Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1999; Updated and revised by: Dr Gia Toan Tang, RMO, Townsville University Hospital, Townsville, Australia; A/Prof Rosemary Nixon AM, Dermatologist, Skin Health Institute, Melbourne, Australia. Copy edited by Gus Mitchell. February 2021.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Chilblains are tender and/or itchy bumps on acral sites following exposure to damp, cold, non-freezing conditions causing a localised form of vasculitis. Chilblains are also called pernio or perniosis.
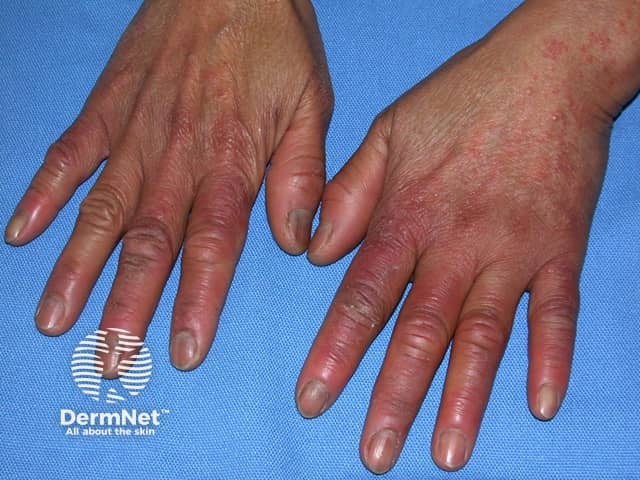
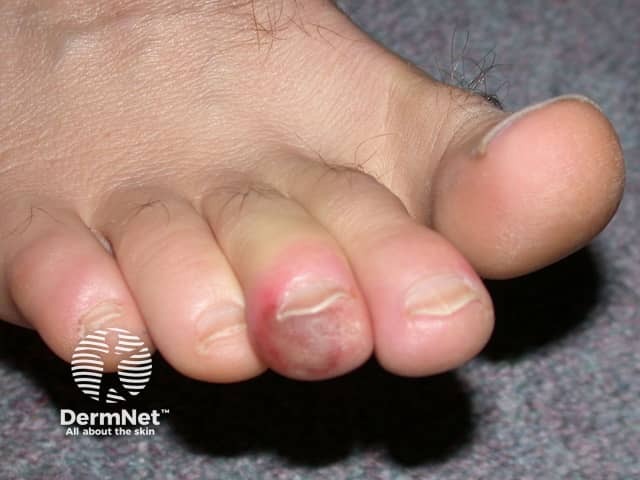
Chilblains can affect all age groups, but is most common in young to middle-aged adults, with a female predominance. Childhood chilblains are well-described but appear to be uncommon. Primary chilblains are unusual in the elderly and an underlying cause should be looked for.
Risk factors predisposing to the development of chilblains include:
Chilblains are seen in temperate climates rather than in countries with extreme cold where the air is often dry, and appropriate clothing and living conditions minimise the risk. Late winter and early spring, when it is wet and temperatures are above freezing, are the peak seasons for chilblains.
During the COVID-19 pandemic, many cases of chilblain-like changes on the toes ('COVID-toes') have been reported as a late manifestation in children and young adults after a mild illness suspected of being due to the novel coronavirus SARS-CoV-2; PCR swabs and antibodies for the virus have been mostly (but not always) negative. Many reported patients had no recent exposure to cold, and a robust antiviral interferon response has been postulated to induce changes in the small blood vessels. Histology has been performed on a small number of cases and the changes described have been typical of chilblains, chilblain lupus, or a thrombotic vasculopathy pattern. The association between COVID-19 and chilblains is still being defined. However, the development of chilblain-like lesions in the absence of exposure to damp cold or secondary causes, should be suspected as being related to SARS-CoV-2 infection.
