Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Sabrina Sapsford, Dermatology Research Fellow, University of Auckland, New Zealand (2023). Minor update November 2025.
Previous contributors: Dr Anthony Yung, Dermatologist (2014); Dr Amanda Oakley, Dermatologist (2014)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Mastocytosis is a diverse group of disorders characterised by the expansion and accumulation of mast cells in one or more organ systems. It can affect the skin, bone marrow, liver, spleen, gastrointestinal tract, or lymph nodes.
In 2022, the World Health Organisation (WHO) categorised three main types of mastocytosis:
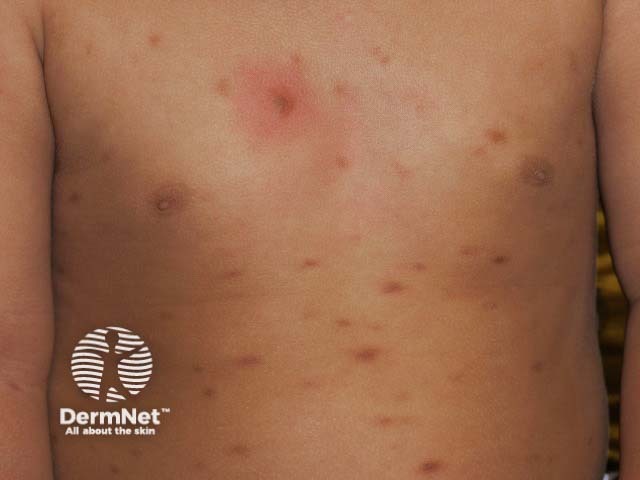
Cutaneous mastocytosis in an infant - yellow-brown macules over the chest and back. The chest lesion has urticated 5 minutes after rubbing (Darier sign)
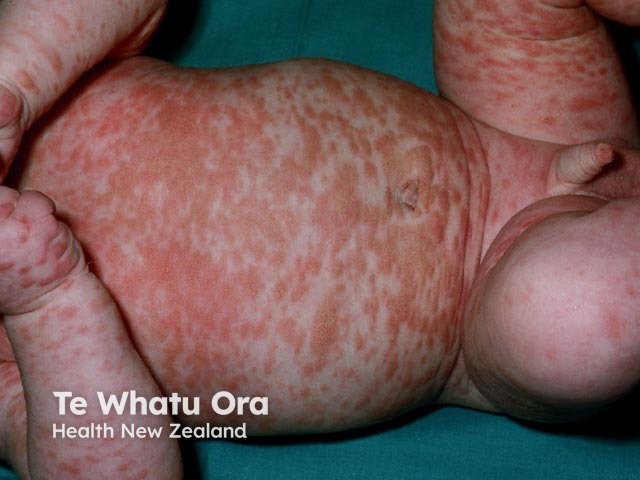
Extensive diffuse mastocytosis in an infant

Maculopapular cutaneous mastocytosis (urticaria pigmentosa); red-brown maculopapular lesions on the leg
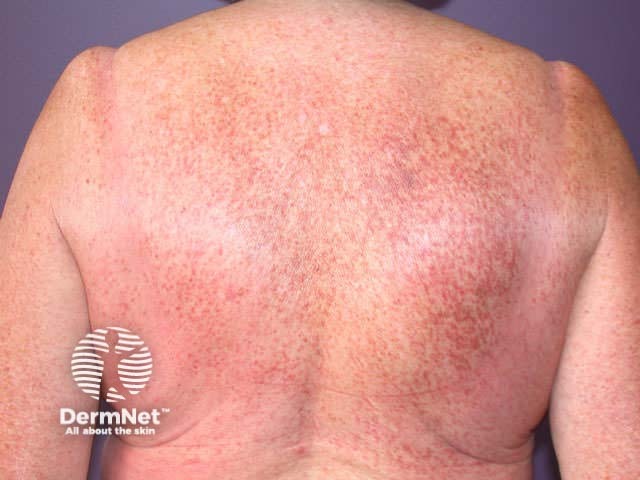
Telangiectasia in maculopapular cutaneous mastocytosis

Dermoscopy showing prominent telangiectasia in telangiectatic maculopapular cutaneous mastocytosis
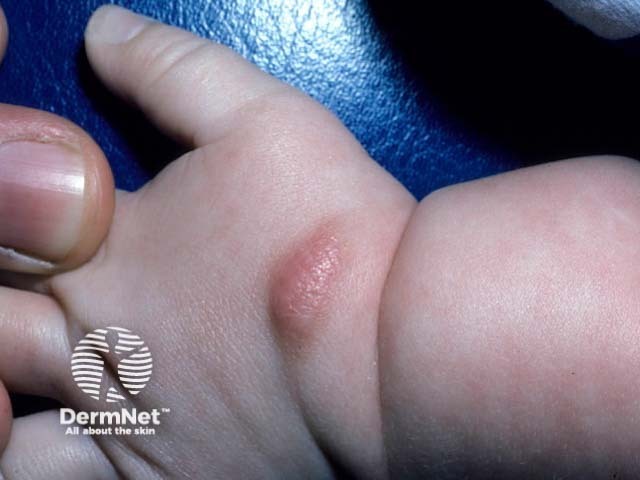
Solitary mastocytoma on a toddler’s hand
See more images of cutaneous mastocytosis
Mastocytosis can occur at any age, although some types are more common in particular age groups. Females have a slightly higher risk of developing mastocytosis than males. In most cases, there is no family history of mastocytosis.
