Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Sonam Vadera, Medical Student, University College London, London, United Kingdom. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. October 2017. Revised February 2021.
Introduction Demographics Spread Clinical features Complications Diagnosis Treatment Prevention
Human papillomaviruses (HPV) form a large family of DNA viruses that infect only human skin keratinocytes and mucosal epithelial cells. The family is divided into types based on DNA hybridisation. Specific HPV types preferentially infect epithelial cells and tend to be sexually transmitted.
Infection with low-risk types of HPV, such as types 6 and 11, are often asymptomatic or cause anogenital warts, mucosal (oral, conjunctival) squamous cell papillomas, and juvenile-onset respiratory papillomatosis.
There are at least 13 high-risk types of sexually transmitted HPV which are associated with precancerous squamous intraepithelial lesions and cancer (squamous cell carcinoma).
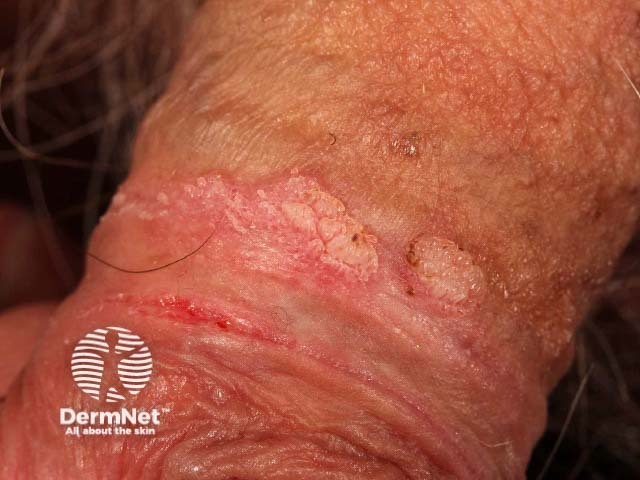
Anogenital wart
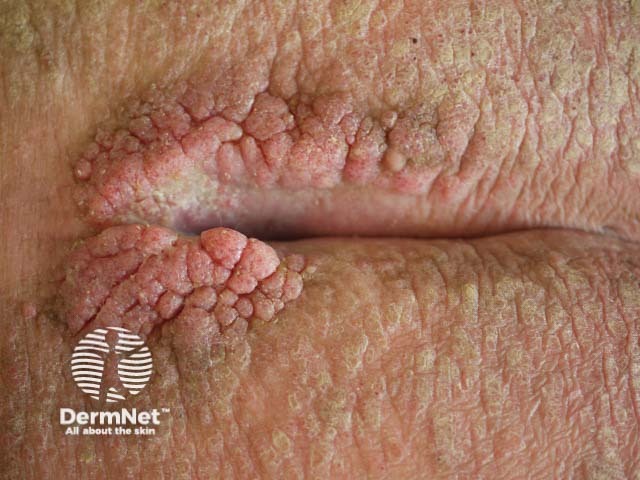
Anogenital wart
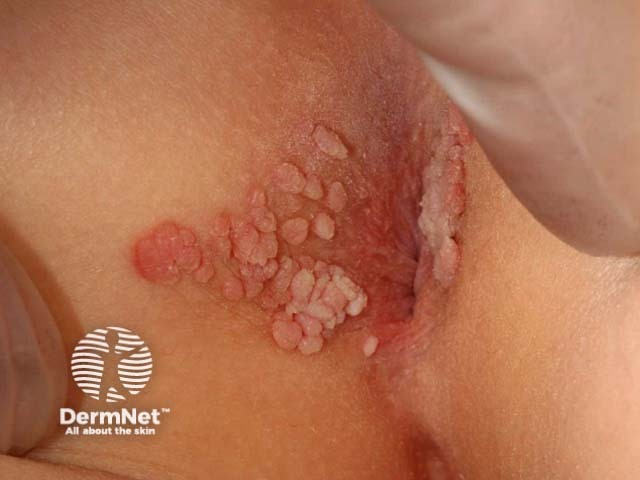
Anogenital wart
see also Genital wart images
Sexually acquired HPV types infect both sexes and all genders. However there does appear to be a male predominance.These viruses can be highly infectious and spread rapidly.
Risk factors for infection include:
Infants and young children can develop anogenital HPV-related lesions due to cutaneous and mucosal HPV types acquired during birth or from the hands of carers.
Epithelial HPV is typically spread by surface-to-surface contact during vaginal, anal and oral sexual intercourse. HPV can also be transmitted vertically, from mother to child during vaginal delivery.
Although HPV is the most common sexually transmitted virus infection. It is often asymptomatic and resolves by itself.