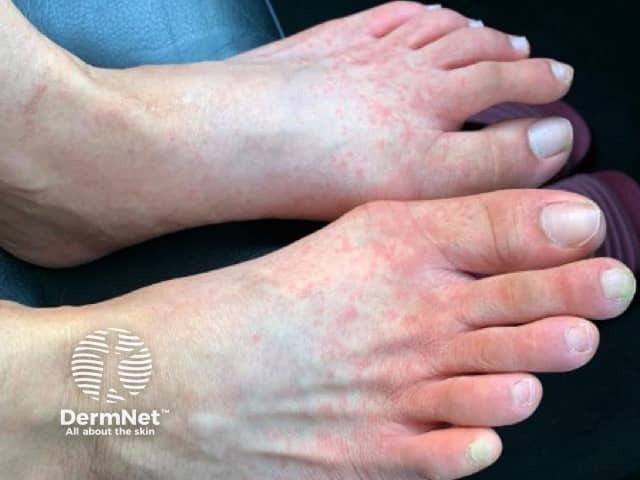
Suspected COVID-19 rash
Cold causes constriction of small arteries and veins but a protective physiological reflex intermittently dilates the blood vessels to prevent skin ischaemia. Persistent or prolonged vasoconstriction due to an abnormal vascular reaction to cold may result in hypoxaemia and inflammation to produce chilblains.
Chilblains commonly occur on the fingers, toes, and ears (acral sites). However, chilblains can develop on any areas exposed to chronic cold, such as the thighs/hips of horse riders (‘equestrian panniculitis’). Chilblains develop several hours after exposure to damp cold and last for more than 24 hours.
Chilblains typically present as:
Dermoscopy is not very informative, but examination of the nailfold capillaries may be useful if an underlying connective tissue disease is suspected.
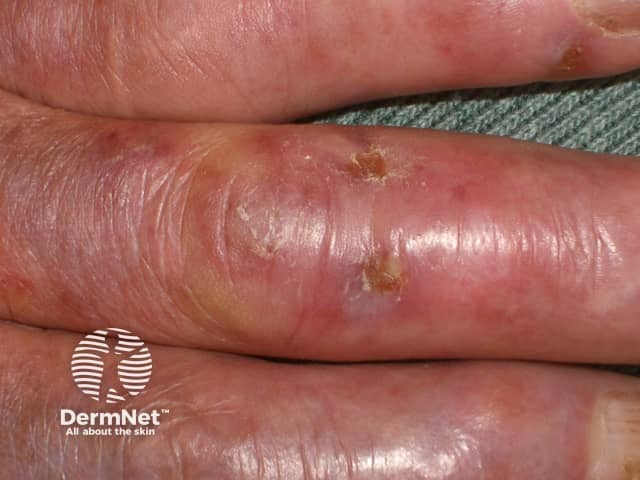
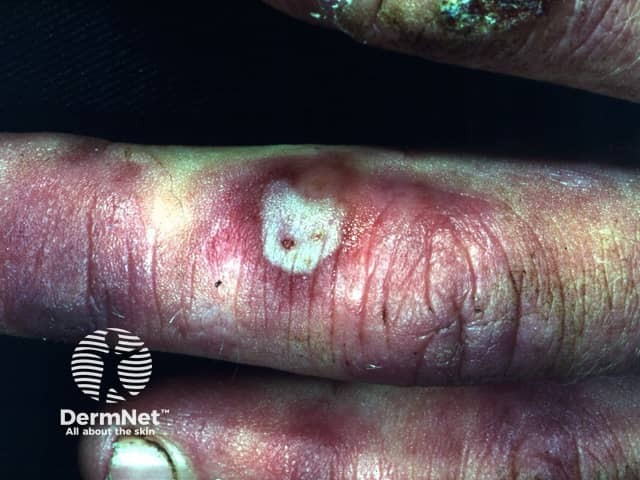
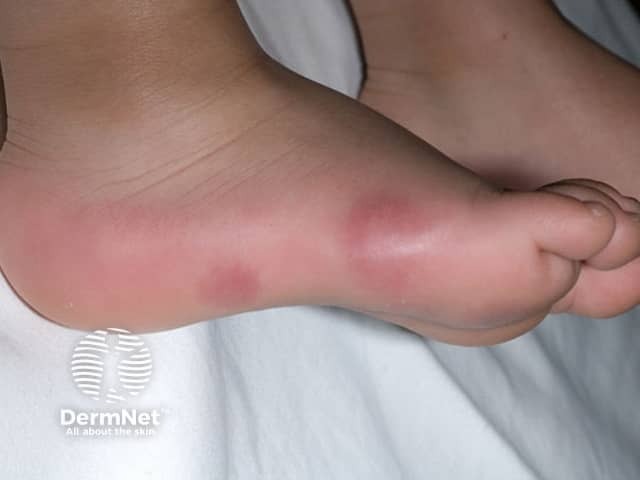
Severe chilblains may blister, or become eroded and ulcerated.
