Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Describe:
Name:
The predominant cutaneous symptom is itch (pruritus). Itch can be localised or generalised, intermittent or continuous. It can occur in the absence of skin disease but is more frequently caused by a dermatological problem. Little is known about the mediators or the neurological processes involved in either the detection of an itch stimulus or the induction of the main response to itch, scratch. Symptom control remains unsatisfactory.
Pain is experienced when the integrity of the skin is broken but may also result from a neuropathic stimulus, as in various forms of neuralgia. It is described as stinging, burning, rawness, stabbing, boring, sharp or dull. Neuropathic symptoms may be accompanied by altered sensation (dysaesthesia), often hyperaesthesia.
Itch is a subjective and variable sensation resulting in scratching. Although itch is mostly unpleasant, scratching is a pleasure, perhaps because the pain of scratching reduces the itch.
Peripheral nervous system
There are complex chemomediators on free nerve endings transmitted by C–fibres. It is possible that itch is low intensity pain at dermoepidermal junction, but specific itch fibres and nerve endings are now considered more likely. Mechanical and electrical stimuli and chemicals including histamine and substance P may induce itch.
Central nervous system
Itch activates a cerebral network resulting in a strong motor effect – itch provokes scratch, whereas pain results in withdrawal from the painful stimulus. Lesions of the lateral spinothalamic tract disrupt itch, pain and temperature sensations. Itch can be induced by centrally acting serotonin and opioids.
History should determine what areas are affected by itch and its severity, exacerbating and relieving factors and the time course of the symptoms and signs.
Examine the patient's skin all over and note the distribution of the itch/rash. Identify primary and secondary skin lesions. Scratching results in picked or linear excoriations, bruises and broken-off hair. Nails used for rubbing appear highly polished.
Perform a full medical examination, particularly if there appears to be generalised itch without a primary skin rash.
Laboratory tests could include swabs and scrapings for viral, bacterial, fungal culture if infection is possible. Consider the possibility of scabies and look for burrows along the sides and between the fingers and on the wrists. Perform microscopy on the contents of a burrow.
Skin biopsy of a typical primary lesion may be very helpful but these can be hard to find – pathology of a scratched spot shows non-specific inflammatory and healing changes and could be misleading.
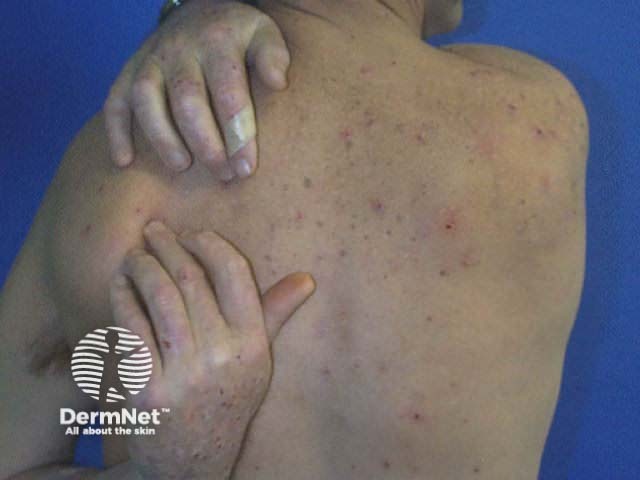
Excoriations but no primary lesions Excoriated dermatitis Rubbing the skin resulting in bruising 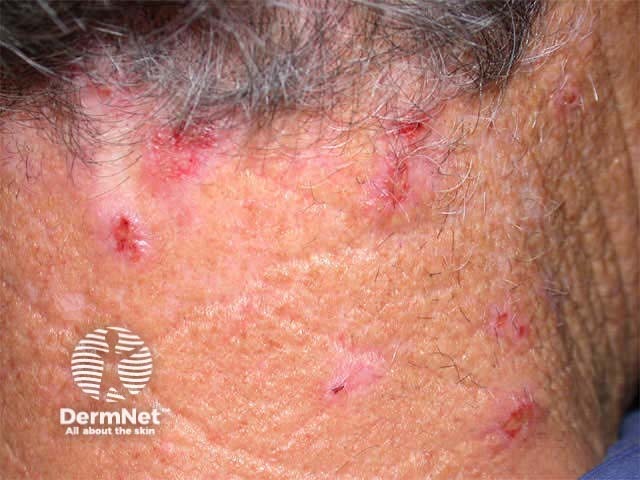
