Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA; Chief Editor: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. February 2016.
Introduction
Occupational risks
Causes
Associated skin disorders
Workplace assessment
Diagnosis and treatment
Childcare work is a major employer worldwide. The number of people employed in this sector is expected to expand, especially in developing countries where more women have entered the workforce and are choosing childcare centres over babysitters or childcare from relatives. However, it is considered to be an occupation at high risk for work-related skin disorders.
Factors that put childcare workers at risk of work-related skin conditions include:
Occupational skin diseases are a variety of dermatological conditions that are the result of — or made worse by — the nature of the patient’s job. It has a large economic impact in the form of missed days of work and may lead to a change of profession if the condition becomes severe. Occupational dermatoses occur when the protective barrier of the skin is breached by mechanical, chemical, or biological means, including cuts and abrasions, exposure to irritants and allergens or contact with viruses or bacteria. In developed countries, tighter regulation and a greater emphasis on worker safety have been credited with reducing the rate of occupational skin disorders.
There are a number of occupational skin disorders related to childcare workers, including:
Contact dermatitis is the most frequently occurring skin problem in child care workers.
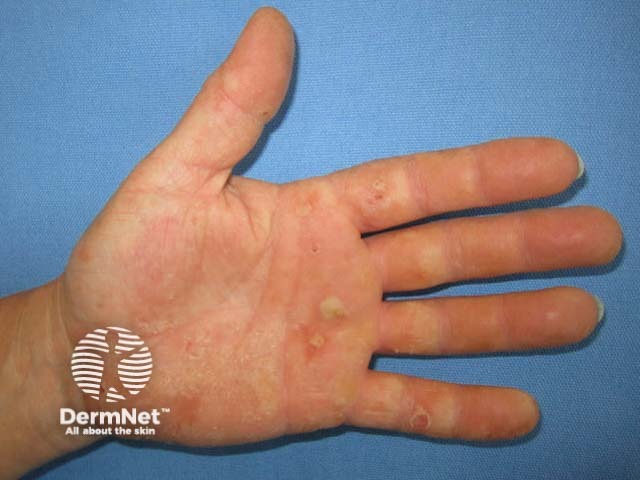
Hand dermatitis due to rubber glove allergy
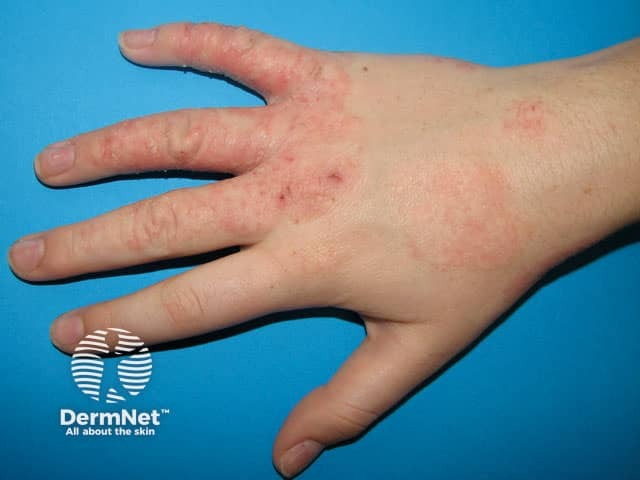
Hand dermatitis
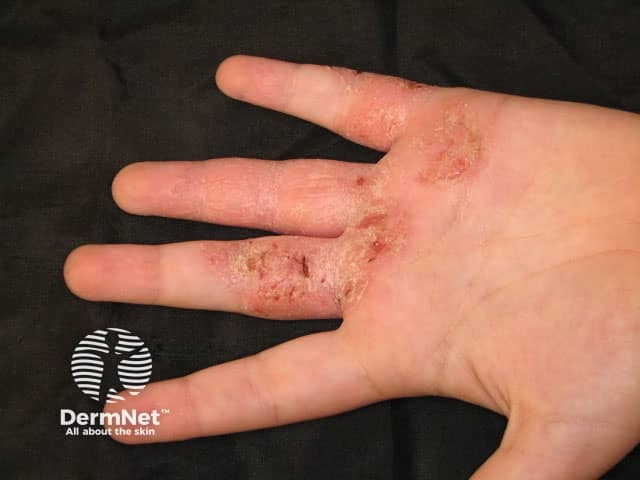
Hand dermatitis
These are another common risk for child care workers.
Due to contact with babies, toddlers, and preschoolers, human bite injuries may occur.
Head lice are a frequent and ongoing problem in the childcare setting.
Sun exposure tends to be overlooked but can represent a significant risk over time for childcare workers.
An effective workplace assessment should include:
Gloves for hand protection are the most frequently used form of personal protective equipment.
Advice for protecting childcare workers includes:
Diagnosis of an occupational skin disorder should be based on:
Management of occupational skin disease may include: