Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. December 2016.
Introduction
Demographics
Causes
Clinical features
Treatment
Outcome
Buschke–Ollendorff syndrome refers to a rare, hereditary disorder affected the connective tissues. It is also known as dermatofibrosis lenticularis disseminata, dermato-osteopoikilosis and familial cutaneous collagenoma.
Buschke–Ollendorff syndrome occurs in 1 in every 20,000 live births worldwide. There appears to be no racial, sexual or geographical predilection. Lesions are present at birth.
Buschke–Ollendorff syndrome is a genetic disease. The underlying cause of Buschke–Ollendorff syndrome is mutation of the LEMD3 gene, which provides instructions for the making of proteins that support connective tissues.
Buschke–Ollendorff syndrome is characterised by small connective tissue naevi.
Non-cutaneous but significant features of Buschke–Ollendorff syndrome include:
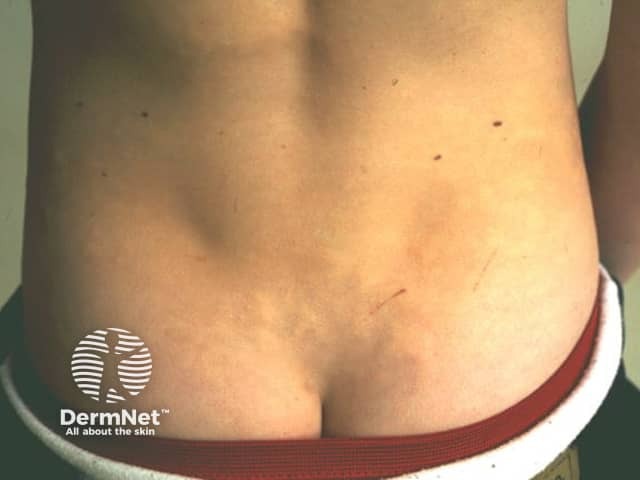
Conenctive tissue naevus in Buschke Ollendorf syndrome
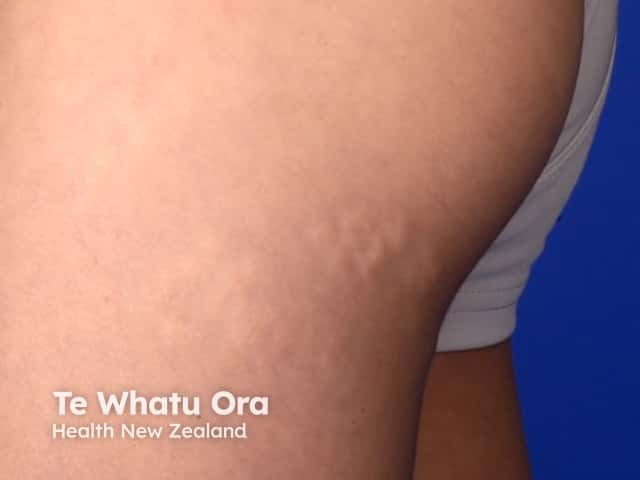
Connective tissue naevus
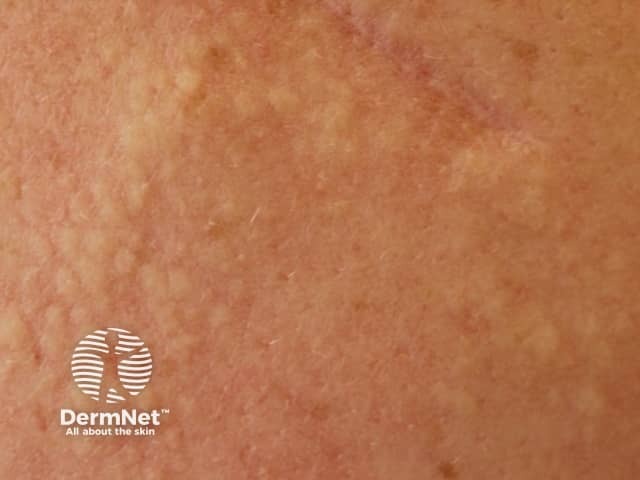
Connective tissue naevus
The treatment of Buschke–Ollendorff syndrome may involve:
The outcome for Buschke–Ollendorff syndrome depends on the associated disorders.