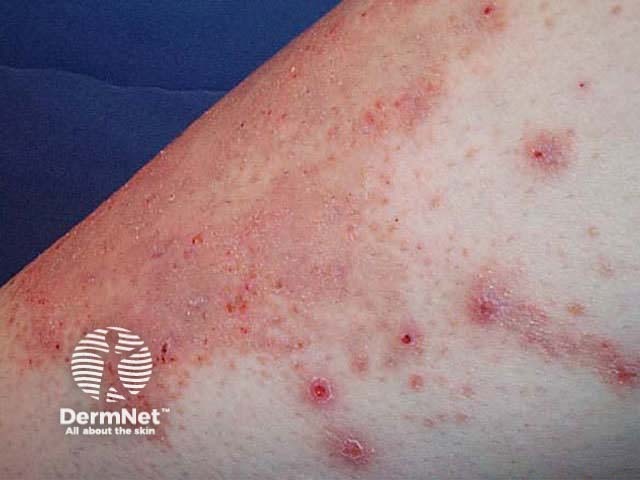
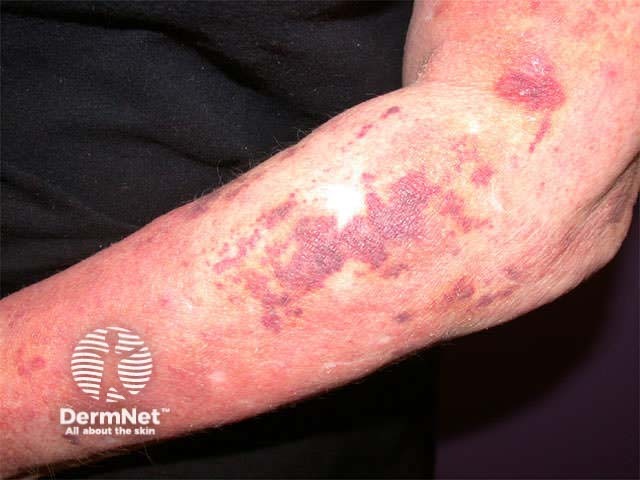
Laboratory tests are indicated if there is generalised pruritus without an obvious primary skin rash. The range of tests should include as a minimum:
A chest X-ray may be indicated if there are pulmonary symptoms or signs or unexplained lymphadenopathy.
In most cases itch is related to an inflammatory condition affecting the skin, although sometimes the itch appears to be caused or at least aggravated by scratching (the itch-scratch cycle). Effective treatments may include emollients, topical steroids and oral antihistamines.
These conditions can occur on any site:
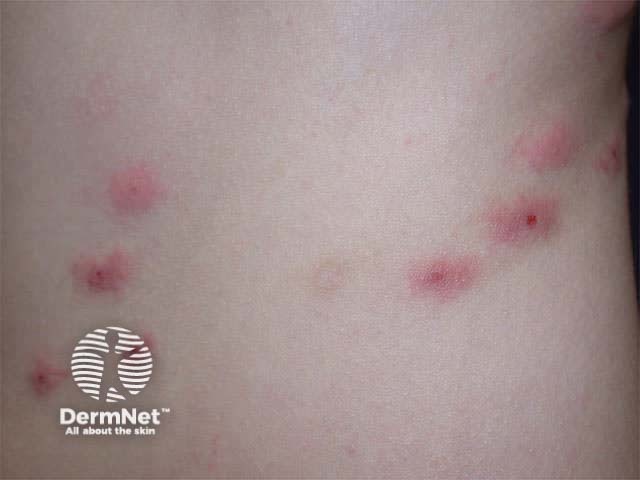
Excoriated insect bites
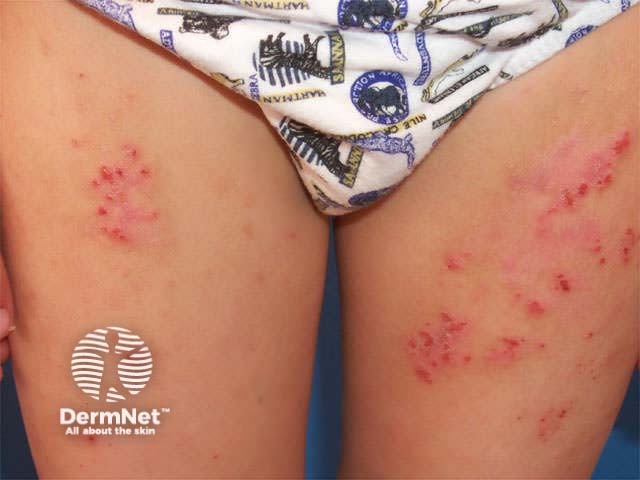
Excoriated atopic dermatitis
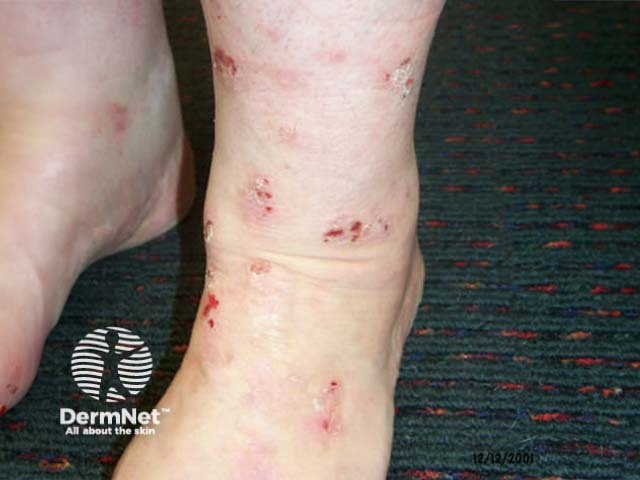
Excoriated nodular prurigo
Localised itch with no primary rash may be due to nerve root impingement resulting in dermatomal neuropathic pruritus. Scratching or rubbing the affected areas may result in secondary hyper/hypopigmentation and lichen simplex (localised lichenified eczema).
Treatment may include non-steroidal anti-inflammatory drugs, tricyclic antidepressants such as amitriptyline and physiotherapy.
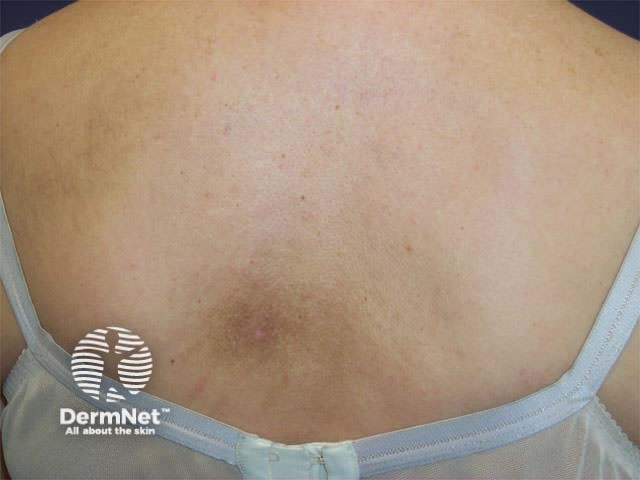
Notalgia paraesthetica
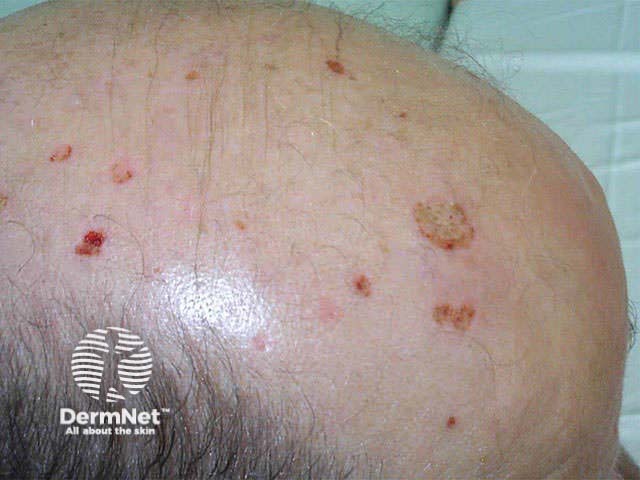
Postherpetic neuralgia
Some regions are particularly prone to chronic itching.
