Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Erysipelas, cellulitis and many cases of necrotising fasciitis are most frequently caused by Streptococcus pyogenes, less often by Staphylococcus aureus, enterobacteriae and anaerobes. Identification and early treatment is essential to prevent septicaemia, skin necrosis and permanent tissue damage.
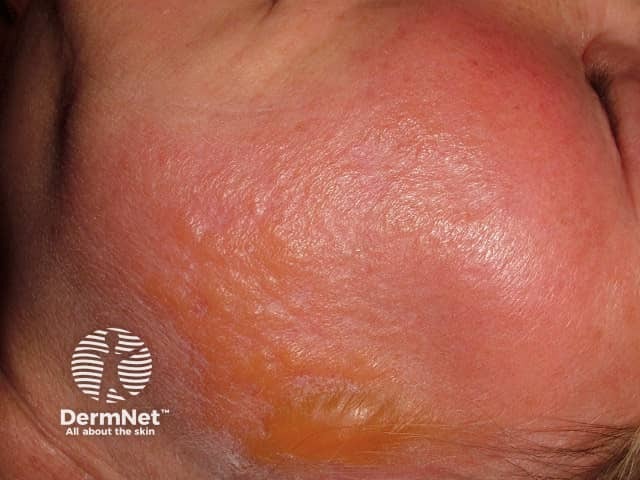
Invasive streptococci result in erysipelas (superficial lymphatic invasion) and cellulitis (involvement of subcutis). Erysipelas has elevated sharply demarcated borders. Cellulitis is less well defined and is sometimes due to other organisms, but the distinction is somewhat arbitrary.
Early infection is characterised by fever, rigors and malaise. There may or may not be a history of initial skin injury. Although any site may be affected, the face, hands and lower legs are the most common. The affected skin becomes red, hot, swollen and painful. In severe cases, there may be bullae, ulceration and necrosis. There may be associated lymphangitis and lymphadenopathy.
Erysipelas Erysipelas Erysipelas Erysipelas Erysipelas Erysipelas 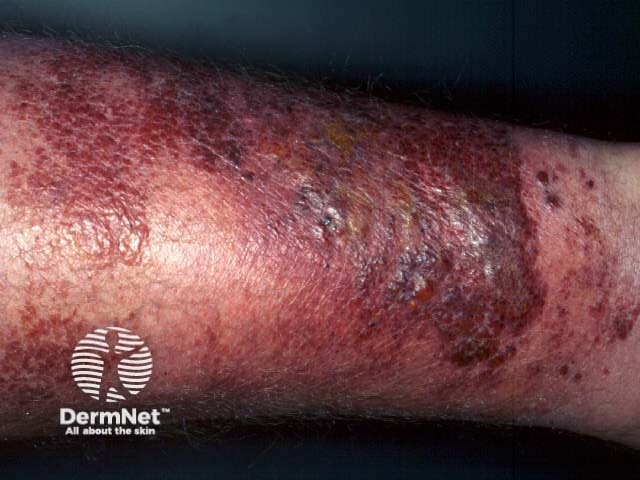
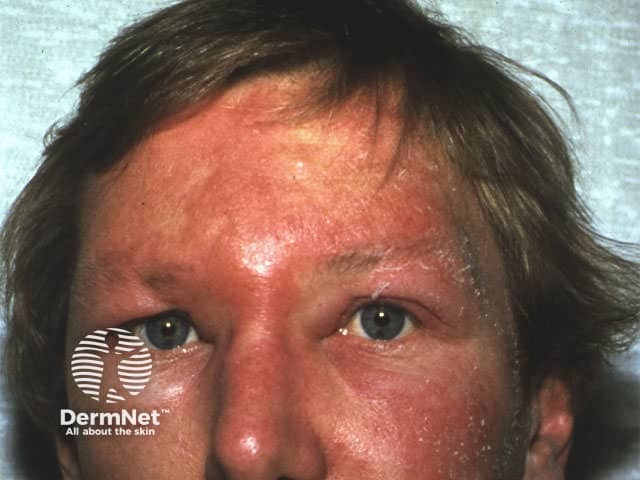
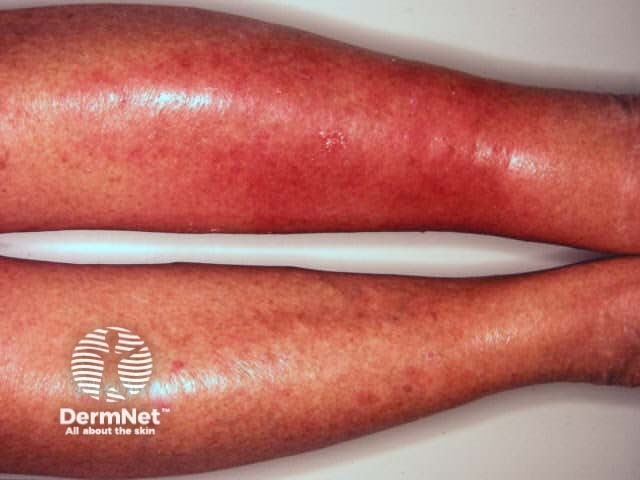
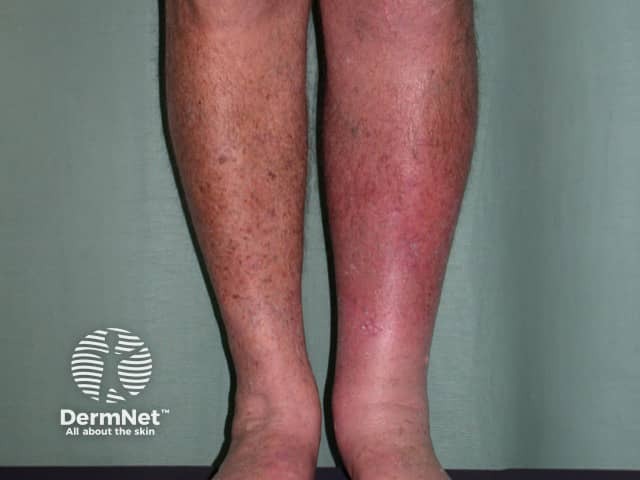
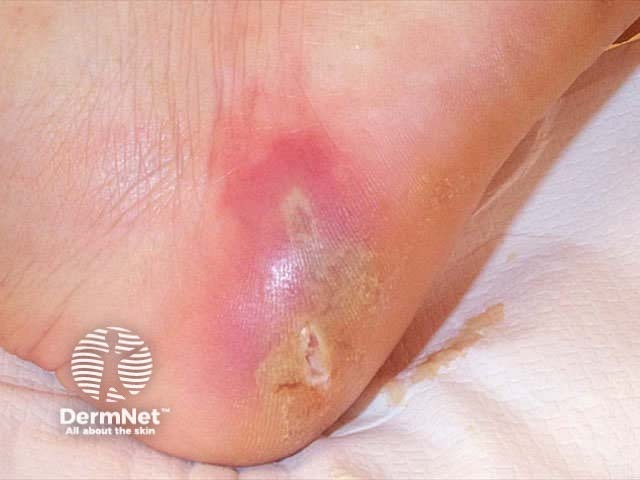
The differential diagnosis of cellulitis/erysipelas includes contact dermatitis, gravitational dermatitis, vasculitis, thrombophlebitis and deep venous thrombosis.
Contact allergy, especially to plants, may cause considerable oedema. Characteristically, plant allergy results in an asymmetrical and bizarre eruption with surface blistering. Affected patients (often children) are systemically well and the face is a common site.
