Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Infections Follicular disorder
Author: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand,1997. Updated by Dr Thomas Stewart, General Practitioner, Sydney, Australia, November 2017. Revised September 2020.
Introduction Demographics Clinical features Diagnosis Differential diagnoses Treatment Prevention
Malassezia folliculitis, also known as pityrosporum folliculitis, is an infection of the pilosebaceous unit caused by lipophilic Malassezia yeasts particularly M. globosa, M. sympodialis and M. restricta. Malassezia yeast are normal inhabitants of the human skin surface and only cause disease under specific conditions.
Malassezia yeasts have been linked to a number of other skin diseases including seborrhoeic dermatitis and pityriasis versicolor.
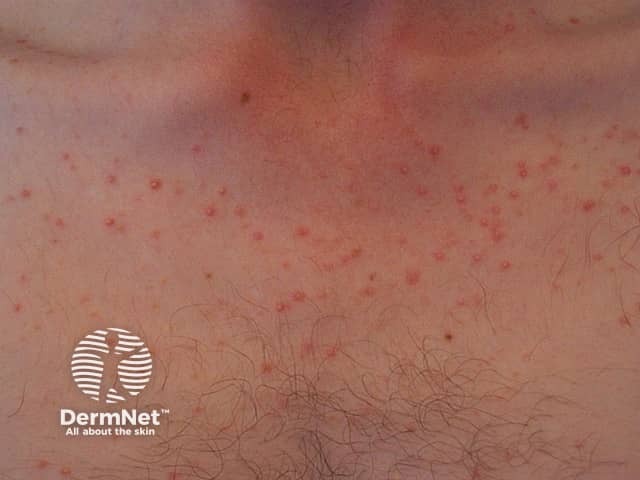
Malassezia folliculitis
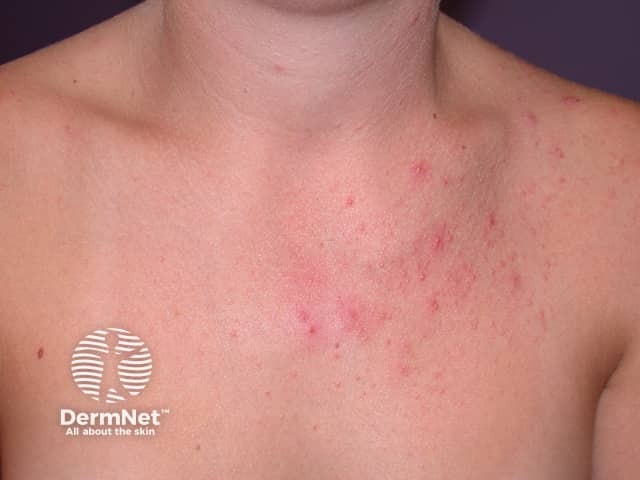
Malassezia folliculitis
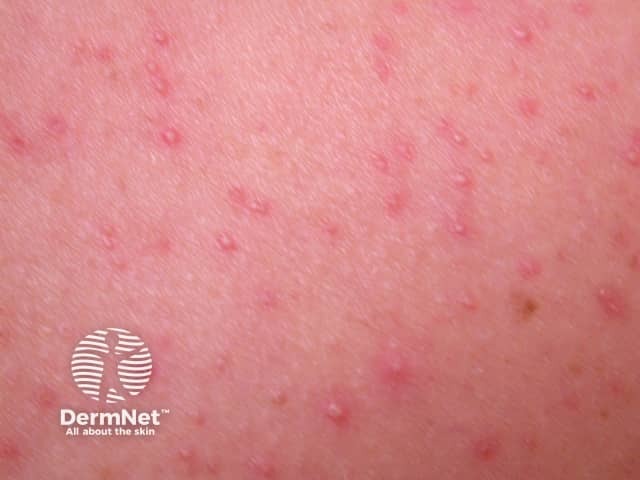
Malassezia folliculitis
Malassezia folliculitis is most commonly seen in adolescent and young adult males.
Risk factors for developing Malassezia folliculitis include:
Malassezia folliculitis presents as small, uniform, itchy papules and pustules particularly on the upper back and chest. Other sites involved can include the forehead/hair line, chin, neck, and extensor aspect of the upper limbs. This is a monomorphic eruption and comedones are not seen, distinguishing this condition from acne vulgaris.
Wood lamp examination may demonstrate a yellow-green fluorescence.
Dermoscopy features have been described and include:
Clinical examination raises the diagnosis. Laboratory investigations on skin scraping, tape stripping, swab, or skin biopsy confirm the presence of yeasts as bacterial folliculitis and steroid acne can be clinically similar.
Diagnosis of Malassezia folliculitis is often delayed due to its clinical resemblance to:
It is important to address any predisposing factors at the outset, as Malassezia folliculitis has a tendency to recur.
Topical treatments such as selenium sulfide shampoo, econazole solution and topical ketoconazole are effective in the majority of cases but may require a longer course than systemic agents. Ongoing weekly application may be particularly useful as maintenance therapy to prevent recurrence.
Oral treatment may be more effective than topical, although results of clinical trials have not consistently shown this. Fluconazole is used more commonly than itraconazole due to its superior side effect profile.
Isotretinoin and photodynamic therapy (PDT) have been used with some success in small case series of recalcitrant disease.
Recurrence is common, even after successful treatment.
Long-term prophylaxis with topical agents may be considered in those at high-risk or with multiple recurrences.
Periodic re-evaluation of predisposing factors is recommended.