Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Ant bites and stings — extra information
Ant bites and stings
Author: Dr Made Ananda Krisna, General practitioner Cipto Mangunkusumo Hospital, Faculty of Medicine Universitas, Indonesia. Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, December 2015. Revised September 2020.
Introduction
Demographics
More information
Clinical features
Allergic reactions
Diagnosis
Treatment
Outcome
What is an ant bite?
An ant bite occurs when an ant bites using their mandibles and mouth to pinch human skin. A bite differs from a sting: only female ants have a stinger, the caudal-most part of their bodies. Fire ants grasp the skin (bite) then inject venom with their stinger (which is immediately painful). Yet other species of ants neither bite nor sting, but instead spray formic acid.
Who gets an ant bite?
Anyone in contact with ants is at risk of ant bites or stings, particularly if they are in an area where ants build their nests. Ants form nests comprising several mounds of varied height and diameter, sometimes reaching more than 0.5 metre and several centimetres high.
Ants tend to be more numerous in areas with:
- Compact soil
- Bare ground
- Little ground cover
- Few large trees.
Large local reactions and systemic reactions are IgE-mediated, seen in individuals already sensitised to ant venom.
More about ants
Ants belong to Hymenoptera insect order, under the family of Formicidae. The order of Hymenoptera includes bees and wasps.
There are more than 12,000 species of ants. Although they can nearly all bite or sting, few cause significant local and/or systemic reaction in humans. Most ants are too small to effectively bite humans, and their sting is mild. However, the sting from harvester ants and fire ants can cause unpleasant symptoms and may lead to allergic reactions.
Pachycondyla chinensis is an invasive ant species that has spread to New Zealand from Far East Asia, and the sting can cause anaphylaxis. Myrmecia pilosula, commonly known as the jack jumper ant, is native to Australia, and is the most common cause of Hymenoptera-induced fatal anaphylaxis in Tasmania.
What are the clinical features of ant bites and stings?
The typical reaction to many ant bites/stings is a localised urticaria, A fire ant bite or sting causes immediate pain and a red spot, followed a few hours later by a tender, itchy pustule that can last several days to weeks. It is common for bites to be clustered especially under clothing.
Typical skin reaction to ant bites/stings
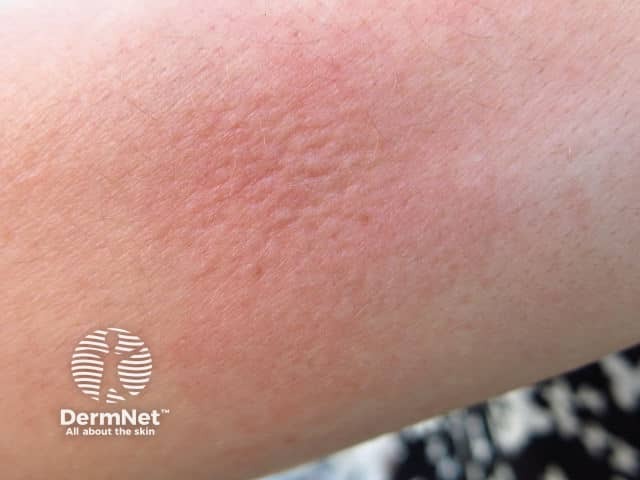
Localised urticarial reaction to ants
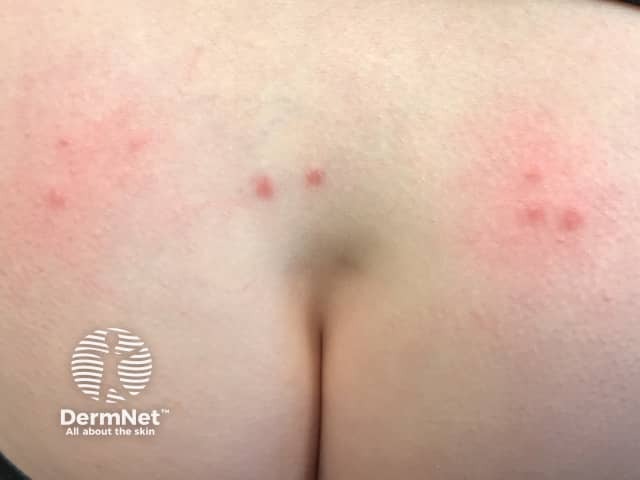
Ant bites
Allergic reactions to ant bites and stings
Generally, allergic reactions to Hymenoptera bites are milder than to stings. Allergic reactions to Hymenoptera are classified into 4 categories:
Local reaction
Local reaction is the most common presentation following an ant bite/sting. It consists of localised pain, itch, redness, swelling, and induration. The swelling is usually less than 5 cm in diameter, and is sometimes urticarial (wealing). A local reaction lasts for less than 24 hours.
Large local reaction
A large local reaction of pain, erythema, blisters, swelling, and itch is defined as involving a large area of skin greater than 10 cm around the bite/sting site persisting for at least 24 hours. In many cases, the severity peaks after 1 to 2 days, and takes 7 to 10 days to resolve.
