Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Juhee Roh, Post Graduate Year 2 House Officer, Waitemata District Health Board, Auckland, New Zealand. Copy edited by Gus Mitchell. November 2020.
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Outcome
ACE inhibitor-induced angioedema is a rare but potentially fatal adverse effect of the class of medications that inhibit angiotensin converting enzyme (ACEi). It typically presents in the first weeks after starting the ACEi as swelling of the face, lips, or tongue in the absence of itch or urticaria.
ACE inhibitors are very commonly prescribed medications used to treat hypertension, coronary artery disease, congestive heart failure, diabetic nephropathy, and chronic kidney disease. Angioedema is reported to affect 0.1–0.7% of those taking an ACEi, and is one of the most common causes worldwide of a patient presenting to an emergency department with angioedema.
Factors recognised to increase the risk of developing ACE inhibitor-induced angioedema include:
ACE inhibitor-induced angioedema is due to the inhibition of bradykinin degradation resulting in elevated plasma bradykinin. As most people on ACEi are able to normalise the bradykinin level by other pathways, a genetic susceptibility is assumed. It is important to note ACE inhibitor-induced angioedema does not involve histamine.
Angioedema is an acute, transient, localised deep swelling of skin or mucous membranes, typically affecting loose areas of tissue in non-dependent areas, and not usually associated with itch or urticaria.
ACE inhibitor-induced angioedema can involve:
Episodes of angioedema usually begin in the first month after starting the ACEi, but onset can be delayed by months or years. Initially symptoms can be mild and self-resolving so identifying the cause may delayed.
ACE inhibitor-induced angioedema particularly affects those of African descent.
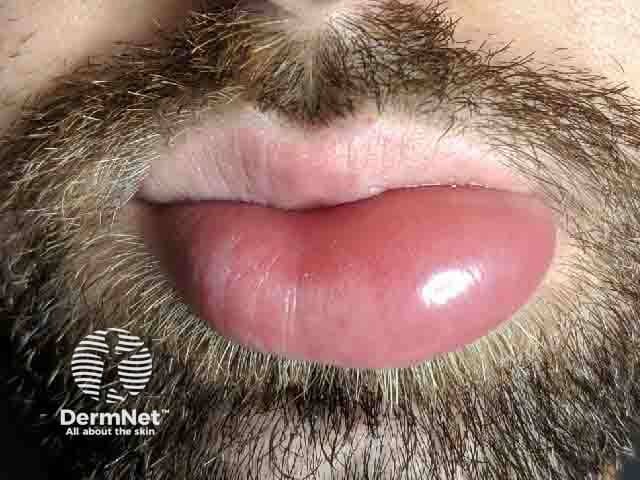
Lip angioedema
Swelling of the upper airways, including the tongue, can obstruct breathing resulting in asphyxiation and death.
Misdiagnosis of gastrointestinal angioedema may result in unnecessary laparotomy.
ACE inhibitor induced-angioedema is a clinical diagnosis based on typical episodes of angioedema in a patient taking an ACE inhibitor. A failure to respond to antihistamines, adrenaline (epinephrine), or systemic corticosteroids is a clue to diagnosis. Ceasing the drug should result in resolution of symptoms, although mild episodes may continue in the first few months.
Gastrointestinal angioedema may be diagnosed on ultrasound or CT scan.
ACE inhibitor-induced angioedema is a bradykinin-mediated angioedema, so must be distinguished from histamine-mediated angioedemas.
Other bradykinin-mediated angioedemas include:
General measures to treat ACE inhibitor-induced angioedema can include:
Specific measures to treat ACE inhibitor-induced angioedema can include the following.
Mild episodes of ACE inhibitor-induced angioedema are self-limiting and resolve without treatment. However, episodes tend to become more frequent and more serious with continued use of the ACEi, and can be fatal if the cause is unrecognised. Discontinuing the ACEi is the only long-term management option, and episodes may continue in the weeks or months after cessation.