Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Sarah Hill, Dermatology Registrar, Waikato Hospital, 2006.
SAPHO syndrome is characterised by any combination of:
The cause is unknown.
Other skin lesions seen in SAPHO syndrome include: hidradenitis suppurativa and dissecting cellulitis of the scalp.
The skin lesions in SAPHO syndrome are characterised on skin biopsy by collections of inflammatory cells, known as neutrophilic pseudoabscesses.
Bony involvement mostly affects the breast bone (sternum), resulting in decreased mobility due to pain, tenderness and swelling. The collar bones (clavicles) are also frequently enlarged on X-ray. Bone biopsy also reveals abscesses, known as sterile osteomyelitis.
SAPHO syndrome is classified along three different spectrums.
Prevalence of CRMO is estimated at 0.04% whilst the other entities are rarer.
SAPHO syndrome is suspected when a patient presents with a pustular skin disease in association with rheumatic pain.
Magnetic resonance imaging (MRI scan) shows inflammation of the bone marrow or joints at characteristic sites such as the collar bone, breast bone, pelvis, heel, and lower jaw.
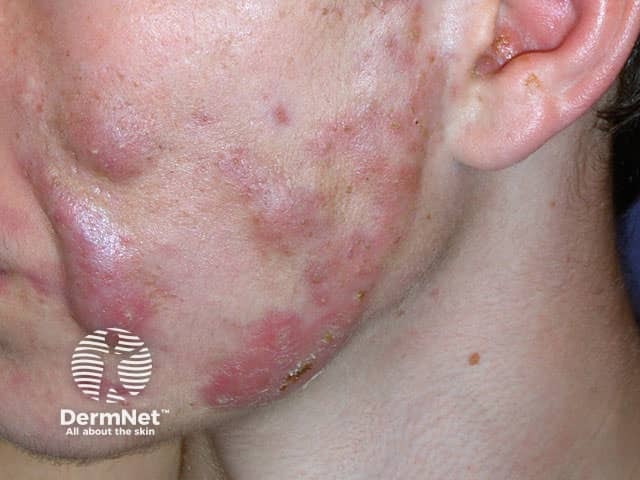
Acne fulminans
SAPHO has no specific drug treatment. It can be a chronic condition but eventually self-heals.
A rheumatologist may manage the joint symptoms, often prescribing nonsteroidal anti-inflammatory drugs or sulfonamides such as sulfasalazine.
A dermatologist may use vitamin A derivatives (oral retinoids) to treat the acne (isotretinoin) and the palmoplantar pustulosis (acitretin).
Other drugs that may be used include: