Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, November 2015. Revised January 2021.
Introduction
Causes
Demographics
Clinical features
Different types
Complications
Diagnosis
Treatments
Pseudomonas species are Gram-negative rod-shaped bacteria widespread in water and soil. Infections of the skin or soft tissues by Pseudomonas aeruginosa and other Pseudomonas spp. range from superficial discolourations to serious and life-threatening because these bacteria are invasive and toxigenic.
Pseudomonas aeruginosa is commonly found transiently on the skin, especially in the axillary and anogenital regions, and readily colonises ulcers and moist skin. However, healthy people do not normally develop pseudomonas infection. Pseudomonas is considered to be an opportunistic infection causing serious disease in immunocompromised patients, damaged tissue, or following accidental intravenous access.
Pseudomonas species can be transmitted in hospitals due to contaminated surfaces and via hands of staff, and is responsible for approximately 10% of all nosocomial infections.
Patients at highest risk for these infections include those with:
Signs of pseudomonas infection vary depending upon the site of the infection, but can include:
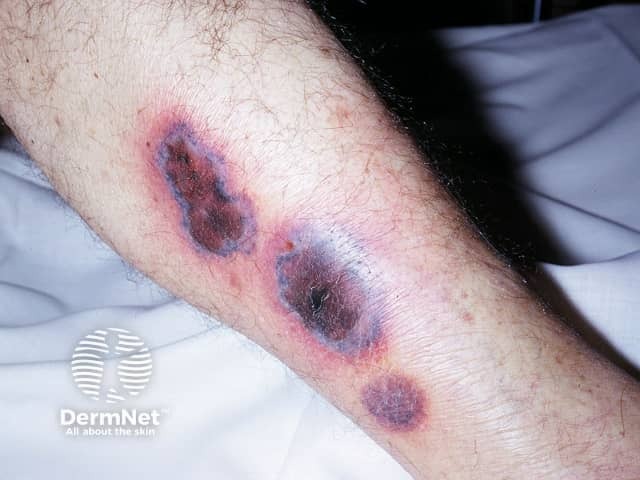
Ecthyma gangrenosum
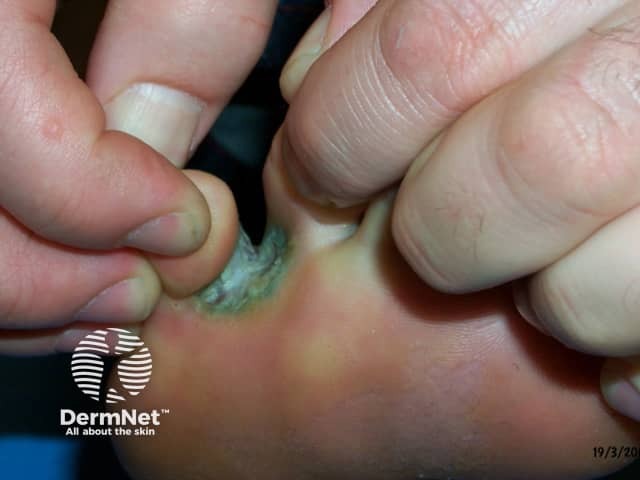
Green-tinged maceration in the toeweb space
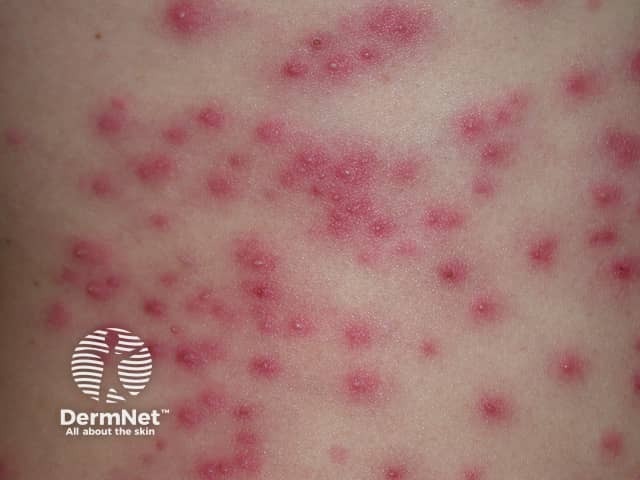
Pseudomonas folliculitis
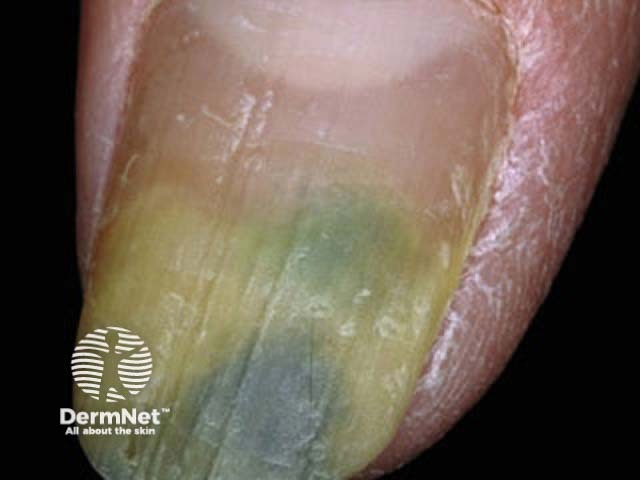
Pseudomonas infection
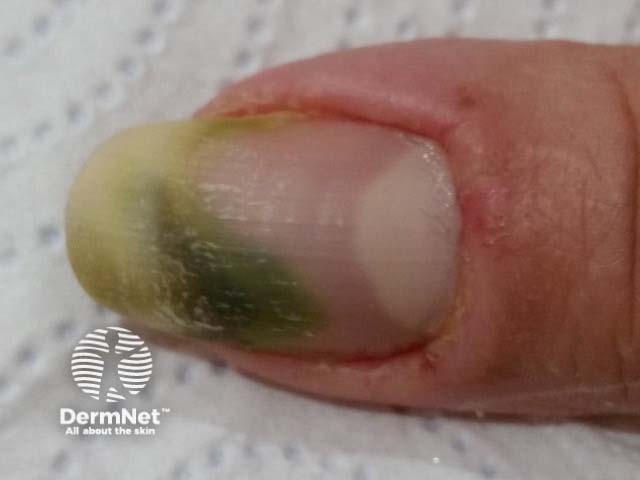
Green nail due to pseudomonas infection with paronychia
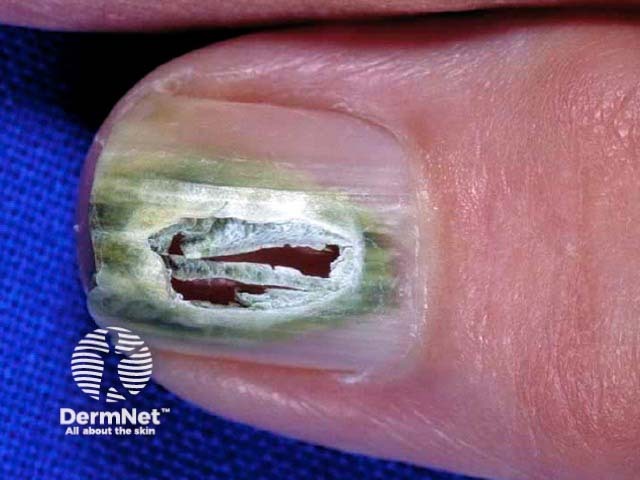
Green nail due to pseudomonas infection
The most serious complication of a pseudomonas skin or soft tissue infection is bacteraemia following contaminated intravenous fluids, drugs, or antiseptics used during placement of an intravenous line. This can be fatal.
Pseudomonas infections are suspected on physical examination when there is a a greenish or blackish, fruity-smelling discharge. They are confirmed by laboratory studies of cultures taken from the affected area.
Treatment is determined by the site of the pseudomonas infection and its severity. It may include: