Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand; Dr Amy Stanway, Dermatology Registrar, Nottingham, UK. Revised: Dr David Lim, Dermatology Registrar, Auckland, New Zealand. August 2011. Updated: Dr Richa Tripathi, Consultant Dermatologist, Grande International Hospital, Kathmandu, Nepal. Copy edited by Gus Mitchell. October 2021
Introduction
Demographics
Causes
Clinical features
Dermoscopy
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Juvenile xanthogranuloma is a type of non-Langerhans cell histiocytosis usually limited to the skin in very young children.
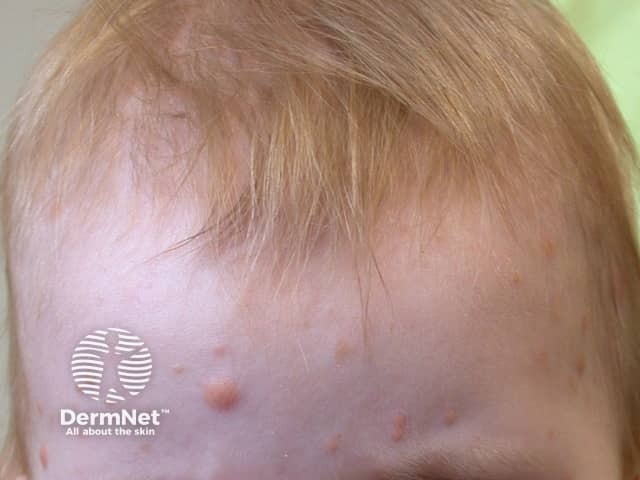
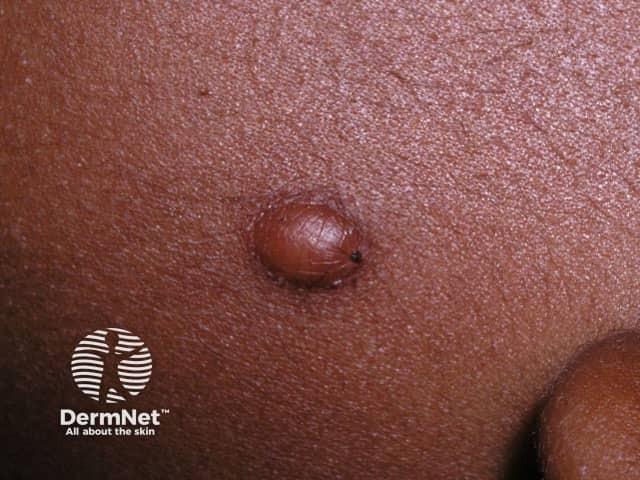
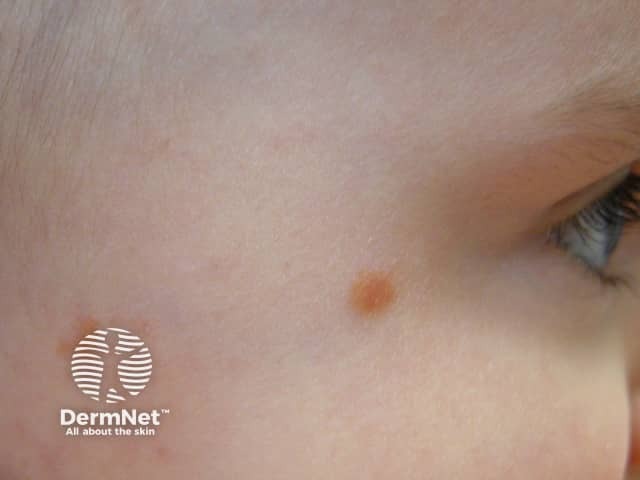
Juvenile xanthogranuloma (JXG) typically presents before one year of age (85%). One third present as a congenital lesion, and adult-onset cases do occur (10%). There is a male predominance in children (up to 7:1) but no difference between the sexes in adult-onset disease. JXG is considered a rare disease in itself, but is the most common type of non-Langerhans histiocytosis.
The incidence of juvenile xanthogranuloma is estimated to be 1 per million in children, however it is probably underdiagnosed.
Up to 10% of patients with neurofibromatosis type I may develop JXG. There have been many single case reports of JXG occurring in association with other conditions.