Mild systemic reaction
A mild systemic reaction involving the skin and/or gastrointestinal system develops in less than 1% of ant bites/stings. Skin manifestations include flushing, itch, angioedema, urticaria, and redness in areas distant from the bite/sting and/or a generalised distribution. Gastrointestinal system symptoms may consist of mild nausea, diarrhoea, and/or abdominal cramping. Dizziness, shortness of breath, and nausea occur in moderately severe reactions.
Severe systemic reaction
A severe systemic response to ant venom is marked by clinical manifestations in 2 organ systems distant from the bite/sting, such as angioedema (especially of larynx), flushing, hoarseness, wheezing/bronchospasm, chest pain, hypotension, dizziness, severe abdominal pain, profuse vomiting, or uterine cramping. Anaphylactic shock and loss of consciousness, respiratory and cardiac arrest can occur.
How are ant bites/stings diagnosed?
The diagnosis of ant bites/stings is based on clinical findings and relevant exposure, or possible exposure, to ants. Referral for allergy testing is warranted only in cases presenting with severe systemic reaction. For a large local reaction, skin testing is not required because the risk of anaphylaxis after a subsequent ant bite/sting is extremely low.
What is the treatment for ant bites/stings?
Treatment for ant bites/stings depends on the type of reaction. First remove the ants from your skin and wash the affected area. Apply a cool compress to sooth the itching and reduce swelling.
Treatment for local and large local reaction
Immediate management may include:
- Oral antihistamines for itch and urticaria
- Analgesics such as paracetamol (American terminology acetaminophen) if painful
- Short-course of oral corticosteroids for large local reaction if inflammation is slow to resolve
- Education for insect avoidance: remove visible ant nests, avoid walking barefoot, wear trousers and long-sleeve shirt when engaged in outdoor activities.
Long-term management:
- Education for insect avoidance in areas where venomous ants are prevalent
- Wear shoes and socks when outdoors
- Wear work gloves when gardening.
Treatment for mild and severe systemic reaction
Immediate management may include:
- Adrenaline (American terminology epinephrine) injection
- Basic life support for anaphylaxis
- Immediate referral to emergency room
- Antihistamine injection as an adjunct.
Long term management:
- Adrenaline self-injection pen for patients with severe systemic reactions and education on how/when to use it
- Allergy specialist referral for skin testing and venom immunotherapy
- A generalised urticarial reaction in children < 16 years of age does not need immunotherapy
What is the outcome for ant bites/stings?
- The risk of a severe systemic allergic reaction following an ant/insect bite is greater in adults (especially > 45 years old) than in children. Approximately 85% of adults having systemic allergic response are categorised as severe reaction, while it is only 40% of children.
- Less than 1% of ant bites result in more severe reaction after a re-bite.
References
- Zirngibl G, Burrows HL. Hymenoptera stings. Pediatr Rev. 2012;33(11):534-5. doi:10.1542/pir.33-11-534. PubMed
- Holbrook T. Ant Anatomy Arizona: Arizona State University; [cited 2015 Dec 19]. Available from: https://askabiologist.asu.edu/explore/ant-anatomy.
- Graham JH, Hughie HH, Jones S, et al. Habitat disturbance and the diversity and abundance of ants (Formicidae) in the Southeastern Fall-Line Sandhills. J Insect Sci. 2004;4:30. doi:10.1093/jis/4.1.30. PubMed
- Agriculture and Natural Resources UoC. An introduction to ants California: University of California; 2014 [cited 2015 Dec 19]. Available from: http://www.ipm.ucdavis.edu/TOOLS/ANTKEY/antid1.html.
- Tripolt P, Arzt-Gradwohl L, Čerpes U, Laipold K, Binder B, Sturm GJ. Large local reactions and systemic reactions to insect stings: Similarities and differences. PLoS One. 2020;15(4):e0231747. doi:10.1371/journal.pone.0231747. PubMed
- Potiwat R, Sitcharungsi R. Ant allergens and hypersensitivity reactions in response to ant stings. Asian Pac J Allergy Immunol. 2015;33(4):267–75. PubMed
- Shek LP, Ngiam NS, Lee BW. Ant allergy in Asia and Australia. Curr Opin Allergy Clin Immunol. 2004;4(4):325–8. doi:10.1097/01.all.0000136761.51195.01. PubMed
- Brown SG, Franks RW, Baldo BA, Heddle RJ. Prevalence, severity, and natural history of jack jumper ant venom allergy in Tasmania. J Allergy Clin Immunol. 2003;111(1):187-92. doi:10.1067/mai.2003.48. PubMed
- Lee EK, Jeong KY, Lyu DP, et al. Characterization of the major allergens of Pachycondyla chinensis in ant sting anaphylaxis patients. Clin Exp Allergy. 2009;39(4):602–7. doi:10.1111/j.1365-2222.2008.03181.x. PubMed
On DermNet
Other websites
- Blistering disorders — DermNet e-lecture [Youtube]
