Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
A cracked heel is a common foot problem. In most cases the problem is merely a nuisance and unattractive to look at, however, when the cracks or fissures become deep, standing, walking or any pressure placed on the heel can be painful.
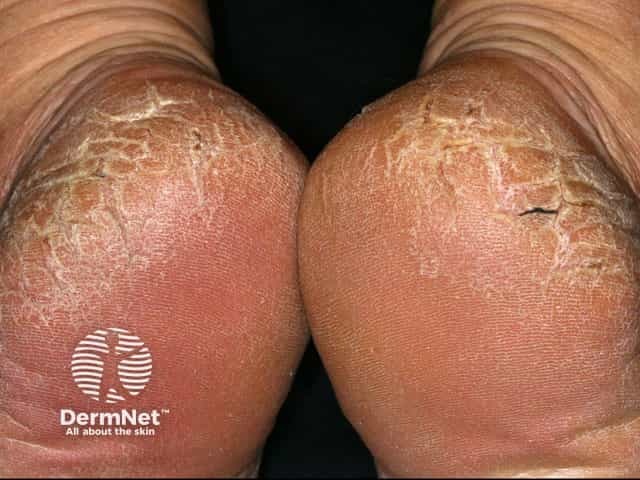
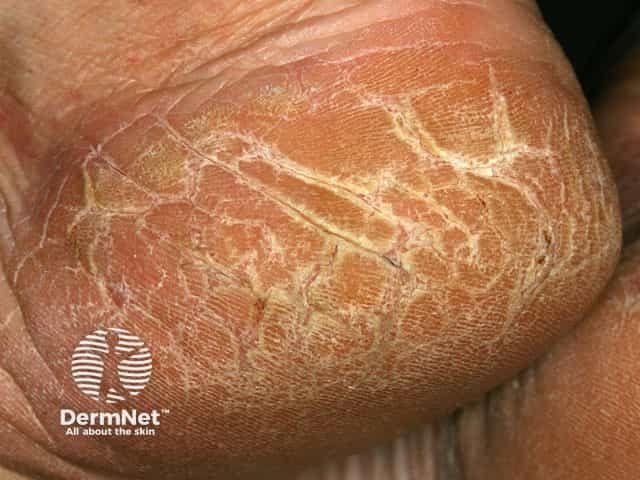
Cracked heels
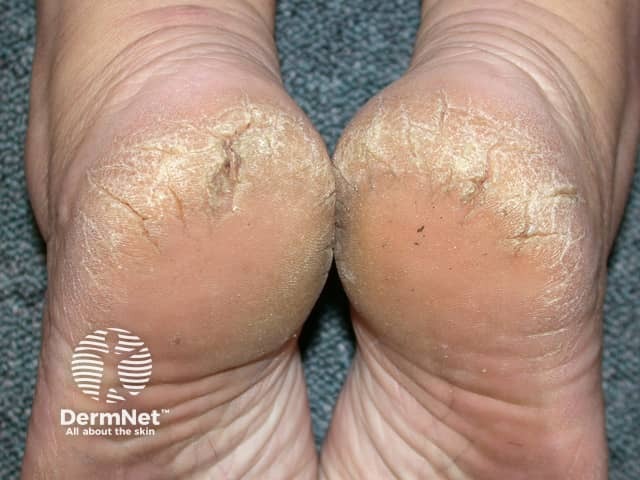
Cracked heels
Anyone can get a cracked heel. Predisposition may be due to:
Dry thickened skin (corn and callus) around the rim of the heel is the very first step towards cracking. Increased pressure on the fat pad under the heel causes it to expand sideways, leading to splitting or cracking of the callus. Some factors that contribute to cracking or splitting include:
The first sign of getting cracked heel is the development of dry, hard, thickened skin around the rim of the heel. This is called a callus and may be a yellow or dark brown discoloured area of skin. Initially, small cracks over the callus are visible. If left untreated and as more pressure is placed on the heel, these cracks become deeper and eventually walking and standing will be painful. The cracks may be so deep that they begin to bleed.
In severe cases, cracked heels can become infected, and lead to cellulitis. This must be treated with the elevation of the area, debridement of dead tissue, and antibiotics.
Cracked heels are of particular concern for diabetic patients, who may suffer neuropathic damage (loss of feeling, particularly of the feet), as the fissures may lead to diabetic foot ulcers.
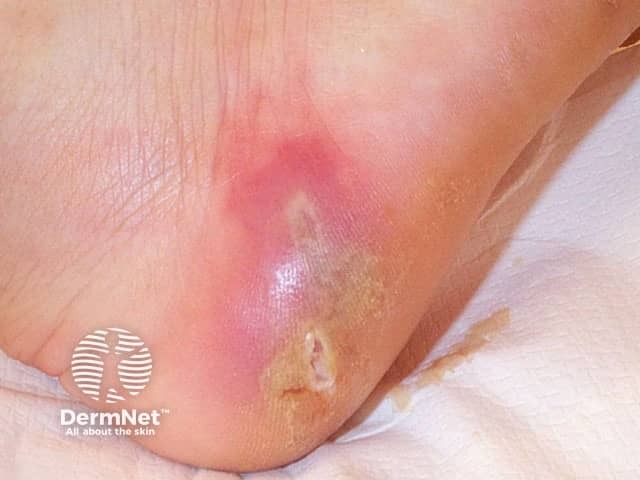
Cellulitis
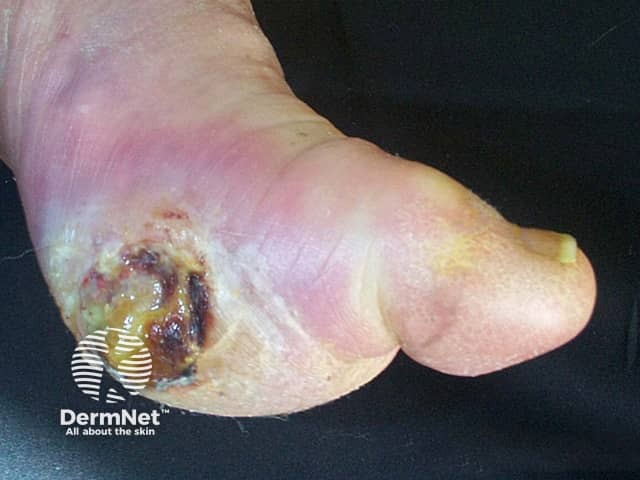
Diabetic ulcer
The best form of treatment for cracked heel is to prevent cracks from occurring in the first place. This can be achieved by simply rubbing the heels with a moisturising cream on a regular basis to keep the skin supple and hydrated. Special heel balms are available that contain descaling (keratolytic) or water-retaining (humectant) agents, such as:
Feet should be inspected daily and on the first sign of any cracking, a moisturising routine 2–3 times a day may be all that is needed to heal the heel. A pumice stone can be rubbed gently against the callus to take away some of the thick hard skin before applying moisturiser.
The fissures may be treated with a liquid, gel or spray bandage to reduce pain, protect and allow more rapid healing.
For severely cracked heels or if no improvement is seen after a week of self-treatment a visit to a podiatrist may be required. Treatments may involve the following: