Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Original page by Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated by Dr Anita Eshraghi, Dermatologist, Sweden, and Dr Oakley, in March 2018. Revised September 2020.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Juvenile plantar dermatosis is a common and chronic, dry-skin condition of the feet that mainly affects pre-adolescent children.
Juvenile plantar dermatosis is also known as atopic winter feet and forefoot dermatitis.
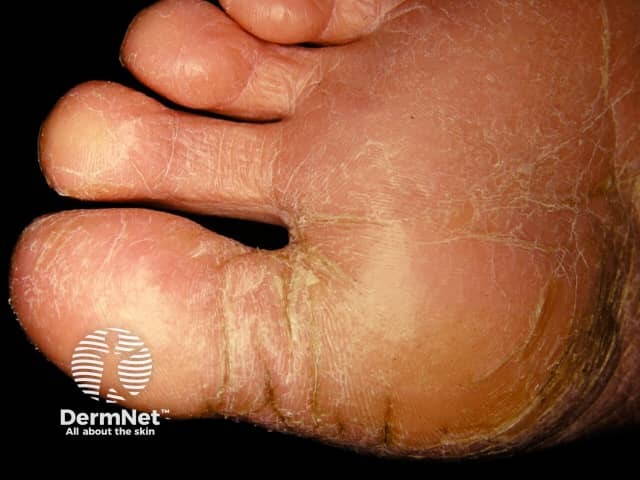
Juvenile plantar dermatosis
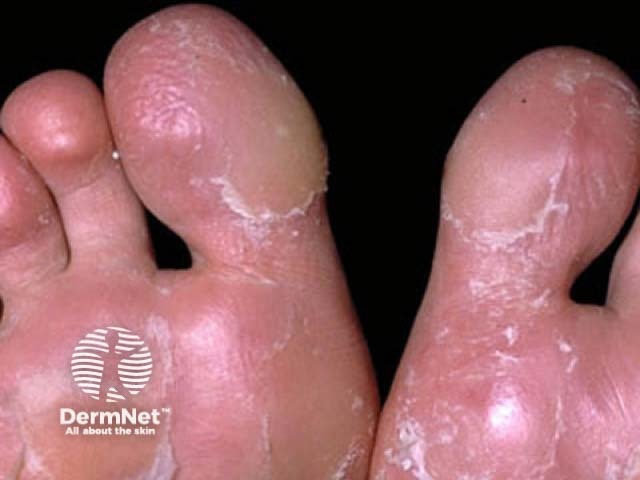
Juvenile plantar dermatosis
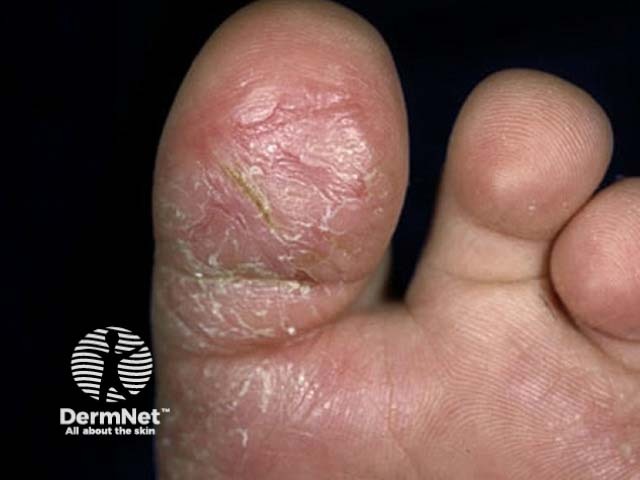
Juvenile plantar dermatosis
See more images of juvenile plantar dermatosis.
Juvenile plantar dermatosis commonly affects children between the age of 3 and 14 years, with an average age of 8. It occurs slightly more frequent in boys than girls. Juvenile plantar dermatosis is rarely seen in adults.
Although an association has been suggested with atopic dermatitis, asthma, or hay fever, this has not been confirmed in case control studies.
Juvenile plantar dermatosis may be caused by:
Juvenile plantar dermatosis involves the weight-bearing areas of the soles of the feet presenting as itchy or sore, shiny, red skin with a glazed appearance and loss of the epidermal ridge pattern.
The diagnosis of juvenile plantar dermatosis is based on the clinical findings.
Skin scrapings to exclude a fungal infection (tinea pedis) and patch tests for contact allergy to footwear may be performed.
Skin biopsy is rarely required. Histology shows epidermal spongiosis and dermal inflammation centred around the sweat ducts.
Juvenile plantar dermatosis is sometimes difficult to distinguish from:
There is no consistently useful treatment. General recommendations include the following without supporting studies to show benefit.
When applied once or twice daily for courses of up to 4 weeks, these rarely prove more effective than simple emollients.
Juvenile plantar dermatosis usually clears spontaneously in adolescence, but can persist into adult life.