Chilblains are usually diagnosed clinically. Investigations are sometimes required to exclude differential diagnoses or look for causes of secondary chilblains.
Skin biopsy of primary idiopathic chilblains shows a superficial and deep lymphocytic vasculitis, lymphocytes around the eccrine sweat glands, subepidermal oedema, with or without interface changes. [see Perniosis pathology].
The Mayo Clinic has developed diagnostic criteria for chilblains:
Major criterion (required) — localised redness and swelling of acral sites lasting at least 24 hours.
Minor criteria (at least one of the following):
Chilblains are classified as idiopathic (primary) if there is no associated cause, and secondary if a cause can be identified.
Investigations for secondary causes of chilblains may include:
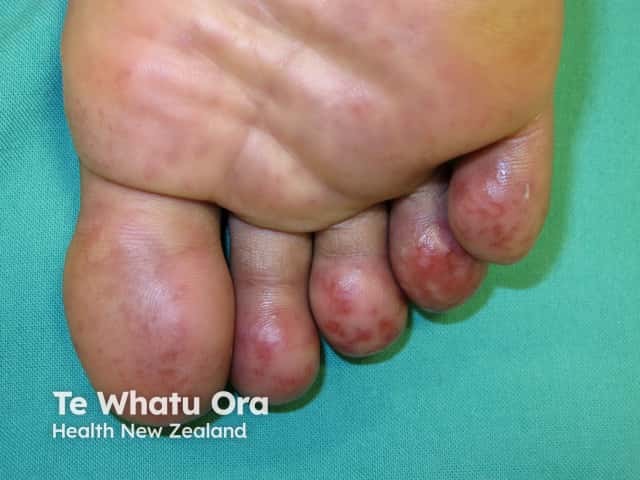
Lupus chilblains
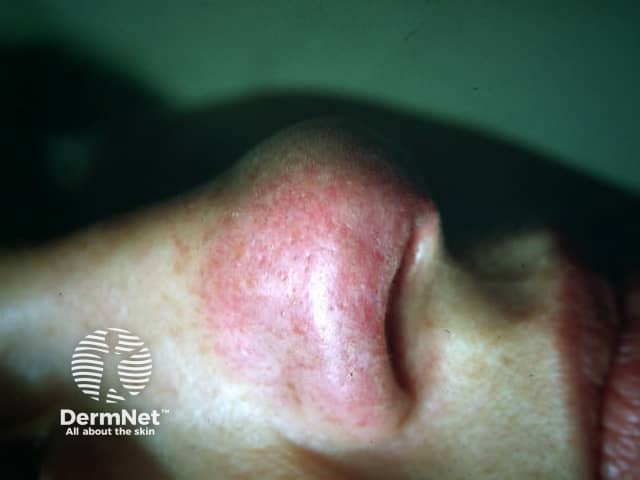
Lupus pernio
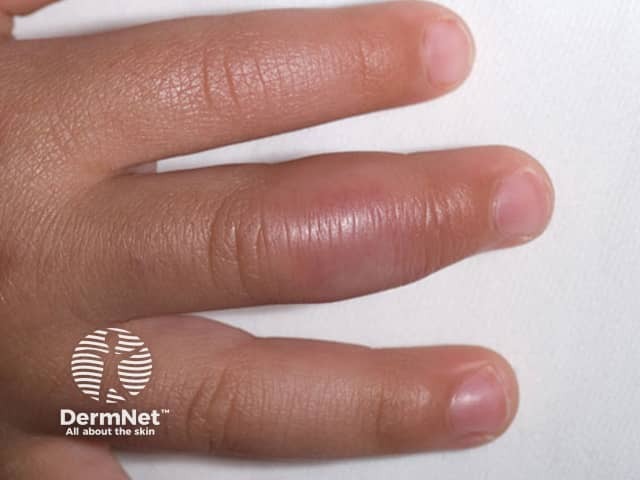
Microgeodic disease
Chilblains usually resolve spontaneously in 1–3 weeks. However, chilblains can become chronic. Recurrences may occur with subsequent exposures or annually.