What is a septic embolus?
A septic embolus is a blood clot containing bacteria that has become dislodged and travelled through the bloodstream. Septic emboli become trapped in small terminal blood vessels, blocking them.
Septic emboli damage the body tissues in two ways:
- completely or partially reduce the blood supply
- introduce an infectious agent into an ischaemic site.
Septic emboli are a consequence of infection and their diagnosis should always prompt a search for the primary source.
Who gets septic emboli?
Septic embolic occur in people at increased risk of infections, particularly of the heart lining and blood vessels. These include:
- Older people
- People with prosthetic heart valves
- Those with a weakened immune system due to human immunodeficiency virus infection (HIV), immunosuppressant drugs, or leukaemia
- Injecting-drug users
What causes septic embolisation?
Septic emboli come from a site of infection, where bacteria are present in large numbers and various inflammatory processes and turbulent blood flow increase the likelihood of clot formation. An infected clot, or a small fragment of a clot, becomes dislodged and comes to rest at a distal location. Local tissue damage occurs due to the combined effects of ischaemia (lack of oxygen supply) and infection.
There are various sources of septic emboli.
- Infective endocarditis – this is an infection of the heart valves and lining of the heart muscle. Embolisation is particularly likely when infection is due to Staphylococcus aureus.
- Skin or soft tissue infection – this may occur after having a peripheral intravenous line inserted for long periods. Risk of developing septic embolisation from a superficial wound is very low. The risk is increased when the infection involves blood vessels (phlebitis) and pus is present.
- Mouth or gum infections and abscesses.
- Artificial prostheses – these include pacemakers, heart valves, and central venous catheters.
- Deep venous thrombosis clot formation in the legs, due to thickening or slowing of blood – which subsequently becomes infected.
What are the clinical features of septic emboli?
People with septic emboli tend to exhibit classic but non-specific signs of infection, including fever, fatigue, and an increased heart rate. There have been reports of asymptomatic primary infection and subsequent septic embolisation, particularly from the spleen.
The specific clinical findings of septic embolisation depend on where the clot gets lodged. This may include any part of the body, such as the lungs, causing lung infections and accesses, or the skin, causing distinctive painful lesions.
Skin manifestations include:
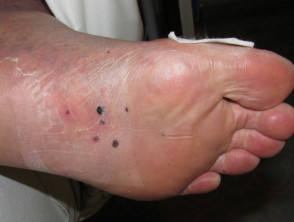
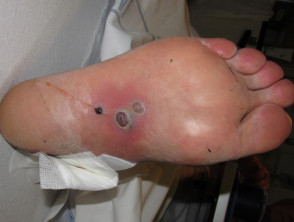
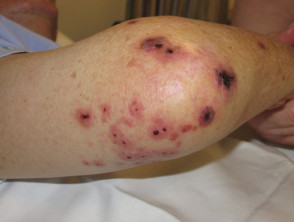
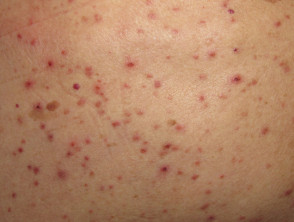
- Small, red or purpuric spots, which are typically located on the hands and feet but may become generalised. They are flat or slightly raised and tend to be painful. They do not blanch under pressure. They may contain pus.
- Blue toe syndrome
- Osler nodes and Janeway lesions are classic descriptors of skin findings where septic emboli originate from infection in the lining of the heart muscle.
Emboli may affect internal organs:
- Brain (abscess, meningoencephalitis and stroke)
- Spleen
- Liver
- Kidney
- Lungs (pneumonia, pneumonitis, or lung abscess)
- Bone (osteomyelitis) and joints (septic arthritis)
- Eyes (bleeding within the eye causing blurred vision).
Septic emboli
How is the diagnosis of septic embolus made?
The diagnosis of septic embolisation requires investigation to confirm and find the source.
Blood tests
- An increased number of white cells is a non-specific sign of bacterial infection.
- Blood cultures may reveal bacteria.
- Skin biopsies may show clot occlusion with abundant neutrophils in blood vessels within the deep layer of the skin.
Imaging
Establishing the source of the septic emboli is the key to diagnosis. While some potentially causative infections may be diagnosed clinically, others require more extensive investigation.
- Ultrasound imaging of the heart may reveal infective endocarditis.
- Computer tomography (CT) and magnetic resonance imaging (MRI) scans can show larger blood clots in the lungs, and tissue death in various sites due to blockage of a blood vessel by embolism.
- Angiograms can reveal septic embolisation within blood vessels or the heart.
What is the treatment for septic emboli?
The mainstay of treatment is to control the original source of infection. How this is best achieved depends on the source and may include:
- Wound debridement or drainage of an abscess
- Removal and/or replacement of infected prostheses
- Intravenous antibiotics.
What is the longterm outcome of septic emboli?
Septic embolisation may be a mild or very severe condition, and the long-term outcome depends on which organs are involved, the severity of the precipitating infection, and the general health of the patient preceding the infection.
In healthy people, or those with only mild infection and cutaneous emboli, active treatment of the primary source of infection is often sufficient to clear disease and prevent further septic embolisation.
Where septic emboli have caused extensive infection of the limbs, gangrene may develop. This may necessitate amputation of affected areas.
Involvement of internal organs, particularly lungs and brain, may progress to overwhelming systemic infection (sepsis) and death. Involvement of internal organs does not preclude full recovery however the treatment course is often long and difficult.