Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Ellen Mooney, MD, Director of the Nordic Institute of Virtual Dermatopathology, 2018. Updated by: Dr Rajendra Singh, MD, Director of Dermatopathology, Summit Health and Dr Ellen Mooney, MD August 2022.
Introduction
Benefits
Uses
Disadvantages
Diagnostic accuracy
Whole slide imaging is the software manipulation of digital images of tissue sections that have been scanned at various magnifications. This enables the viewer to zoom in on areas of interest, thereby simulating the examination of glass slides under a traditional microscope. Magnifications of up to × 60 can be achieved. A few modern scanners can also do x 100 for blood smears and bone marrow aspirations.
Whole slide imaging is also called virtual microscopy.
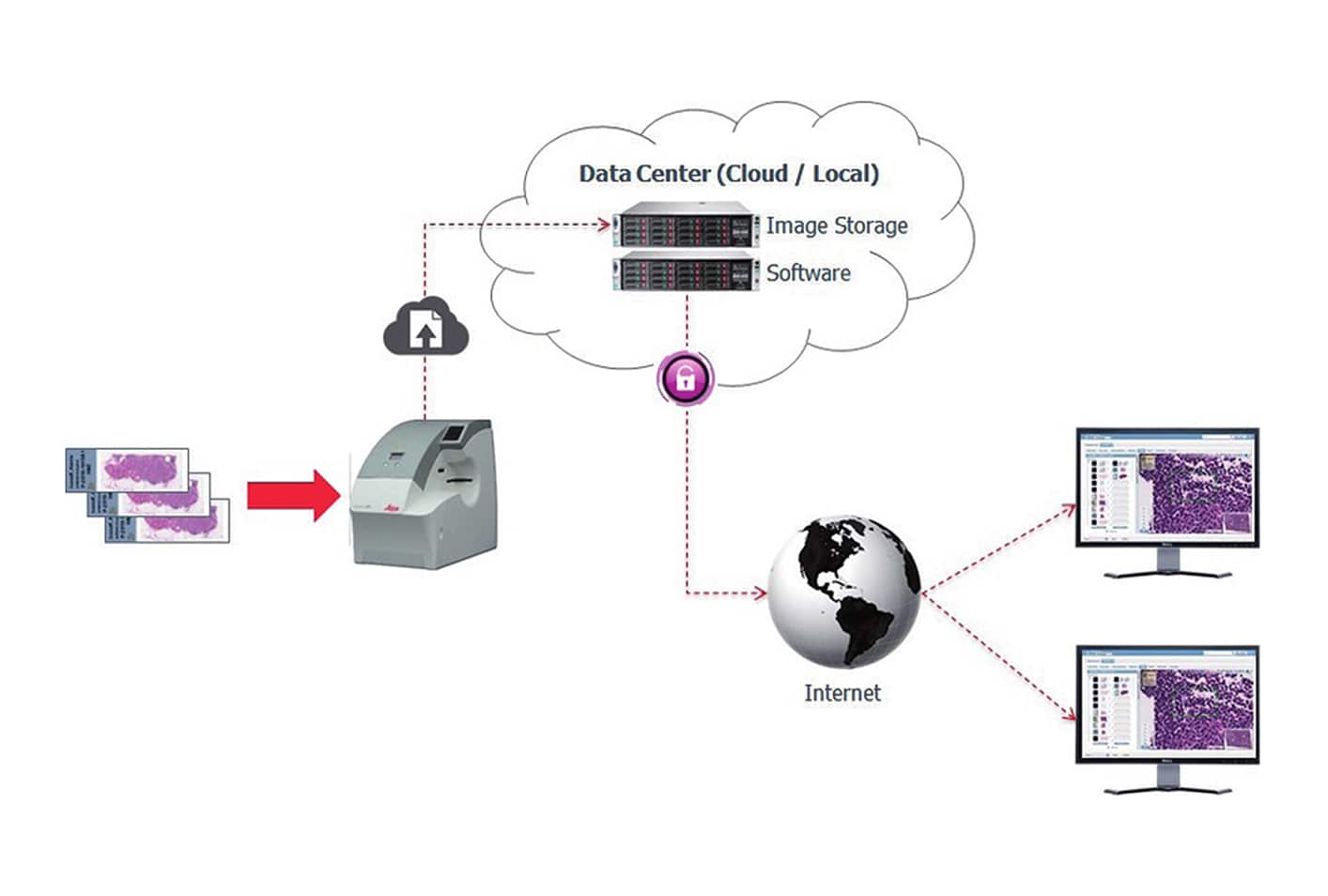
Whole slide image production and sharing Courtesy of Colin Doolan Leica Biosystems 2
Advantages of using whole slide digital images for microscopic examination of pathology specimens include:
The US Food and Drug Administration (FDA) permitted the marketing of whole slide imaging systems for use in pathological diagnosis in April 2017.
Dermatopathology is ideally suited to whole slide imaging for diagnoses, due to high case volume, low slide count and small specimen size in this speciality.
Computers are now readily available in educational institutions and are less costly than microscopes.
Whole slide imaging is also useful in continuing medical education (CME) or continuing professional development (CPD) and external quality assurance (EQA). The incorporation of examinations with integrated multiple-choice questions makes it possible to accrue CME credit online. Accruing CME credit is becoming increasingly important for specialists. In some countries, it provides higher salaries, as is currently the case in Europe. In other countries, it is necessary for renewal of licensure and maintenance of speciality certification and is mandatory. The latter is already the case in the USA, along with mandatory certification examinations.
Digital pathology has been proven globally to be a strong tool for CME, CPD, and EQA-type programmes. Several key organisations, including the College of American Pathologists, the American Society for Clinical Pathology and the Royal College of Pathologists of Australasia, are already using digital pathology to deliver accredited CME exercises. In 2013-2015, the European Academy of Dermatology and Venereology offered their members a quarterly Clinico-Pathological Self-Assessment Module with whole slide imaging.
The American Society of Dermatopathology has an interactive case study of the month, which uses whole slide images with multiple choice answers and explanations: asdp.org/education/case-study-of-the-month/case-archive
In addition, a number of pathology subspecialty EQA programmes in the UK use digital pathology.
Consultation between pathologists and clinicians around the globe is easily manageable. Suitable software allows the incorporation of the following with the slide data:
To view as an example of whole slide imaging, click on the sample dermatopathology image below.
Some institutions use whole slide imaging for filing purposes.
Disadvantages of whole slide imaging may include:
Studies of diagnostic accuracy using whole slide imaging have been done, comparing use of glass slides to digital slides as well as photomicrographs to digital slides. See references below. This is not a comprehensive list.