Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Cutaneous adverse reactions to medications are common; many are non-immunological in nature. This quiz considers some drug eruptions believed to be immunologically-mediated ('drug allergy'), or that are at least idiosyncratic in nature.
Often it is difficult to be certain whether a rash is due to drug, a skin disease or an underlying illness. A careful drug history is essential, considering prescription and over-the-counter medicines, topical agents, herbal remedies and supplements. Previous exposure, dose, duration and frequency of drug administration should be established. Refer to standard textbooks and obtain specialist advice from a dermatologist as necessary.
For each of the ten cases, study the image(s) and then answer the questions. You can click on the image to view a larger version if required.
Each case should take approximately 2 minutes to complete. There is a list of suggested further reading material at the end of the quiz.
When you finish the quiz, you can download a certificate.
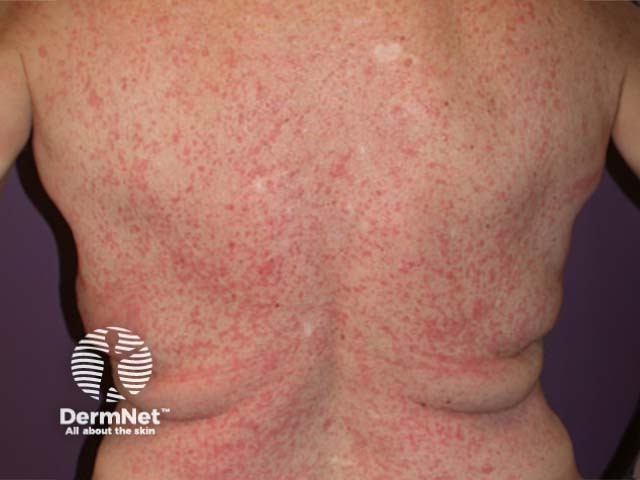
Name this skin condition.
Morbilliform eruption due to amoxicillin
What are its clinical features?
Morbilliform (measles-like) eruptions (figure 1) are the most common pattern, but may be indistinguishable from toxic erythema or exanthem due to bacterial or virus infection. Fever and enanthem (mucosal lesions) suggest an infective cause.
Widespread symmetrical erythematous macules (small flat lesions), patches (large flat lesions), papules (small bumps) and/or plaques (large indurated areas) are most prevalent on the trunk and proximal limbs. Itch can be absent, or mild to severe. The skin often peels off as the rash resolves.
Morbilliform eruptions typically develop within two weeks of exposure to the drug. The drug should be stopped to prevent progression to exfoliative dermatitis / erythroderma. Late onset accompanied by eosinophilia, fever and internal organ involvement suggests drug hypersensitivity syndrome, which is fatal in around 8% of cases.
Sometimes the rash resolves despite continuing the responsible drug, and it may not always recur on re-exposure.
Management should include emollients and mild to moderate potency topical steroids. Systemic steroids are not usually required, but are mandatory for drug hypersensitivity syndrome.
List drugs that are commonly responsible.
The list of possible culprits is too long to list here! Antibiotics are the most common.