Juvenile xanthogranuloma is a polyclonal proliferation of cholesterol-containing factor XIIIa-positive histiocytes, the cause of which is unknown. Theories include:
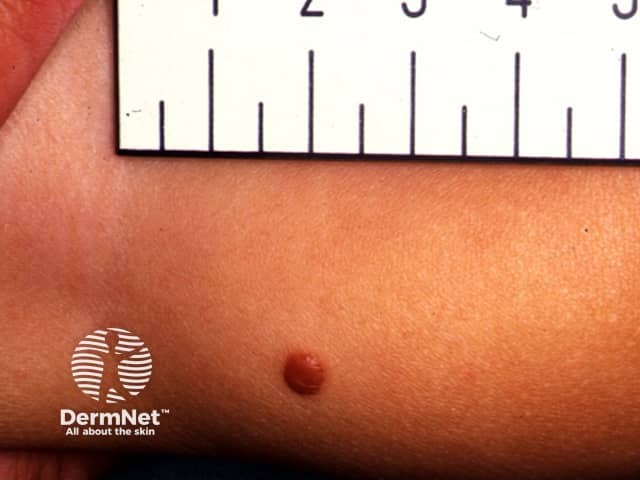
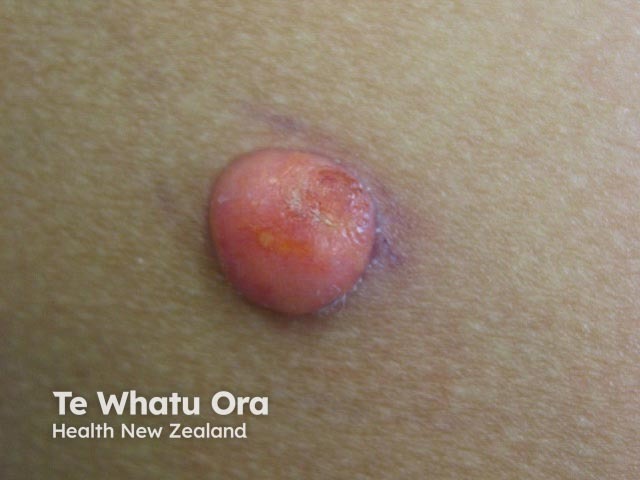
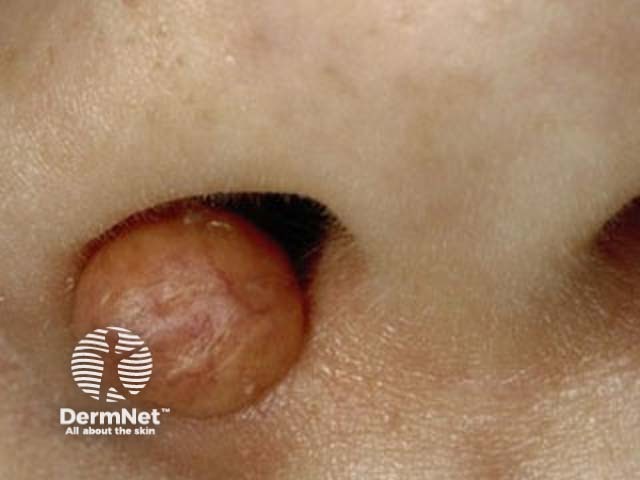
Juvenile xanthogranuloma is probably underdiagnosed in dark skin as erythema can be difficult to appreciate and the asymptomatic nature and self-limiting course mean a solitary lesion may not be noticed.
Juvenile xanthogranuloma is rarely a clinical diagnosis, although dermoscopy is characteristic. Confirmation may require biopsy [see Juvenile xanthogranuloma pathology].
Patients with more than two skin lesions, early onset lesions, and/or a unilateral red eye or ocular symptoms should be referred for an eye examination.
Following a full skin examination, a typical solitary lesion may be investigated only if clinically indicated. If two or more skin lesions are identified investigations should be directed by clinical symptoms and signs, and may include:
Juvenile xanthogranuloma is usually self-limiting with skin lesions regressing in 3–6 years. Even systemic JXG resolves spontaneously in most cases. Skin lesions of juvenile xanthogranuloma in adults tend to be more persistent than JXG in children.