Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2009.
Herpes zoster, or shingles, is a painful blistering rash caused by reactivation of the herpes varicella-zoster virus. The primary infection presents as chickenpox (varicella), usually during childhood. Like herpes simplex, the virus persists in selected cells of dorsal root ganglion before it is reactivated.
Herpes zoster can occur in childhood but is much more common in adults, especially the elderly, sick or immune suppressed. It is infectious, resulting in chickenpox in those who have never developed primary immunity, both from virus in the lesions and in some instances the nose and throat.
The first sign of herpes zoster is usually pain, which may be severe, in the areas of one or more sensory nerves, often where they emerge from the spine. The patient usually feels quite unwell with fever, headache and regional lymphadenopathy. Within one to three days of the onset of pain, crops of closely grouped erythematous papules develop within the unilateral dermatome(s). New papules continue to appear for several days, each blistering or becoming pustular then crusting over.
Herpes zoster Herpes zoster Herpes zoster Herpes zoster Herpes zoster Herpes zoster 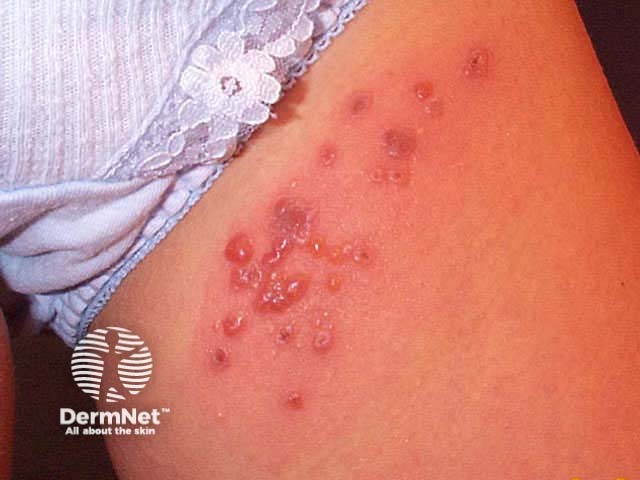
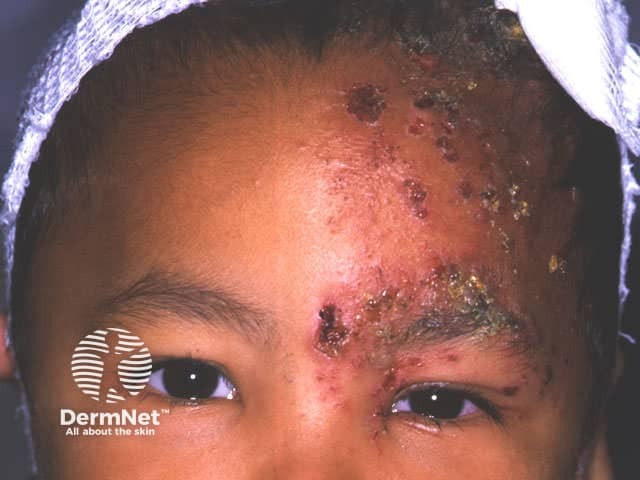
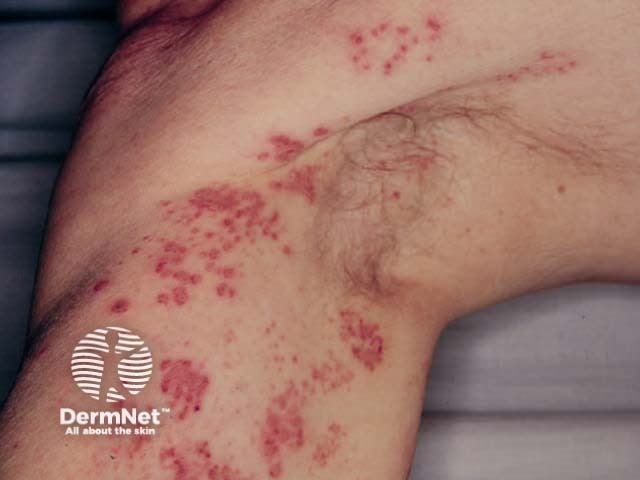
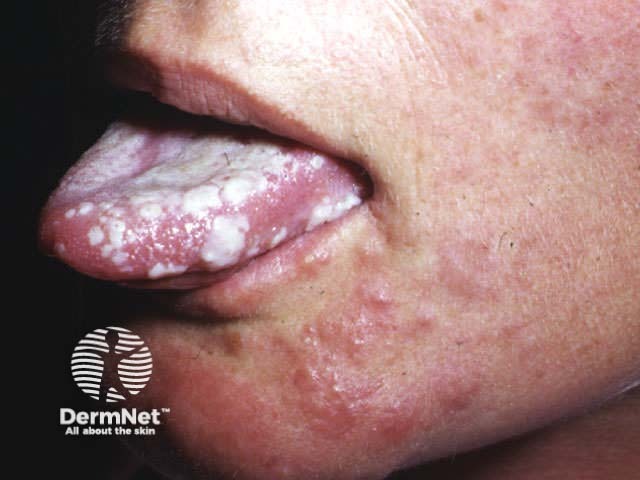
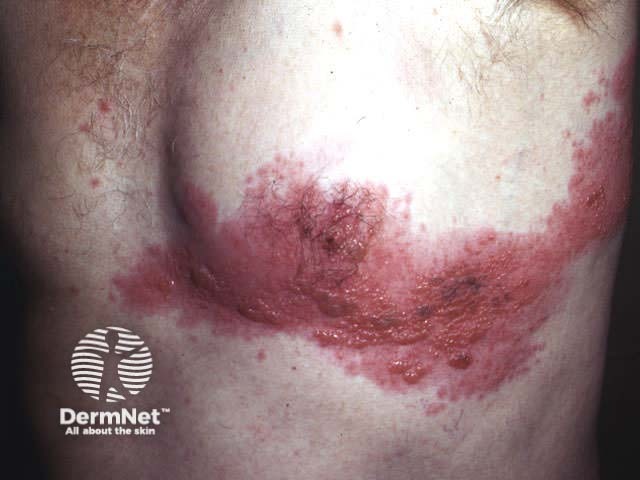
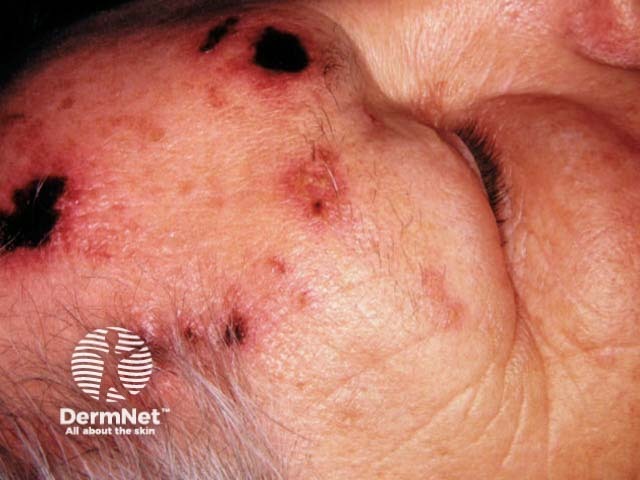
The pain and general symptoms subside gradually as the eruption disappears. In uncomplicated cases recovery is complete in 2–3 weeks in children and young adults, and 3–4 weeks in older patients.
The thoracic, cervical, ophthalmic and lumbar/sacral sensory nerve supply regions are most commonly affected at all ages but the frequency of ophthalmic zoster increases with age. Rarely the eruption may affect both sides of the body.
In elderly and undernourished patients the blisters are deeper. Healing may take many weeks and be followed by scarring. Muscle weakness arises in about one in twenty patients because the motor nerves are affected as well as the sensory nerves. Facial nerve palsy is the most common result. There is a 50% chance of complete recovery and in time some improvement can be expected in nearly all cases.
Post-herpetic neuralgia is defined as persistence or recurrence of pain more than a month after the onset of shingles. It becomes increasingly common with age, affecting about a third of patients over 40. It is particularly likely if there is facial infection. The pain may be continuous and burning with increased sensitivity in the affected areas, or a spasmodic shooting type, or, rarely, itching and crawling (formication). The overlying skin is numb or exquisitely sensitive to touch (hyperaesthesia and allodynia).
