Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: May, 2021
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Spa pool folliculitis, also called hot tub folliculitis or pseudomonas folliculitis, is a Gram-negative bacterial infection of hair follicles acquired during exposure to hot water such as in spa pools, hot tubs, and jacuzzis.
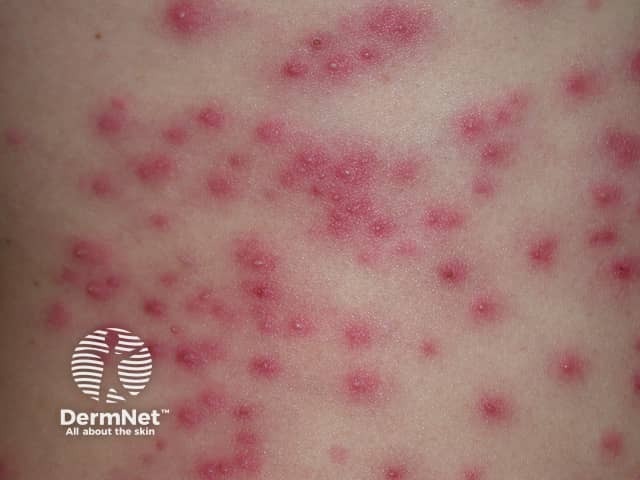
Pseudomonas folliculitis
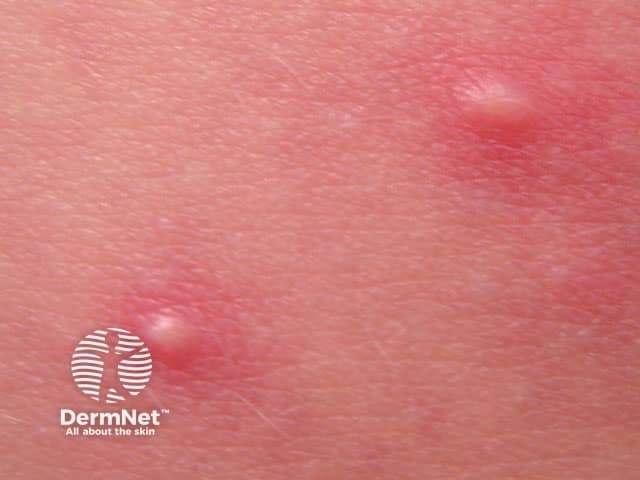
Spa pool folliculitis
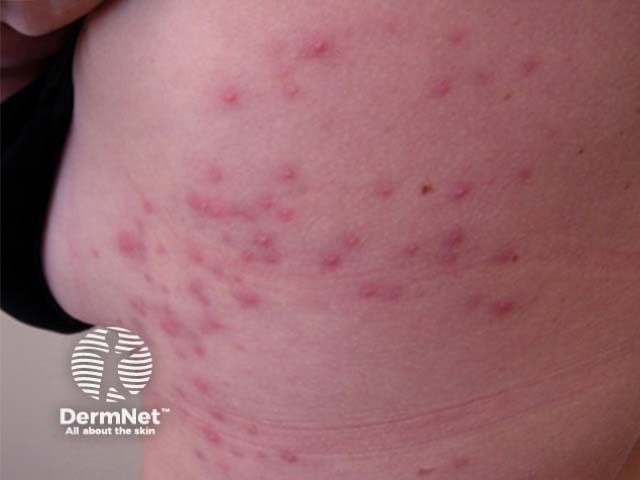
Spa pool folliculitis
Spa pool folliculitis can affect the skin of anyone who has been exposed to warm wet environments. Examples of potential exposures include spa pools, hot tubs, jacuzzi, warm water swimming pools, rehabilitation pools, floatation tanks, whirlpools, floatation aids in swimming pools, contaminated toys in the family bath tub, wet suits, and industrial closed-loop water recycling systems. The longer the duration and frequency of exposure the greater the risk.
Spa pool folliculitis predominantly affects females. All age groups and races can develop the condition following exposure. Immunocompromised patients may be predisposed to rapid skin colonisation by Gram-negative bacteria. However, not all exposed individuals develop the infection, perhaps reflecting the duration of exposure, sex, and skin microflora.
Spa pool folliculitis is due to an opportunistic bacterial infection of the skin by Pseudomonas aeruginosa or, less commonly, Aeromonas hydrophila. These ubiquitous Gram-negative bacteria can survive in warm water, even when adequately chlorinated, because of the formation of a biofilm on the tub surface or within the piping system. Contamination is more common if the water is inadequately treated or organic material, such as skin, is present.
It is hypothesised that water absorption into the stratum corneum increases proportionately with the time submerged in water, enhancing permeability to bacteria.
Spa pool folliculitis presents as a sudden eruption of scattered red macules that evolve into papules and pustules centred on hair follicles. The onset is generally between 8 hours and five days after exposure. Areas of skin covered by swimwear, such as the buttocks, are most prone to develop the rash. Itch, pain, and a burning sensation are common. Swollen tender lymph glands may develop.
Pseudomonas aeruginosa can also cause ‘hot hand-foot syndrome’ (hot-foot syndrome) presenting as tender or painful red nodules on the palms and/or pressure-bearing areas of the soles of the feet, particularly in children, which may develop at the same time as the folliculitis.
Some people with spa pool folliculitis feel unwell, with the most common symptoms being malaise/fatigue, headache, low-grade fever, earache, sore throat, abdominal discomfort, nausea, vomiting, and diarrhoea.

