Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Assoc Prof Patrick Emanuel, Dermatopathologist, Auckland, New Zealand, 2013.
Tinea corporis is a superficial dermatophyte infection caused by three types of dermatophyte infecting truncal skin, namely: Trichophyton, Microsporum, and Epidermophyton.
Well established plaques of tinea corporis typically show foci of parakeratosis with epidermal acanthosis, spongiosis, and collections of neutrophils in the upper layers of the epidermis. The dermis may display oedema and predominantly chronic inflammatory changes (figures 1, 2). GMS staining confirms the presence of septate branching hyphae are seen in the stratum corneum. Some dermatophyte species also may invade the follicular infundibulum (figure 3). Prolonged topical treatments with corticosteroids may result in attenuation of these inflammatory changes and extensive proliferation of the organisms which become easy to identify, even with routine haematoxylin and eosin stain.
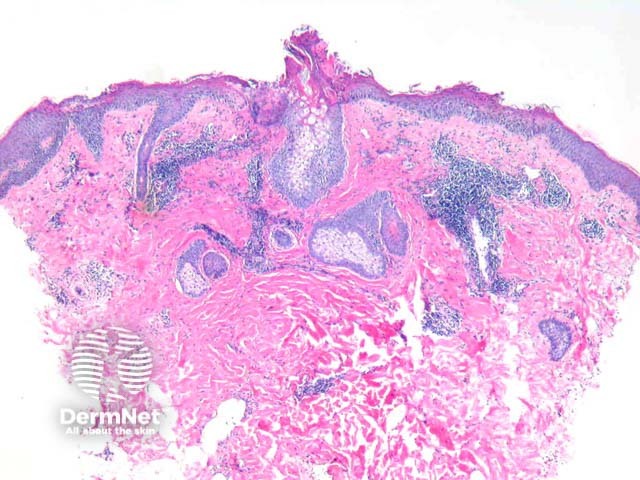
Figure 1
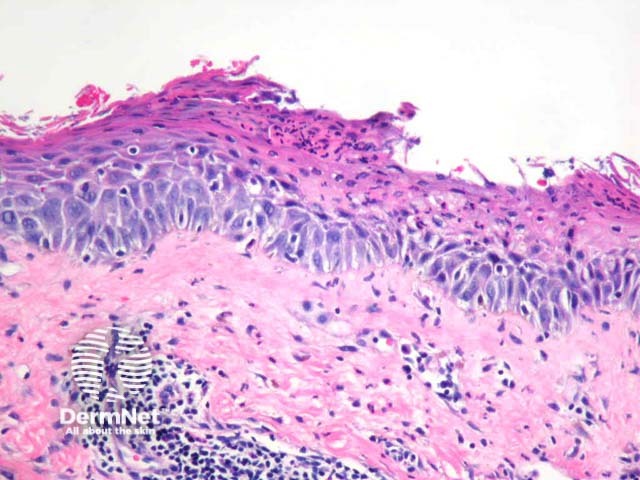
Figure 2
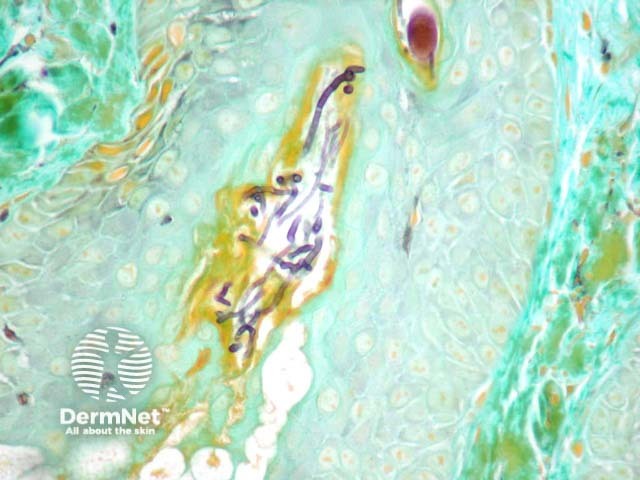
Figure 3
PAS or GMS stains (figure 3) highlight the septate branching hyphae. Interestingly, the organisms are autofluorescent with fluorescent microscopy.
Pityriasis versicolor – Malassezia (formerly known as Pityrosporum) yeasts colonise the stratum corneum and fail to elicit much of an epidermal response. Typically there is minimal hyperkeratosis and sparse lymphocytes in the dermis.
Psoriasis – Tinea corporis elicits a reaction pattern which can be exceedingly difficult to distinguish from psoriasis. Special stains and correlation with scraping and culture results may be required.
Eczema – Nummular, allergic contact, and other eczematous reactions can mimic dermatophytoses, particularly when the lesions are impetiginised and superinfected with bacteria. Special stains, scrapings, and culture studies are sometimes required for distinction.