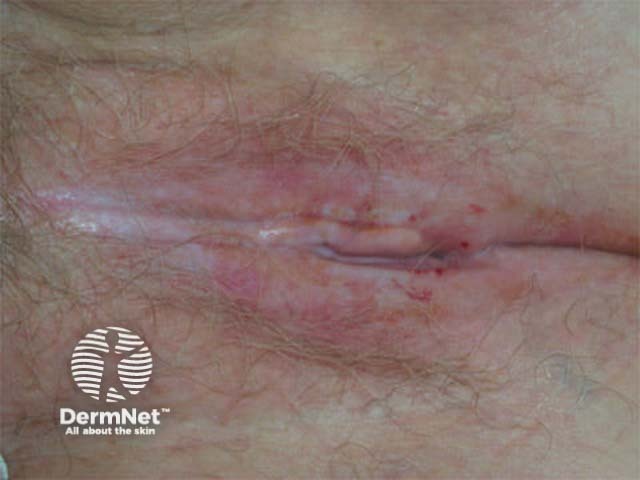
Pruritus vulvae

Pruritus ani
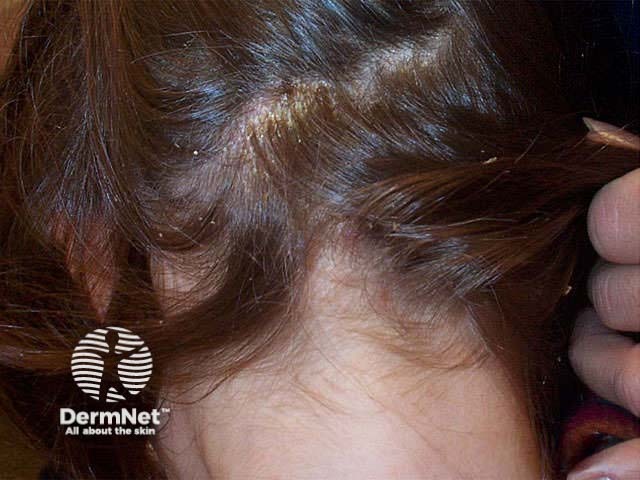
Scalp itch
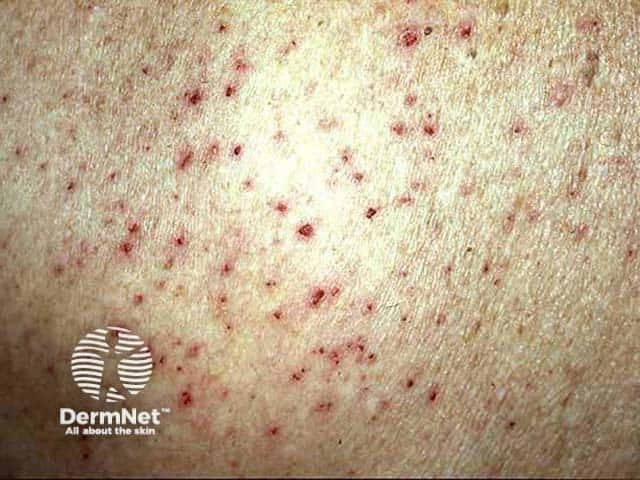
Excoriations
A few primary skin disorders are intensely itchy even when there isn't much rash to see.
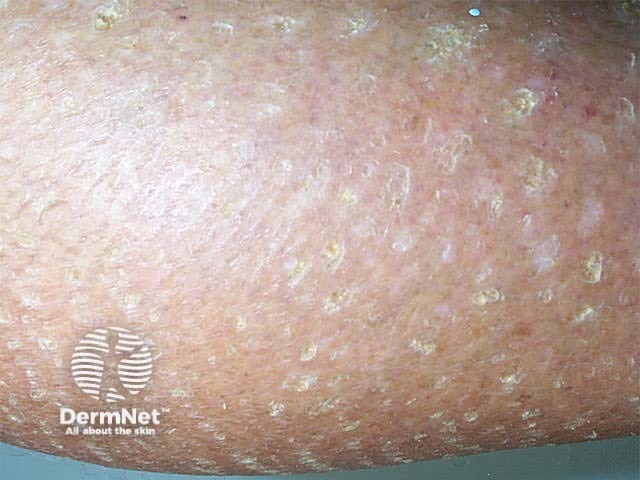
Dry skin can be itchy
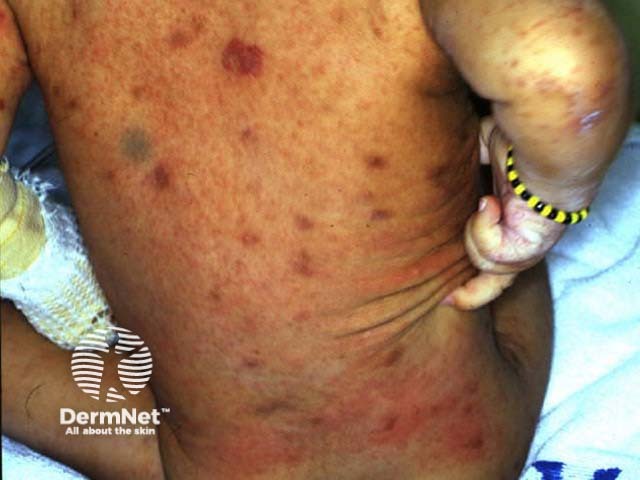
Scabies
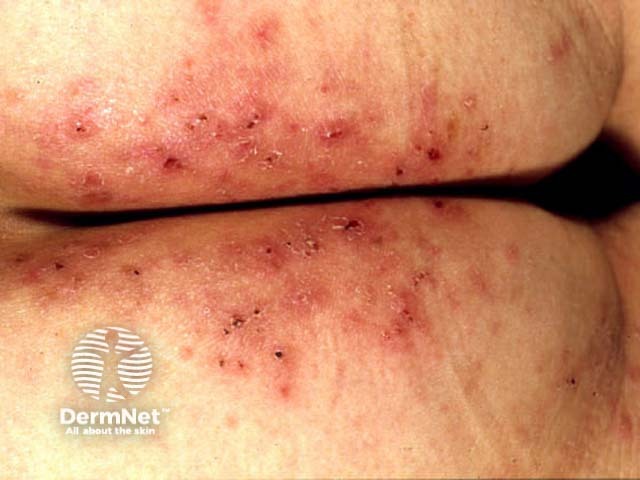
Dermatitis herpetiformis
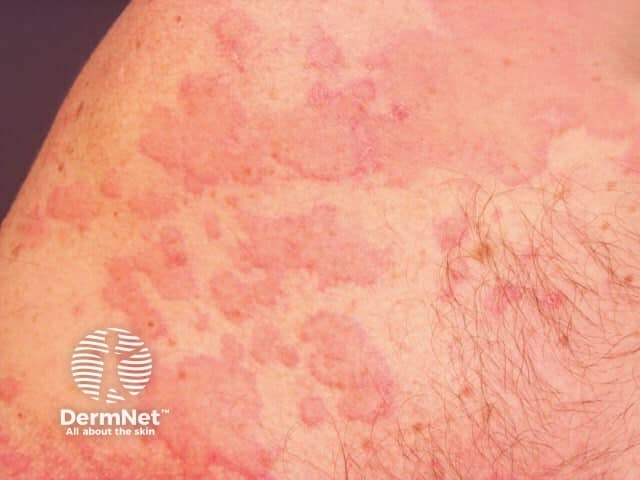
Urticaria
Itch may due to various systemic diseases, but in most cases the mechanism is not understood and symptoms may be very severe. Increased opioidergic tone may have a role.
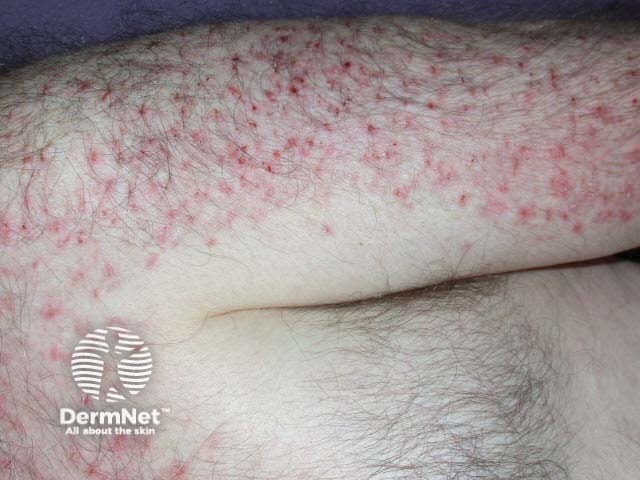
Pruritus associated with
Chronic renal failure
Clearly it is important to identify the cause and treat the primary skin condition and dermatitis, which may be secondary to scratching and rubbing. General measures include:
Specific topical antipruritic agents include:
Oral agents
Pain obviously arises when the skin is injured or from a painful infection or skin disease. Pain information is conveyed by a peripheral system of slow unmyelinated C and faster myelinated A-delta neurons. The cell bodies of these fibres exist in the posterior (dorsal) roots of the spinal cord. They extend another process into the spinal cord itself and bundles of these form Lissauer's tract. The fibres terminate in the dorsal horns of the spinal column. Secondary neurons then convey pain information to centres in the brain-stem, thalamus and cerebral cortex.
Biochemical mediators released as a result of tissue injury (noxious stimuli, mechanical injury and extremes of temperature) have been implicated in nociceptive activation and sensitisation (hyperalgesia). These mediators include serotonin, bradykinin, histamine, prostaglandins, substance P (sP) and various ions (H+ or K+). Substance P, synthesised by cells of the spinal ganglia, has also been identified at the peripheral terminal of C fibres.
Pain in the skin due to stimulation of the myelinated A fibres results in sharp, pricking pain and stimulation of the unmyelinated C fibres results in stinging, burning pain.
Deep pain is caused by injury of visceral organs and deep muscle and skeletal structures. It is characteristically diffuse, aching and poorly localised. However, pain within deep structures may also be referred to the skin.
Specific cutaneous neuropathic syndromes include:
Postherpetic neuralgia is a radiculopathy arising from Herpes zoster (shingles). This double-stranded DNA virus establishes latent infection in dorsal root ganglion after primary chickenpox. Viral reactivation in about 15% of adults (most often over 60 years) results in dermatomal mucocutaneous blistering, neuralgia and sometimes, transverse myelitis. Neuralgia may begin before, during or after the rash appears and persist for months after resolution of the rash. It is characterised by aching, burning, dysaesthesias and allodynia (severe pain from light touch) in the same segment as the rash. It is most likely in older patients. Recovery may be partial or complete (90% within six months). Treatment is with topical anaesthetics and analgesics and oral analgesics, tricyclic antidepressants, gabapentin and anticonvulsants. Transcutaneous stimulation and physiotherapy may also be helpful. In some cases systemic steroids have a role. Identification and prompt treatment of early herpes zoster with oral antiviral agents prevents postherpetic neuralgia or reduces its severity.
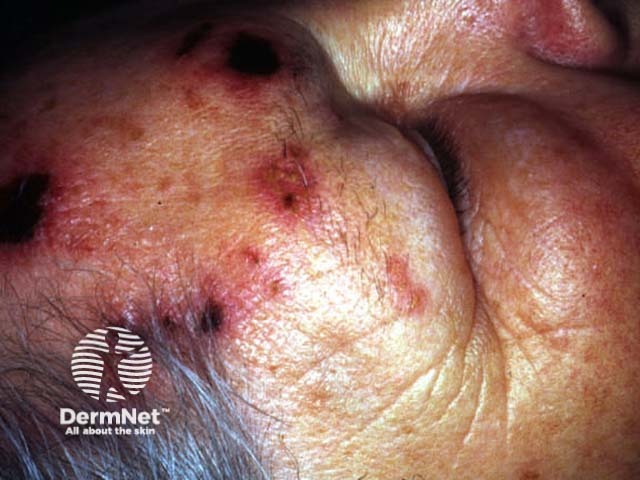
Herpes zoster ophthalmicus
Trigeminal Neuralgia (tic douloureux) results in frequent sharp facial pain, most often in the region of the second division of the trigeminal nerve. The pain is sometimes mistaken for disease of the teeth, gums and sinuses. The cause is unknown.
Pudendal neuralgia affects the perineum (mons pubis, vulva or scrotum, anal area or medial thighs) and is typically more severe when sitting. It may be unilateral or bilateral and result in burning discomfort, sharp stabbing pain, hyperalgesia or dysaesthesia. It is one cause of vulvodynia (burning pain affecting the vulva) or scrotodynia (affecting the scrotum). Vulvodynia may also present as localised tenderness in the introitus (vulvar vestibulitis) or as more generalised dysaesthetic vulvodynia associated with inflammatory processes.
Glossodynia or burning mouth syndrome presents as unexplained, prolonged pain and/or burning inside the oral cavity. It is often accompanied by dryness, paraesthesia, and changes in the sensations of taste and smell, and occurs more frequently in middle-aged women. It appears in some to be related to menopause, salivary disturbances, candidiasis, or diabetes.
Describe how to objectively assess the severity of a patient's itch or pain.
Information for patients
See the DermNet bookstore