Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Jennifer Nguyen, House Medical Officer, Monash Health, Melbourne, Australia; A/Prof Rosemary Nixon AM, Dermatologist and Occupational Physician, Occupational Dermatology Research and Education Centre, Carlton, Australia. Copy edited by Gus Mitchell. April 2021
Introduction
Common types
Causes
Clinical features
Prevention
Treatment
Outcome
Face masks and respirators are examples of personal protective equipment (PPE) worn over the mouth and nose to protect the wearer from inhaling particles and dust, and to reduce the risk of spread of airborne infectious pathogens. Face masks are used by the general public during viral epidemics, and routinely in occupational settings such as healthcare facilities and dusty work environments.

Face masks

N95 mask

Mask etiquette
Mask etiquette image from World Health Organization, 2020

Cotton face mask

Surgical mask

N95 mask with exhalation valve
The skin barrier can be compromised due to increased humidity and temperature, created from breathing in a closed environment under a face mask. This causes follicular occlusion, increases sebum secretion, and changes skin microflora. Mechanical effects are due to friction and pressure.
Further contributory factors include:
Facial itch, redness, rash, dryness and peeling, swelling and numbness, pain and tingling, and oily skin are commonly reported symptoms related to face mask usage, particularly when a mask is worn for more than 4 hours daily.
Mechanical skin damage can initially present as pressure indentations around the nose from the metal nose clip, or itching, redness, and scaling behind the ears due to the earloops.
Friction may also cause koebnerisation of a pre-existing skin condition such as psoriasis and vitiligo.
Mechanical skin damage may progress to erosions, ulceration, postinflammatory hyperpigmentation, and scarring.
Mask wearing can induce or exacerbate acne, an effect that has been colloquially termed ‘maskne’, a form of acne mechanica. It is the commonest skin rash related to face masks and particularly affects the cheeks. Rosacea flares can also be triggered by face mask usage. Acne and rosacea flares due to face masks can impact quality of life.
Underlying skin conditions such as atopic dermatitis increase the risk of developing irritant contact dermatitis (ICD) due to a pre-existing defective skin barrier [see Barrier function in atopic dermatitis].
Allergic contact dermatitis (ACD) is a less common cause of mask reactions. Identifying the allergen can be difficult due to the variety of constituents used by manufacturers and the lack of publicly available information. Reported causes of ACD related to masks include:
Worsening of seborrhoeic dermatitis may present with increased itch, redness, and peeling, particularly with prolonged mask-wearing. This is thought to be due to the overgrowth of malassezia yeasts under the mask.
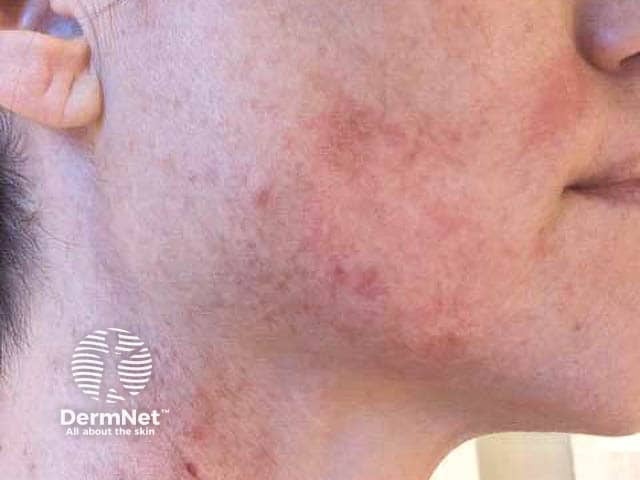
Face mask dermatitis
Skin reactions to face masks will usually improve or resolve with reduced or cessation of mask use.