Persistence of specific HPV types can lead to:
High-risk HPV types 16 and 18 are thought to be responsible for at least 70% of precancerous and cancerous disease of the anogenital area.
Squamous intraepithelial lesions (SILs), also known as intraepithelial neoplasia (IN), are classified by the affected site. Types of SIL include:
Infection with high-risk HPV types can lead to invasive squamous cell carcinomas of the anus and anal canal, oropharyngeal tract (oral cancer), vagina, vulva, and penis. The most common invasive cancer associated with HPV is cervical cancer.
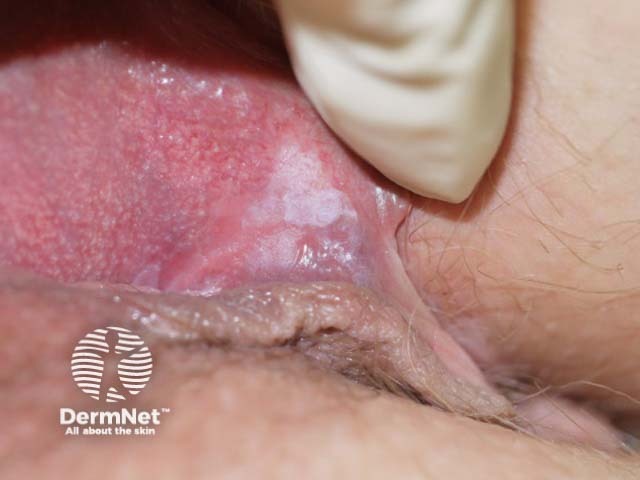
Vulval high-grade squamous intraepithelial lesion
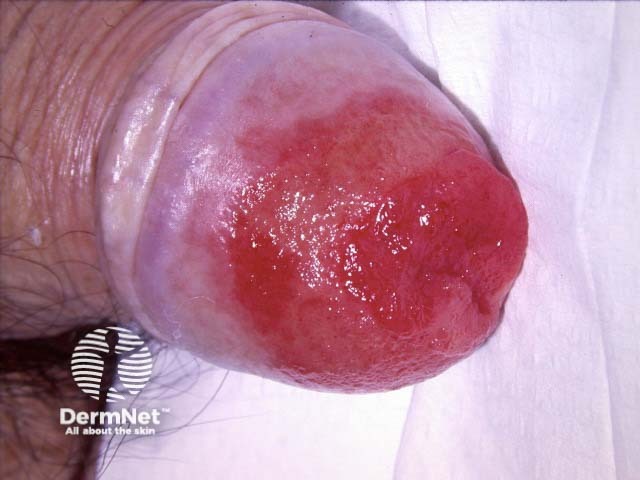
Penile high-grade squamous intraepithelial lesion
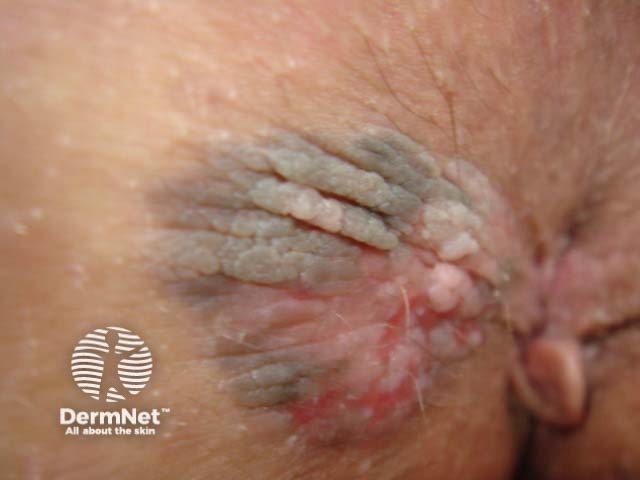
Perianal high-grade squamous intraepithelial lesion
see also Vulval intraepithelial neoplasia images, Penile epithelial neoplasia images
Most benign lesions caused by HPV infection can be diagnosed clinically. Cytology can be used to diagnose mucosal HPV infection when typical koilocytes ('hollow cells') with hyperchromatic or double nuclei, abundant cytoplasm, and a perinuclear halo are detected.
Other methods of diagnosing HPV infection include:
Treatment of anogenital warts, precancerous, and cancerous lesions may include:
Koilocytes and viral DNA can often be detected some distance away from the clinical and histologically delineated lesion. Recurrence is therefore common after all treatments.
Condoms are an important means to reduce the transmission of HPV. However, they do not completely eliminate the risk.
Most sexually acquired HPV infection can now be prevented by vaccination during childhood before the onset of sexual activity. [see Vaccines against human papillomavirus]