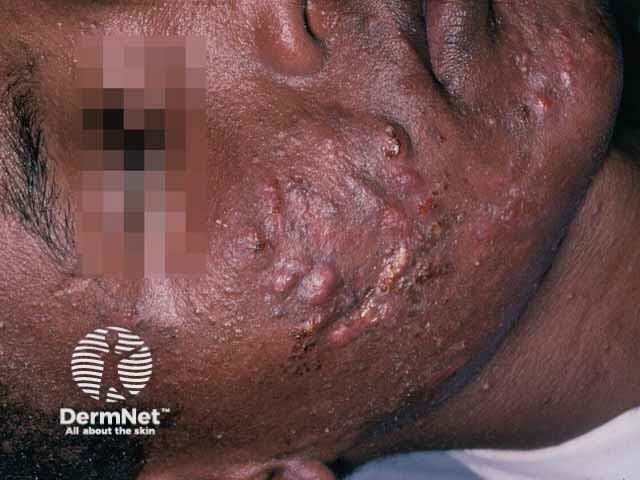
Nodulocystic acne: face
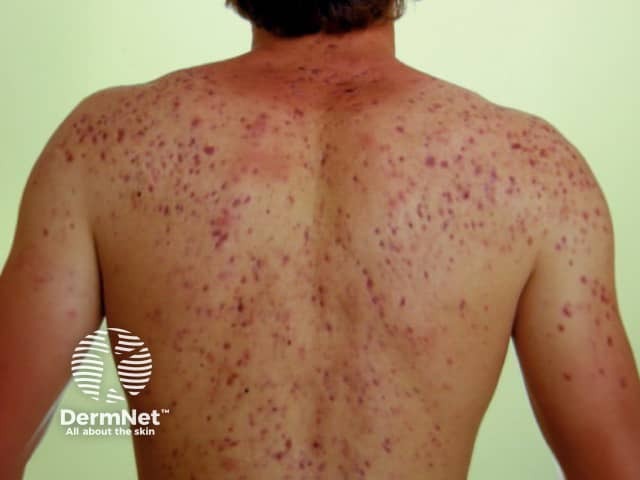
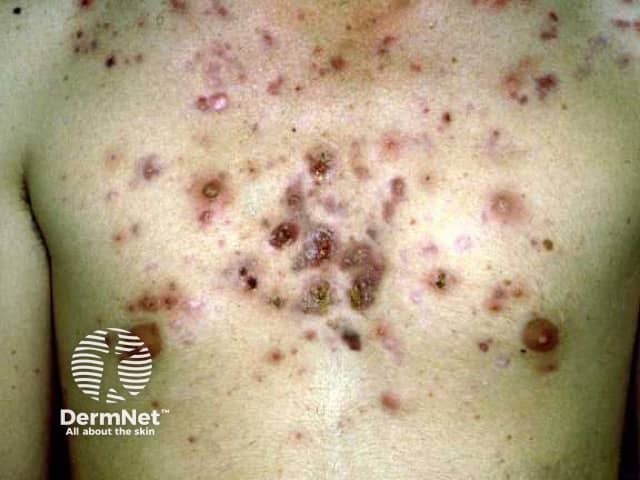
Nodulocystic acne
Nodulocystic acne is usually a disorder of adolescence and early adult life seen most commonly in males. However there is a rare juvenile form with onset before 6 years of age, also with a male predominance.
No studies have shown an increased incidence in specific racial groups.
Nodulocystic acne is associated with other follicular occlusion disorders particularly hidradenitis suppurativa.
The acne conglobata variant of nodulocystic acne is the 'A' in a number of syndromes including: SAPHO, PASH, PASS, and PAPA.
The pathogenesis of acne is believed to be multifactorial involving increased sebaceous gland activity, abnormal keratinisation of follicles, the action of microorganisms, and subsequent inflammation.
Specific risk factors for nodulocystic acne include:
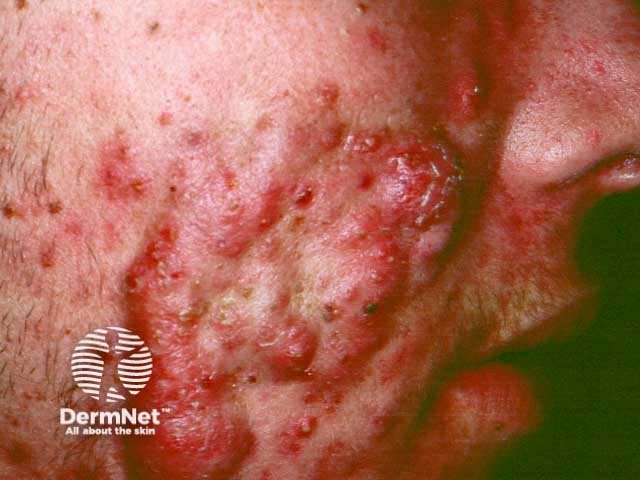
Nodulocystic acne: cheek
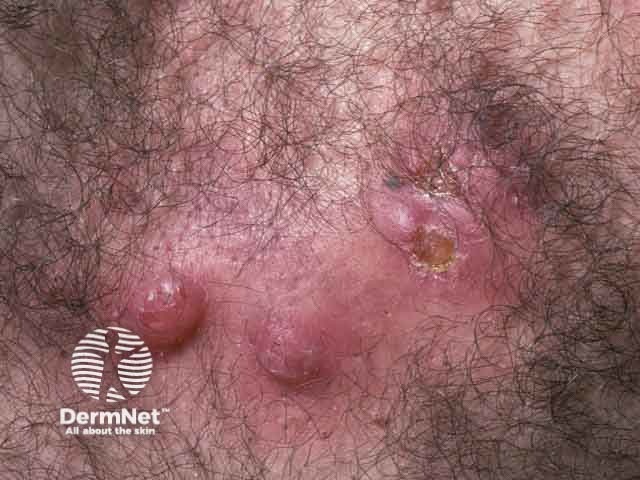
Nodulocystic acne: chest
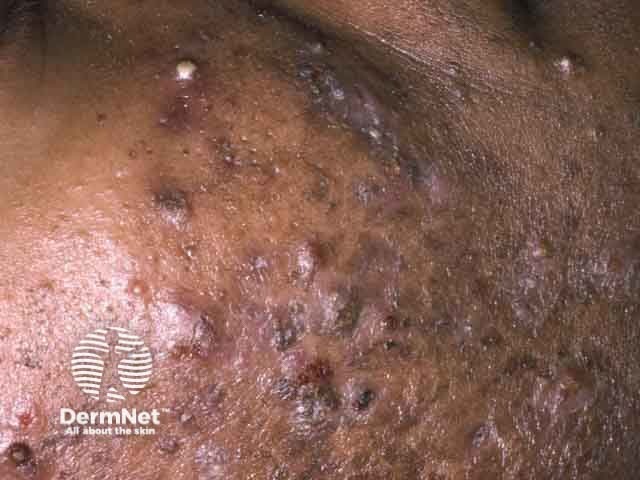
Nodulocystic acne: face
More images of acne ...
Acne conglobata is a rare severe form of nodulocystic acne. It presents with groups of multiple comedones and inflammatory papules, pustules, and nodules involving the trunk, limbs, and buttocks. Interconnecting abscesses and draining sinuses become secondarily infected causing pain and malodour. Healing is slow, leaving unsightly hypertrophic and atrophic scars. Acne conglobata is often very persistent, lasting into the 30s or 40s.
Postinflammatory hyperpigmentation and keloid scarring are common complications of nodulocystic acne in skin of colour.
Nodulocystic acne is a clinical diagnosis. Hormone studies may be considered in the presence of suggestive clinical features.
Topical treatment is usually ineffective for nodulocystic acne.
The recommended treatment is oral isotretinoin which should be commenced early to prevent scarring. Treatment is required for at least five months, and further courses are sometimes necessary. Intralesional steroids following cyst drainage, can be used for individual persistent or large inflammatory nodules or cysts.
Patients with acne conglobata often need additional treatments, such as:
Nodulocystic acne typically persist into adult life. Unless treated early and effectively, nodulocystic acne results in scarring particularly on the torso.