The incidence and severity of herpes zoster can be reduced by vaccination.
In most cases no investigations are necessary as the clinical features are diagnostic. However, at times the diagnosis should be confirmed in one of the following ways:
Treatment of active herpes zoster may include:
Post-herpetic neuralgia may be difficult to treat successfully. If paracetamol and soothing local applications are unhelpful, the following may be used:
The chosen drug should be stopped if it does not produce the desired effect or causes unacceptable side effects at appropriate dose and duration. Polypharmacy can be useful to allow lower doses to achieve analgesia but side effects and drug interactions can be risky.
Tramadol may be quite useful for neuropathic pain as it has serotonergic effects. More potent opioids are sometimes required short term, but can result in escalating dose requirements. If one opiate is ineffective, others are also likely to be ineffective.
Capsaicin reversibly depletes the nerve endings of the neurotransmitter substance P. Compliance is quite poor because it results in a burning discomfort when first applied. It may be required 4 times daily for up to 4 weeks before achieving adequate analgesia. The addition of glyceryl trinitrate seems to reduce the burning discomfort.
These are membrane stabilisers. Lignocaine/prilocaine cream or patches (EMLA) may be useful for localised neuralgia, and should be applied three times daily.
Amitriptyline, imipramine, dothiepin, clomipramine, desipramine and doxepin have been shown to have analgesic effects in patients with neuropathic pain, independent of their antidepressant action. They have an effect on the inhibitory serotonergic pathway, noradrenergic pathway, sodium channels, NMDA receptors and adenosine receptors. They appear to have both central and peripheral effects. As there are differing adverse effects, it is sometimes worth trying several different agents.
Amitriptyline 25 to 150 mg daily is the best studied of this group. It is helpful for neuropathic pain but is not well tolerated. Anticholinergic effects include dry mouth, blurred vision, constipation, urinary hesitancy, tachycardia and ejaculatory difficulty. Histaminergic adverse effects include sedation and weight gain. Alpha blocker action results in orthostatic hypotension. There is significant risk of mortality in overdose.
Tricyclics may also have analgesic effect when used topically, but no topical formulation is available in New Zealand.
Although SSRIs have some analgesic properties and are safer, they appear to be less effective than the tricyclics.
These have widely differing methods of action so it is logical to try other agents if the first is unsuccessful.
Discuss the role of vaccination in the prevention of herpes zoster.
Information for patients