Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2004.
Introduction Associated skin conditions Diagnosis Predisposing factors Treatment
Malassezia refers to a group of basidiomycetous (club-shaped) yeasts of the genus Malassezia, which has several different species. Species names include:
Skin conditions caused or aggravated by infection by malassezia include:
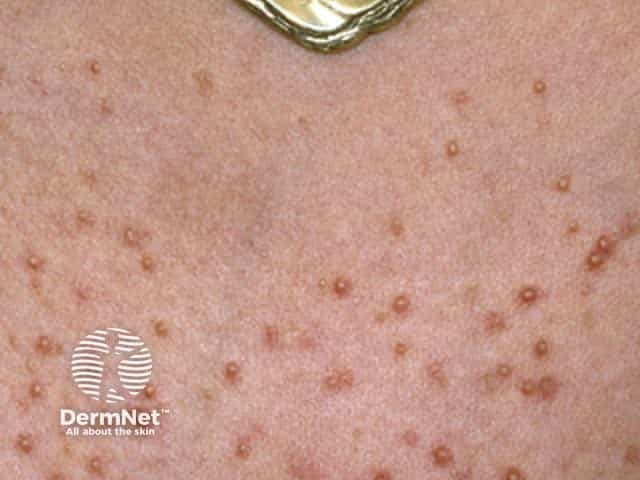
Malassezia folliculitis
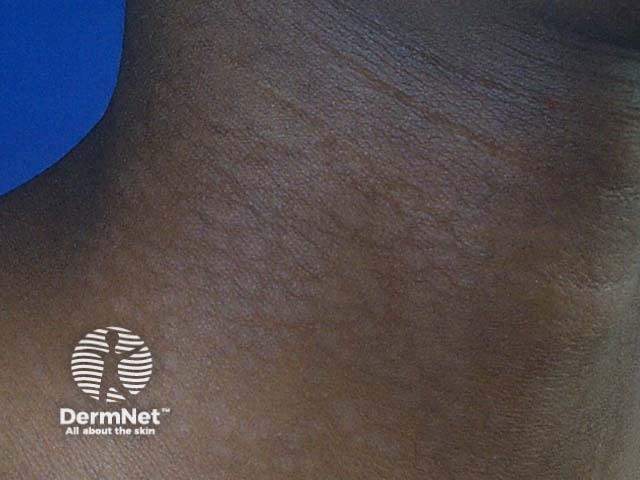
Pityriasis versicolor
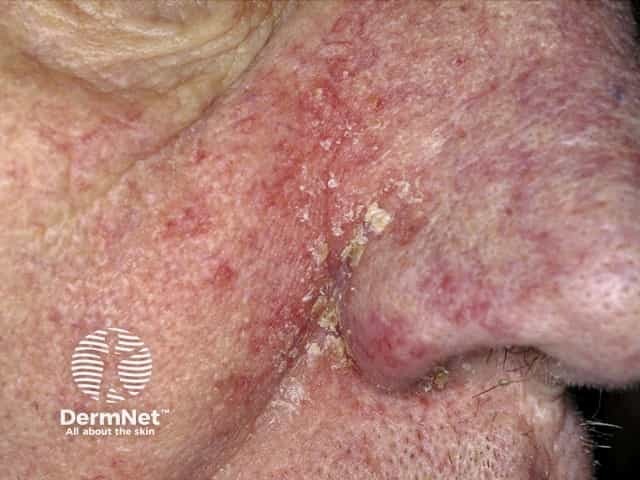
Seborrhoeic dermatitis
The diagnosis of skin conditions associated with malassezia is often made clinically but can be confirmed when skin scrapings reveal malassezia (see laboratory tests for fungal infection). Microscopy of malassezia, using potassium hydroxide (KOH) preparations, shows clusters of yeast cells and long hyphae. The appearance is said to be like 'spaghetti and meatballs'. The hyphae filaments used to be called 'Malassezia' and the yeast forms were called 'Pityrosporum', but mycologists eventually realised they were the same bimorphic organism.
Malassezia species are difficult to grow in the laboratory so scrapings may be reported as 'culture-negative'. The yeast grows best if a lipid such as olive oil is added to Littman agar culture medium.
Yeasts may also be detected within the stratum corneum on histopathology of a skin biopsy; they are best seen using special stains such as periodic acid-Schiff (PAS).
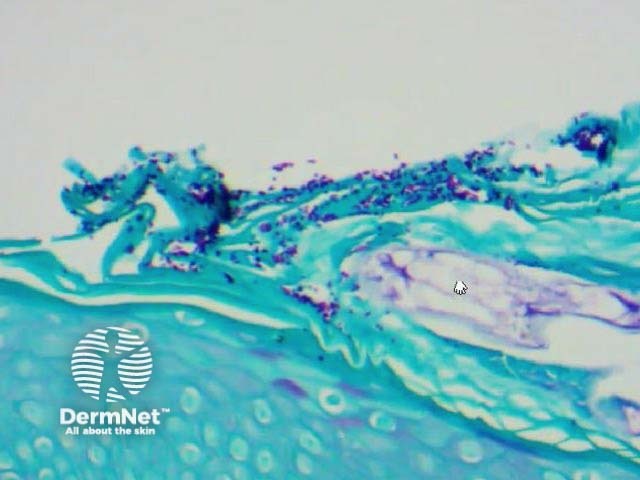
Malassezia species inhabit the skin of about 90% of adults without causing harm. In some people, the yeast suppresses the body's expected immune response to it allowing it to proliferate and cause a skin disorder, often with very little inflammatory response. When malassezia is associated with dermatitis, it is thought that irritating metabolites of the yeasts may be responsible (free fatty acids are hydrolysed from triglycerides).
Predisposing factors to Malassezia skin disease include:
The yeasts produce chemicals that reduce the pigment in the skin, causing whitish patches. These include azelaic acid, pityriacitrin and malassezin. Azelaic acid is a useful treatment for some skin disorders such as acne and rosacea.
Malassezia may fluoresce on exposure to ultraviolet light (Wood lamp). This is due to another chemical, pityrialactone.
Consult DermNet's pages on the individual skin conditions to learn about treatment.
In general, malassezia infections are treated with topical or oral antifungal agents, such as ketoconazole shampoo and oral fluconazole. Seborrhoeic dermatitis may also be treated with topical steroids.