Cutaneous mastocytosis is most commonly diagnosed in childhood. It can be present at birth and around 50% of children develop skin lesions before they are 6 months old. It usually resolves by puberty but in some cases may persist. Urticaria pigmentosa (maculopapular cutaneous mastocytosis) more commonly presents in adulthood and may be persistent and slowly progressive.
Systemic mastocytosis is usually diagnosed in adulthood after the second decade of life.
Mastocytosis is caused by a mutation of the KIT gene on the 4q12 chromosome. This results in too many mast cells being produced.
Mast cells contain chemicals that mediate inflammation (eg, via histamine, leukotriene C4, prostaglandins, tryptase, TNFα, and IL-8). Upon activation, mast cells release these mediators, resulting in localised itching, swelling, redness and sometimes blistering of the skin. This can be a normal reaction; for example, to insect bites. However, in mastocytosis, this process becomes uncontrolled.
In rare cases, the KIT genetic defect is inherited. In most cases, it is sporadic, with no family history.
There are three main forms of cutaneous mastocytosis:
In all forms, rubbing or scratching an area of skin affected by mastocytosis results in redness, swelling, itching, and occasionally blistering within a few minutes (Darier sign).
See images of cutaneous mastocytosis
Types of cutaneous mastocytosis |
Features |
Maculopapular cutaneous mastocytosis |
|
Diffuse cutaneous mastocytosis |
|
Mastocytoma |
|
Patients usually have skin lesions, although these may be smaller than those of childhood-onset cutaneous mastocytosis. Evidence of other organ involvement may include:
Depending on clinical presentation, systemic mastocytosis can be classified as indolent (slow expansion), smouldering (premalignant), or aggressive. It can be limited to the bone marrow (bone marrow mastocytosis). In rare cases, it may be associated with haematological neoplasia or progress to mast cell leukaemia.
In darker skin tones:
Skin biopsy findings in all Fitzpatrick skin types would demonstrate increased mast cell numbers.
It is important to differentiate between cutaneous and systemic mastocytosis. A full history should be taken, along with skin and abdominal examination and checking for lymphadenopathy.
Cutaneous mastocytosis is usually diagnosed by its clinical appearance and positive Darier sign, in the absence of systemic symptoms and signs.
Patients with a solitary mastocytoma generally require no further workup.
Skin biopsy and histology can be helpful for confirmation of cutaneous mastocytosis. This may show aggregates of mast cells with positive staining for CD117 filling the papillary dermis, and may have positive staining for tryptase. See also: Maculopapular cutaneous mastocytosis pathology.
Systemic mastocytosis is diagnosed when a patient has a positive bone marrow biopsy or other extracutaneous biopsy. Specific laboratory and genetic tests may also support the diagnosis.
Relevant tests include:
Major criteria |
|
|
Minor criteria |
|
|
*Updated by WHO, 2022
Many forms of cutaneous mastocytosis without symptoms require no treatment.
Avoidance of triggers for histamine release/ mast cell degranulation is important in patients with symptomatic mastocytosis.
Special care should be taken with patients with diffuse cutaneous or systemic mastocytosis, especially if they have elevated serum tryptase, prior to receiving anaesthetic or having imaging that requires radio-contrast.
Physical agents:
Emotional factors:
Drugs:
Venoms:
Others:
An adrenaline (epinephrine) autoinjector (eg, EpiPen®) is recommended in patients with previous anaphylaxis, high tryptase, or significant cutaneous disease.
Specific treatments for patients with cutaneous mastocytosis may include:
Systemic mastocytosis treatments include:
There is no known way to prevent mastocytosis.
Cutaneous mastocytosis is usually self-limiting and benign. If symptomatic, the main aims of management are symptom control and trigger avoidance to prevent anaphylaxis.
In adults with systemic disease, treatment is more complex and prognosis varies. A multidisciplinary team of haematologists, dermatologists, immunologists, and specialist nurses are often involved, as well as the patient’s general practitioner or primary care physician.