Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Daniel Mazzoni, Basic Physician Trainee, Royal Brisbane and Women’s Hospital, Brisbane, Queensland, Australia; Nicolas Anning, Clinical Pharmacist, Royal Brisbane and Women’s Hospital, Brisbane, Queensland, Australia. Copy edited by Gus Mitchell. November 2020.
Introduction
How it works
Clinical uses
Uses
Adverse effects
Cutaneous adverse effects
Beta-blockers are medications that antagonize the effects of adrenaline and noradrenaline by blocking adrenergic receptors.
Beta-blockers are used mainly for the treatment of cardiovascular diseases and glaucoma. Their use in dermatology is increasing for a variety of conditions.
Two classes of beta-blocker are currently used in clinical practice: cardio-selective (beta-1 receptor-selective) and non-selective (beta-1, beta-2, and/or alpha-1 receptor) beta blockers.
Blockade of cardiac beta-1 adrenergic receptors results in decreased heart rate and blood pressure. Blockade of beta-2 adrenergic receptors causes the relaxation and dilatation of peripheral blood vessels, resulting in decreased blood pressure.
Commonly used examples of cardio-selective beta-blockers include:
Non-selective beta-blockers include:
Beta-blockers may be administered orally (immediate or controlled release), intravenously, or topically as eye drops.
The current approved uses of beta-blockers in medicine are summarised below.
Metoprolol, bisoprolol, and carvedilol are prescribed for cardiovascular disease.
Propanolol is used for anxiety, essential tremors, migraine prophylaxis, and haemangiomas.
Ophthalmic timolol drops are applied topically onto the eye for glaucoma. Use of topical timolol in dermatology is off-label.
Oral propranolol is FDA-approved for large or life-threatening infantile haemangioma (see Propranolol for infantile haemangioma). Topical timolol is used for smaller haemangiomas.
Small case series have demonstrated improvement in the flushing and persistent erythema of rosacea using oral carvedilol. Topical timolol seems to be less effective.
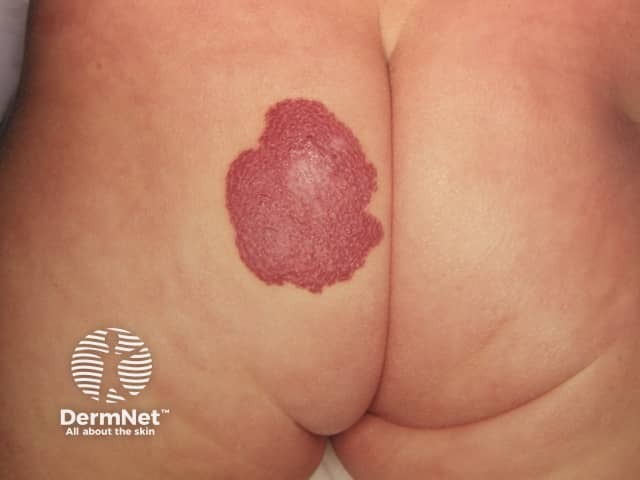
Infantile haemangioma
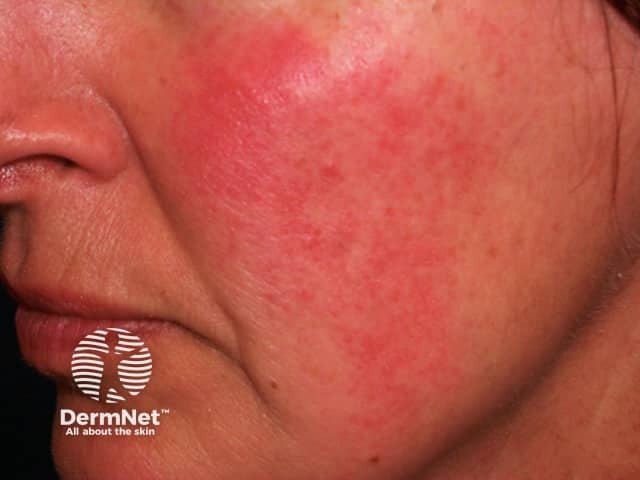
Rosacea
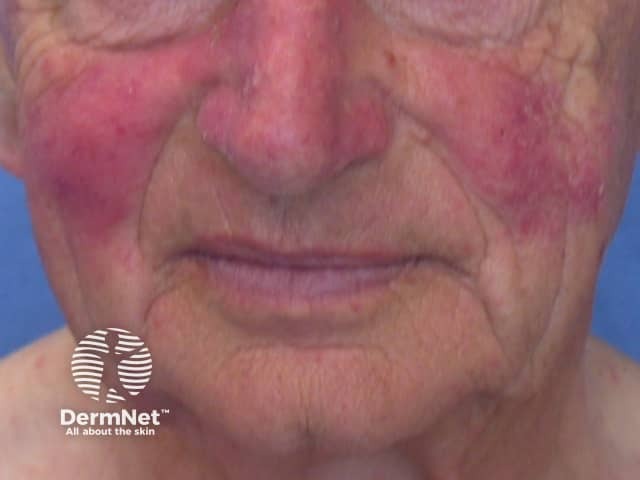
Rosacea
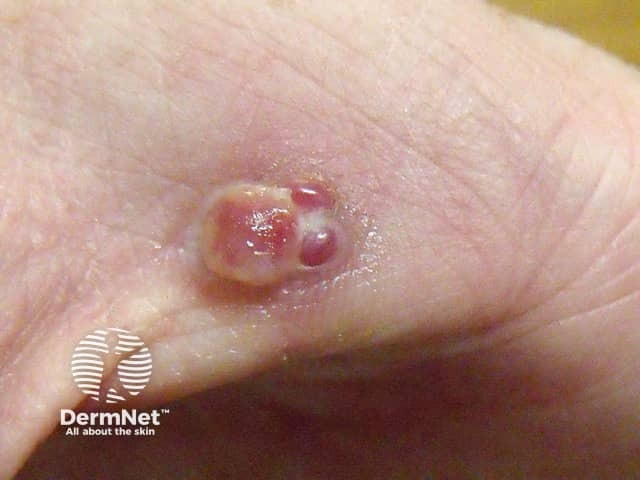
Topical timolol has been reported to clear pyogenic granuloma in most, but not all, cases.