Also known as venous or stasis eczema, this has a slower onset than cellulitis, does not cause systemic upset and is frequently bilateral. Surface skin may be blistered, but is often dry and intensely itchy. Look for other signs of venous disease (varicose veins, pigmentation, brawny induration).
Look for purpuric papules, plaques, bullae and erosions.
Evaluate superficial vasculature; thrombophlebitis results in a tender red or purple subcutaneous 'cord' and associated swelling.
Pain and swelling without redness or blistering. Positive Homan's sign.
Cellulitis may coexist with these disorders. If in doubt, treat for infection. It is quite safe to prescribe additional potent topical steroid for a few days. Arrange vascular studies if clinically indicated.
Surface swabs are generally negative
Streptococcal infections must be treated aggressively as they are potentially fatal. Group A streptococci are uniformly sensitive to penicillin and improvement is usually seen within hours of treatment.
Follow up carefully. If there is no improvement within 24 hours of oral treatment, consider intravenous antibiotics and if necessary, admission.
Erysipelas and cellulitis may recur in the same site and prolonged courses of penicillin are sometimes prescribed prophylactically. Treat tinea pedis actively, as fissured toe clefts appear to predispose to recurrence. Prophylactic compression stockings may be helpful for persistent lymphoedema.
Outline the criteria for hospital admission of a patient with cellulitis.
Information for patients
See the DermNet bookstore