Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2002. Updated September 2015.
Introduction
Prevalence
Causes
Demographics
Signs and symptoms
Diagnosis
Treatment
Complications
Prevention
Scarlet fever is a bacterial illness that often presents with a distinctive rash made up of tiny pinkish-red spots that cover the whole body. It affects people who have recently had a sore throat (strep throat) or school sores (impetigo) caused by certain strains of the group A streptococcus bacteria. A toxin released by the streptococcal bacteria causes the rash of scarlet fever.
Scarlet fever has also been called scarlatina in the past.
Scarlet fever is not as common as it was a century ago when it was associated with deadly epidemics. The development of antibiotics and their early use in the treatment of streptococcal infections has prevented many cases of scarlet fever and the long-term complication of rheumatic fever.
Scarlet fever occurs mostly in children aged 4-8 years. By 10 years old, up to 80% of children have developed lifelong protective antibodies against streptococcal toxins, whilst children younger than 2 years still have acquired maternal antiexotoxin antibodies. Males and females are affected equally.
Group A streptococcal infections that cause scarlet fever are contagious. Streptococcal bacteria can spread from person to person by breathing in airborne droplets from an infected person's coughing or sneezing. Bacteria can also be passed by touching the infected skin of someone with a streptococcal skin infection, or by sharing contaminated clothes, towels or bed linen.
Scarlet fever can also be spread by infected individuals who are carriers of streptococcal bacteria but do not show any symptoms. Up to 15-20% of school-age children are thought to be asymptomatic carriers.
To get scarlet fever you must still be susceptible to the toxin produced by the streptococcal bacteria. Therefore, it can happen that 2 children of the same family may both have streptococcal infections, but only one (who is still susceptible to the toxin) develops scarlet fever.
Scarlet fever generally has a 1–4 day incubation period.
Those at greatest risk for scarlet fever include:
Scarlet fever usually starts with a sudden fever associated with sore throat, swollen neck glands, headache, nausea, vomiting, loss of appetite, swollen and red strawberry tongue, abdominal pain, body aches, and malaise.
The characteristic rash appears 12–48 hours after the start of the fever. The rash usually starts below the ears, neck, chest, armpits and groin before spreading to the rest of the body over 24 hours.
Scarlet spots or blotches, giving a boiled lobster appearance, are often the first sign of rash.
As skin lesions progress and become more widespread, they start to look like sunburn with goose pimples. The skin may have a rough sandpaper-like feel.
