Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. March 2017.
Introduction - psoriasis
Demographics
Introduction - psychological effects of psoriasis
Clinical features
Diagnosis
Treatment
Outcome
Psoriasis is a chronic skin disease characterised by red, scaly plaques. These can be minimal or very extensive on the scalp, face, trunk and limbs. Psoriasis may also involve the nails (psoriatic nail dystrophy). Psoriasis is relatively common, affecting around 2–4% of the general population. It is associated with psoriatic arthropathy and several other health problems.
Long-term, disfiguring scaling and redness on the face, neck and other readily visible portions of the body can cause severe negative psychological effects for people with psoriasis.
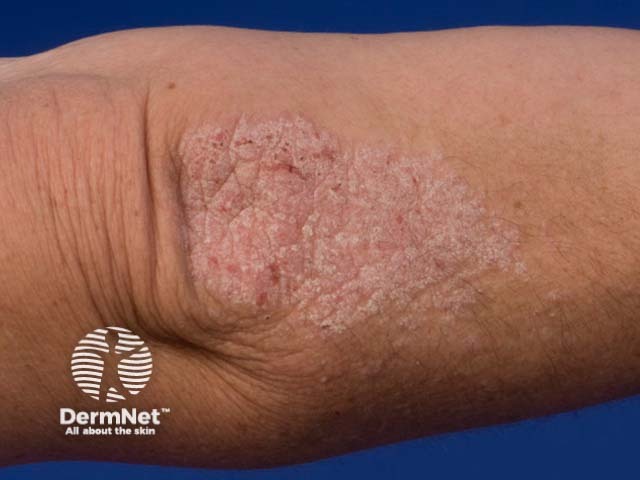
Chronic plaque psoriasis
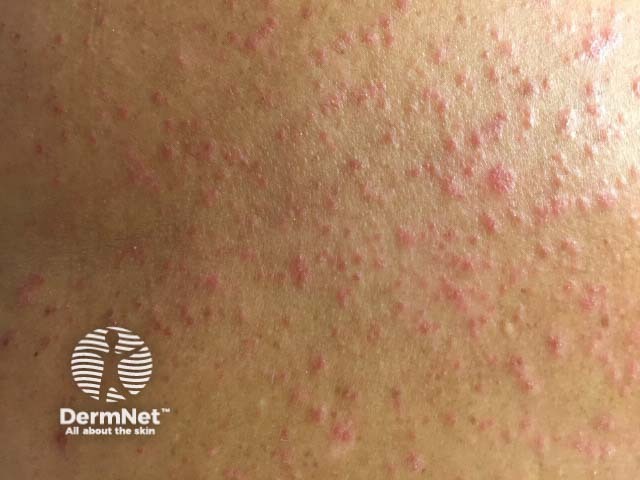
Guttate psoriasis

Nail psoriasis
Most people with psoriasis report that it affects their quality of life to some extent. Patients with disfiguring scaling and redness on the face, neck and other readily visible portions of the body are particularly affected by the skin disorder, particularly if the onset of psoriasis is during childhood and adolescence.
It has been estimated that the psychological impact of their skin disorder is severe in 10–62% of patients with psoriasis.
Psoriasis is associated with a variety of psychosocial symptoms, including:
Depression affects a large percentage of people who suffer from psoriasis, and can lead to:
Useful tools that can be used to measure the impact of psoriasis on the individual include:
Treatment for psoriasis may require collaboration between a dermatologist and a psychologist or psychiatrist to deal with both the physical and psychological effects of the disorder. The successful treatment of the physical symptoms of psoriasis often leads to improvement in the psychological effects of psoriasis on the patient; for example, their depression, alcohol dependence, or behavioural disorder (eg, obsessive–compulsive disorder) improves.
The psychological effects of psoriasis may be treated with any combination of the following:
The psychological effects of psoriasis can have deep and negative impact on family and other social relationships, work and employment, education and other aspects of life for those affected, especially if those effects go untreated.