Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 2005; Updated: Dr Maanasa Bandla, Hospital Intern, Monash Health, Melbourne, Australia; Dr Martin Keefe, Dermatologist, Christchurch, New Zealand. Copy edited by Gus Mitchell. June 2021
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Bromhidrosis, also known as osmidrosis or ozochrotia, is an unpleasant or offensive body odour due to any cause including poor hygiene, infections, diet or medications, or inherited metabolic disorders. It may be associated with hyperhidrosis.
Bromhidrosis can affect all age groups, races, and both sexes. Bromhidrosis is more common in adults than children as sebaceous glands and apocrine sweat glands do not become active until puberty. The elderly have a different body odour from babies, pre-pubescent children, teenagers, and adults. It has a male predominance, and can be a particular issue in hot humid tropical climates. There may be a genetic predisposition, with studies suggesting axillary malodour is more common in Europeans and Africans than Asians.
Body odour is normal and is primarily produced by the breakdown of sweat, sebum, and keratin by bacteria on the skin surface (skin microbiota). What is regarded as acceptable is determined by cultural influences including race and social upbringing.
Bromhidrosis may be classified as eccrine or apocrine, exogenous or endogenous:
Bromhidrosis presents as a bad body smell which the patient may be unaware of. Malodour may be the reason for the consultation, raised by a mother or partner, or be obvious during a medical consultation for other reasons. The odour may be worse after exercise, often adhering to clothing.
Apocrine bromhidrosis is the most common form of bromhidrosis in adults and is localised, usually to the armpits and/or anogenital area.
Eccrine bromhidrosis presents as a generalised malodour, and may be associated with bad breath (halitosis), anogenital odour, and smelly urine.
Specific sites and features to look for on examination:

Underarm sweating
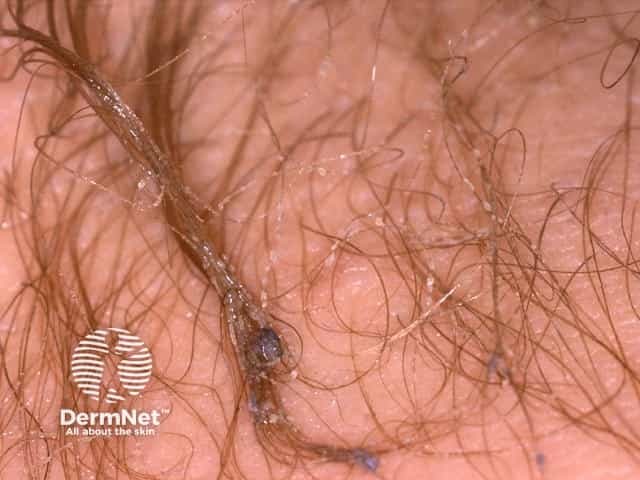
Trichomycosis axillaris
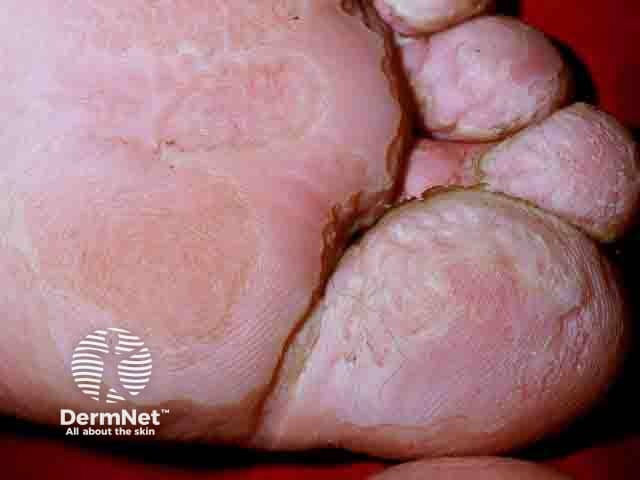
Macerated skin over the toes and ball of the foot in pitted keratolysis
Bromhidrosis can have a significant impact on quality of life, causing:
Bromhidrosis is a clinical diagnosis, but careful history and examination is required to determine the underlying cause. Investigations should be considered in children, if the smell is generalised also involving urine and breath, or if it is of recent onset unrelated to hygiene habits.
The clinician who notices a strong body odour is wise to tread carefully when broaching the subject but correct diagnosis and treatment has the potential to be life-changing for the patient.
Fixing bromhidrosis due to poor hygiene or other treatable causes can be life-changing. However not all cases of malodorous body odour can be completely suppressed.