Spa pool folliculitis
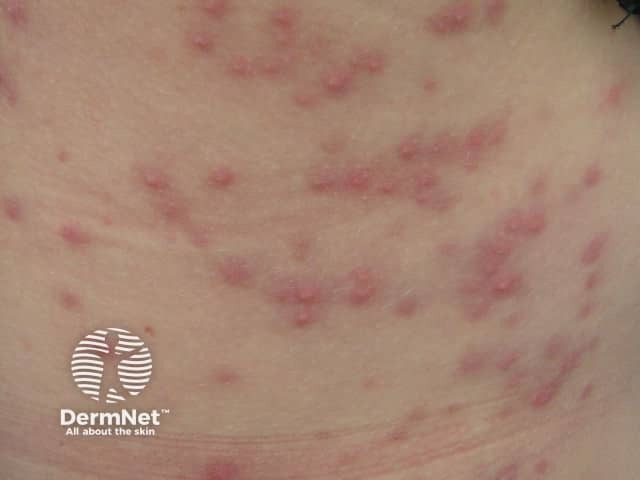
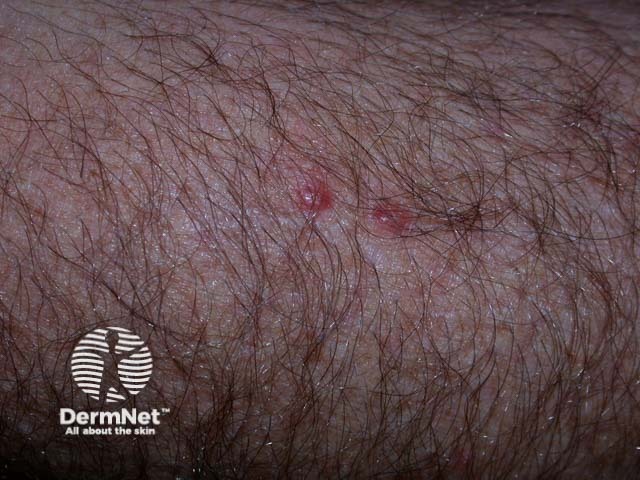
Spa pool folliculitis
The erythema of spa pool folliculitis may be difficult to appreciate in skin of colour. Postinflammatory hyperpigmentation is common in darker skin types.
Spa pool folliculitis is usually diagnosed based on the history of exposure and the clinical features.
Gram stain of a smear taken from pustules will show Gram-negative (pink/red) rods. Culture and antibiotic sensitivities should be reported as isolates may show resistance to multiple antibiotics.
Skin biopsy of the folliculitis is not usually required. Histology is morphologically identical to malassezia folliculitis pathology without the yeast. Biopsy of the hot hand-foot syndrome nodules is reported to show neutrophils around blood vessels, eccrine sweat glands, and other skin adnexae in the dermis and subcutis.
The source of infection may be confirmed by microbiological assessment of the water, pool surfaces, filter, and pipes.

Superficial bacterial folliculitis
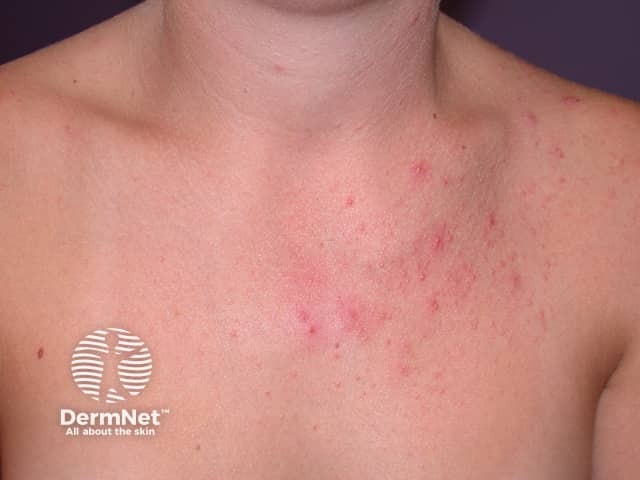
Malassezia folliculitis
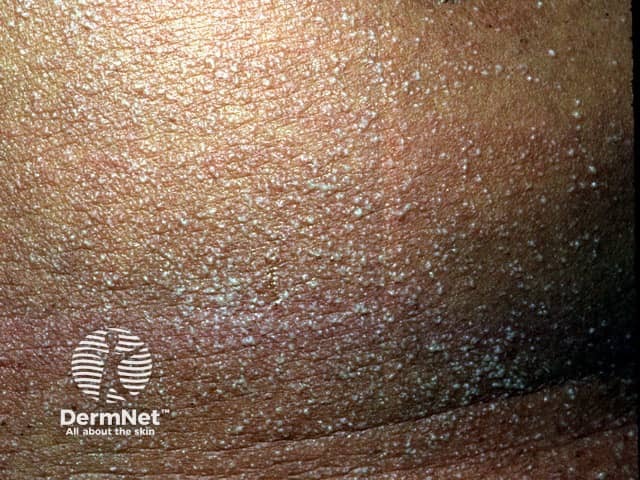
Miliaria
Spa pool folliculitis is best treated by avoiding the source of infection. The responsible pool should be properly cleaned and disinfected.
A topical skin antiseptic and/or oral antibiotics may sometimes be required.
Spa pool folliculitis is usually self-resolving within 14 days without sequelae.
Recurrences may occur if the source of the infection is not identified and treated/avoided.