Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated September 2014. DermNet revision August 2021
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
Outlook
Pityriasis versicolor is a common yeast infection of the skin, in which flaky discoloured patches appear on the chest and back.

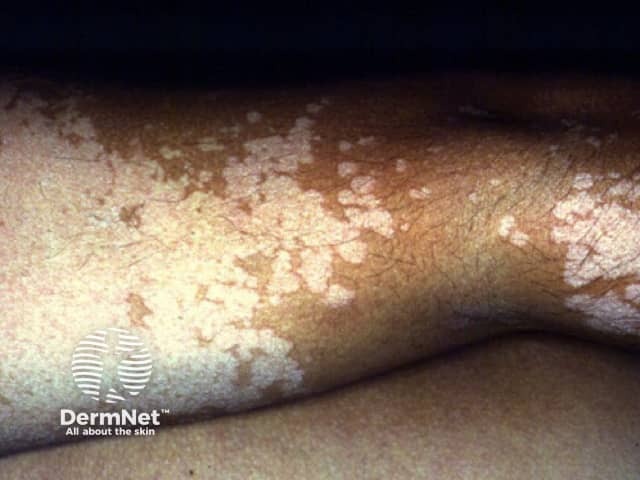

The term pityriasis is used to describe skin conditions in which the scale appears similar to bran. The multiple colours of pityriasis versicolor give rise to the second part of the name, versicolor. Pityriasis versicolor is sometimes called tinea versicolor, although the term tinea should strictly be used for dermatophyte fungus infections.
Pityriasis versicolor most frequently affects young adults and is slightly more common in men than in women. It can also affect children, adolescents, and older adults.
Pityriasis versicolor is more common in hot, humid climates than in cool, dry climates. It often affects people who perspire heavily. It may clear in the winter months and recur each summer.
Although it is not considered infectious in the conventional sense, pityriasis versicolor sometimes affects more than one member of a family.
Pityriasis versicolor is caused by mycelial growth of fungi of the genus Malassezia.
Malassezia are part of the normal skin microbiota (microorganisms found on normal skin). They are dependent on lipid for survival. Fourteen different species of malassezia have been identified. The most common species cultured from pityriasis versicolor are M globosa, M restricta and M sympodialis.
Usually malassezia grow sparsely in the seborrhoeic areas (scalp, face and chest) without causing a rash. It is not known why they sometimes grow more actively on the skin surface to form pityriasis versicolor. One theory implicates a tryptophan-dependent metabolic pathway.
The yeasts induce enlarged melanosomes (pigment granules) within basal melanocytes in the brown type of pityriasis versicolor. It is easier to demonstrate the yeasts in scrapings taken from this type of pityriasis versicolor than in those taken from the white type.
The white or hypopigmented type of pityriasis versicolor is thought to be due to a chemical produced by malassezia that diffuses into the epidermis and impairs the function of the melanocytes.
The pink type of pityriasis versicolor is mildly inflamed, due to dermatiits induced by malassezia or its metabolites.
Pityriasis versicolor affects the trunk, neck, and/or arms, and is uncommon on other parts of the body. The patches may be coppery brown, paler than surrounding skin, or pink. Pale patches may be more common in darker skin; this appearance is known as pityriasis versicolor alba. Sometimes the patches start scaly and brown, and then resolve through a non-scaly and white stage.
Pityriasis versicolor is usually asymptomatic, but in some people it is mildly itchy.
In general, pale or dark patches due to pityriasis versicolor do not tend to be more or less prone to sunburn than surrounding skin.
Hyperpigmented, hypopigmented, and pink pityriasis versicolor are usually seen as distinct variants but may sometimes co-exist. Pink pityriasis versicolor may also co-exist with seborrhoeic dermatitis as both are associated with malassezia overgrowth.
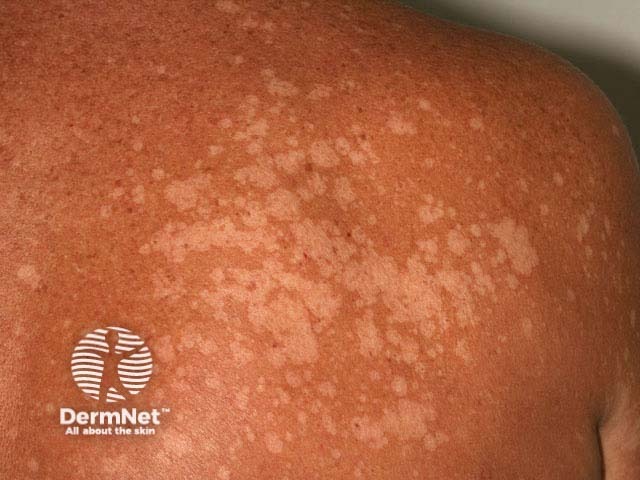
Pityriasis versicolor
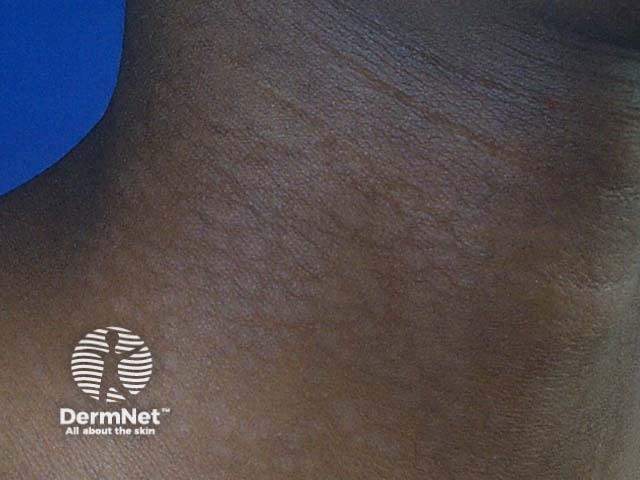
Pityriasis versicolor
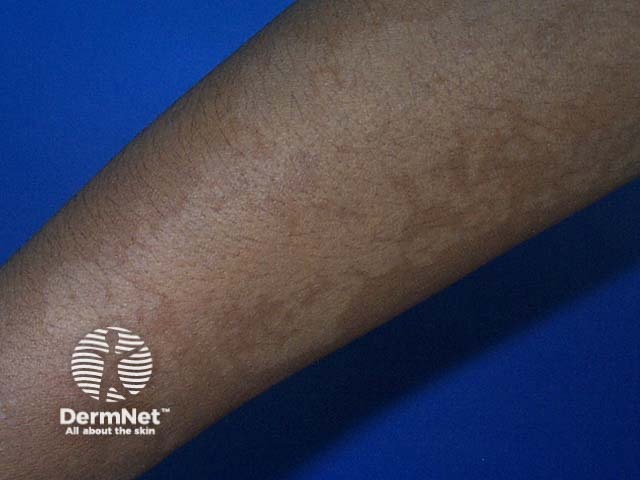
Pityriasis versicolor
See more images of pityriasis versicolor.
Pityriasis versicolor is usually diagnosed clinically. The following tests may be useful.
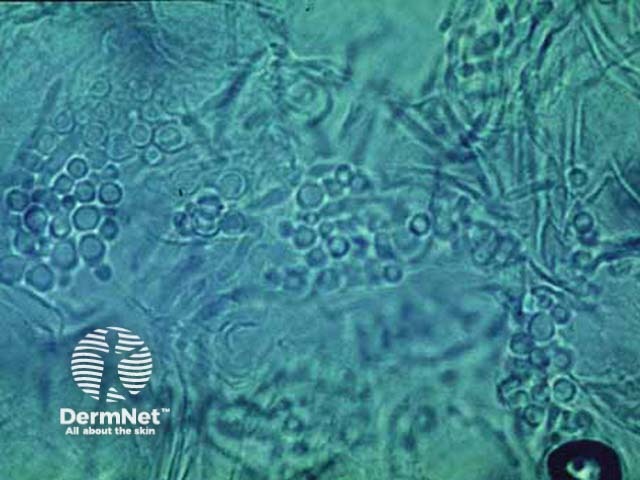
Microscopy of Malassezia furfur
Mild pityriasis versicolor is treated with topical antifungal agents.
The medicine should be applied widely to the skin from the jawline down and left on the skin for 5-15 minutes before rinsing off in the shower. This should be done daily for one week then weekly for one month.
Oral antifungal agents, itraconazole and fluconazole, are used to treat pityriasis versicolor when extensive or if topical agents have failed.
Vigorous exercise an hour after taking the medication may help sweat it onto the skin surface, where it can effectively eradicate the yeast. Bathing should be avoided for a few hours. A few days' treatment will clear many cases of pityriasis long term, or at least for several months.
Oral terbinafine, an antifungal agent used to treat dermatophyte infections, is not effective for yeast infections such as pityriasis versicolor.
Reapplication of a topical treatment such as selenium sulfide shampoo every month once the rash has cleared will usually prevent recurrence.
Pityriasis versicolor generally clears satisfactorily with treatment but often recurs when conditions are right for malassezia to proliferate. The fine surface scale is the indication of active infection and once this has disappeared, infection is no longer ongoing. The colour may persist for weeks or months, particularly the hypopigmentation, and do not indicate treatment failure.
Pityriasis versicolor often recurs when the weather becomes warm and humid again. Regular use of topical treatment minimises this risk.