In body folds, especially the armpits and elbows, fragile blood vessels (capillaries) can rupture and cause classic red streaks called Pastia lines. These may persist for 1-2 days after the generalised rash has gone.
In the untreated patient, the fever peaks by the second day and gradually returns to normal in 5–7 days. When treated with appropriate antibiotics, the fever usually resolves within 12-24 hours.
By about the sixth day of the infection the rash starts to fade and peeling, similar to that of sunburned skin, occurs. Peeling of the skin is most prominent in the armpits, groin, and tips of the fingers and/or toes and may continue up to 6 weeks.
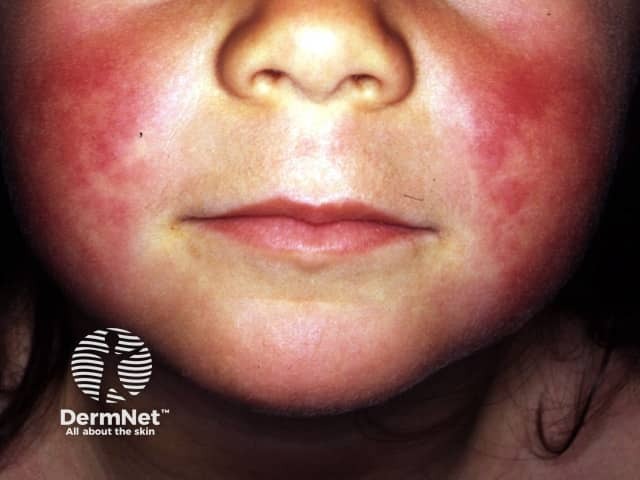
Scarlet fever
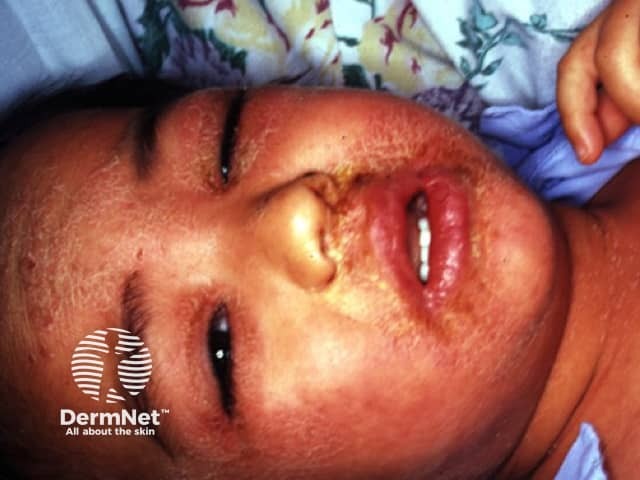
Scarlet fever
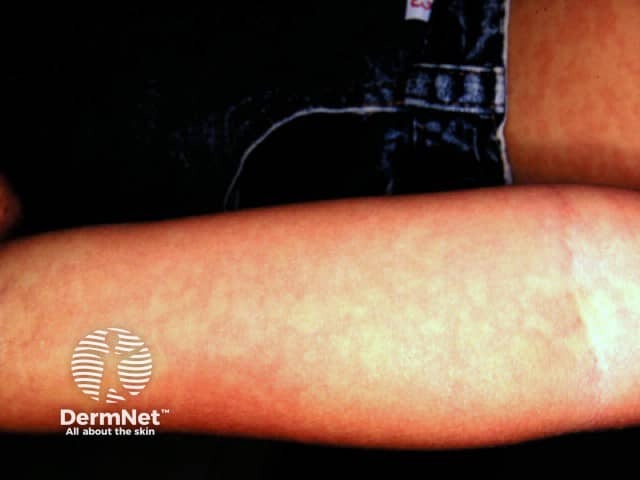
Scarlet fever
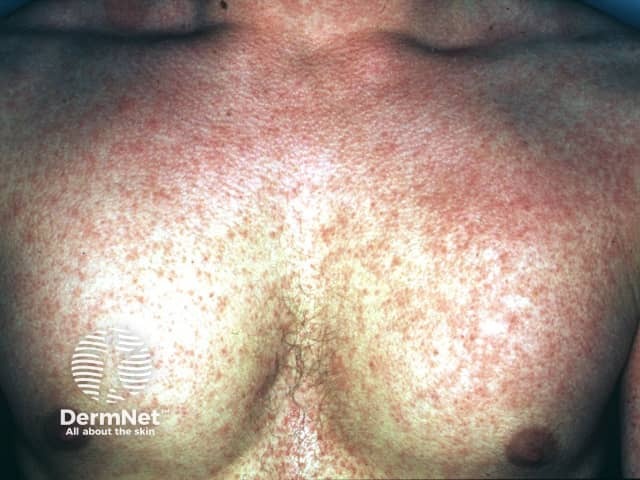
Scarlet fever
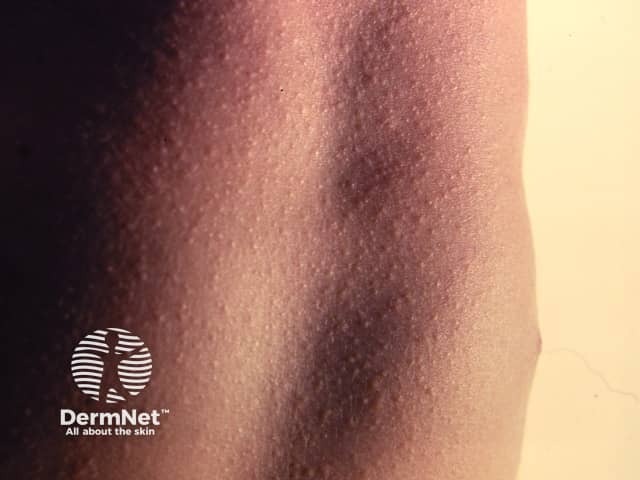
Scarlet fever
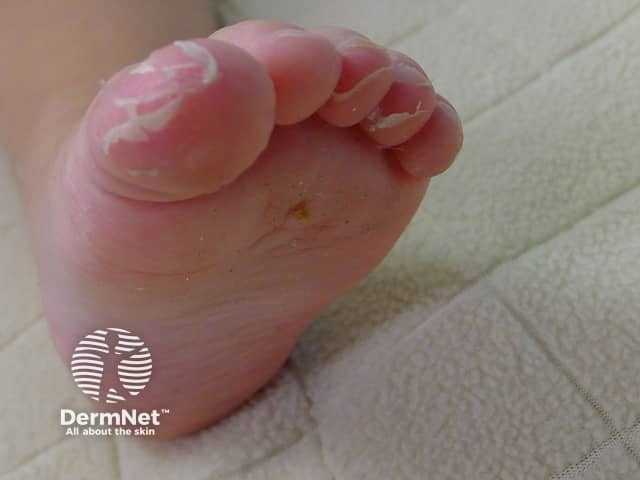
Peeling toes after scarlet fever
Diagnosis of scarlet fever is often suspected from the characteristic history and physical examination. Diagnosis is supported by a swab taken from the posterior pharynx or tonsils. The following methods may be used (check local guidelines):
Blood tests for anti-dexoyribonuclease B and antistreptolysin-O titres may also be helpful.
Once a streptococcal infection is confirmed, a course of antibiotics is prescribed, usually penicillin, for up to 10 days. It is very important that the full antibiotic course is taken to ensure all the infection is cleared, to reduce the risk of complications.
In some situations a single dose of penicillin may be given by intramuscular injection. Patients allergic to penicillin may be treated with an alternative antibiotic, such as erythromycin.
Additional treatments include:
The fever usually improves within 12-24 hours after starting antibiotics and most patients recover after 4-5 days with clearing of skin symptoms over several weeks.
Nowadays, scarlet fever infection usually follows a benign course when diagnosed and treated appropriately. However, if left untreated or treatment is unsuccessful, the following complications caused by the streptococcal infection may arise.
Rheumatic fever, which affects the heart, and glomerulonephritis, which affects the kidneys, may permanently damage the body and require long-term treatment.
To prevent spread of streptococcus bacteria that cause scarlet fever, an infected individual should ideally be isolated from other family members, especially from infants and younger siblings. To help prevent spread, keep drinking glasses and eating utensils used by the infected individual separate from those of other family members. These items need to be washed thoroughly in very hot soapy water, preferably with antibacterial soap or detergent.
Children should be kept away from school until they have received at least 24 hours of antibiotic therapy and there are clear signs of improvement.