A small number of cases have described successful treatment of Kaposi sarcoma using topical timolol in both HIV-positive and HIV-negative cases.
Several case series using topical timolol have reported improved wound healing in chronic diabetic and venous leg ulcers.
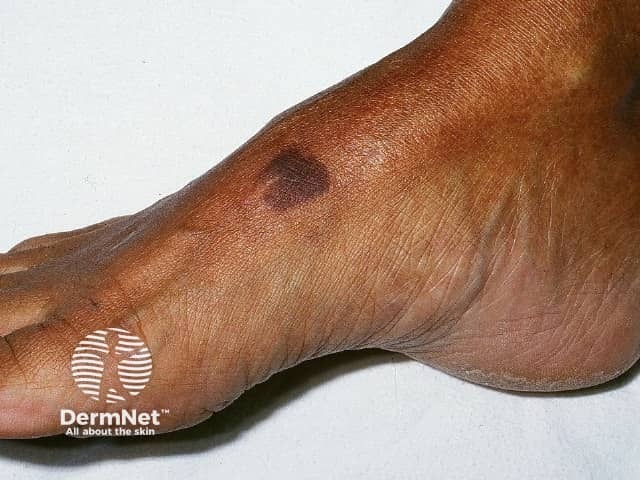
Kaposi sarcoma
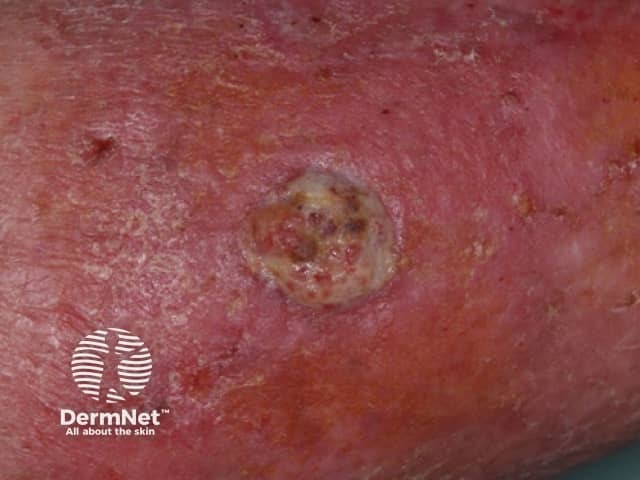
Leg ulcer
The side effects of beta-blockers occur primarily due to their anti-adrenergic effect.
Common adverse effects of beta blockers include:
Adverse effects may also occur if regular beta-blocker therapy is abruptly ceased. This is due to beta-blockers inducing up-regulation of beta-adrenergic receptors in the body.
Abrupt withdrawal of beta-blockers can induce:
Beta-blockers are a well-recognised trigger to exacerbate or precipitate psoriasis.
Exacerbation of Raynaud phenomenon is commonly reported in patients taking a beta-blocker.
Alopecia due to beta-blockers is a telogen effluvium, a reversible thinning of the hair.
Other reported adverse reactions to beta-blockers include:
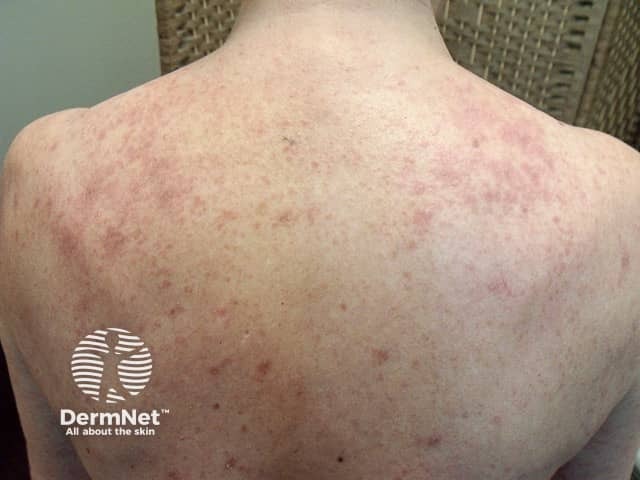

Nail psoriasis: onycholysis and pitting