Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Adam Dedat, Trainee General Practitioner; Dr Sidra Khan, Specialist Dermatology Registrar; Dr Ian Coulson, Consultant Dermatologist, United Kingdom (2022)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Causes
Resistant fungi
Prevalence
Clinical features
Diagnosis
Management
The acquired resistance of dermatophyte fungi to antifungal medication (both topical and oral) was previously thought to be exceptionally rare. However resistance, globally, is on the rise.
An epidemic-like spread of recalcitrant and terbinafine-resistant dermatophytosis has been reported across the Indian subcontinent since 2015. In recent years, 85% of European countries have also reported clinical and/or mycological confirmation of terbinafine-resistant dermatophytosis. Although best recognised with terbinafine, resistance to griseofulvin and triazole (azole) antifungal agents is becoming more prevalent.
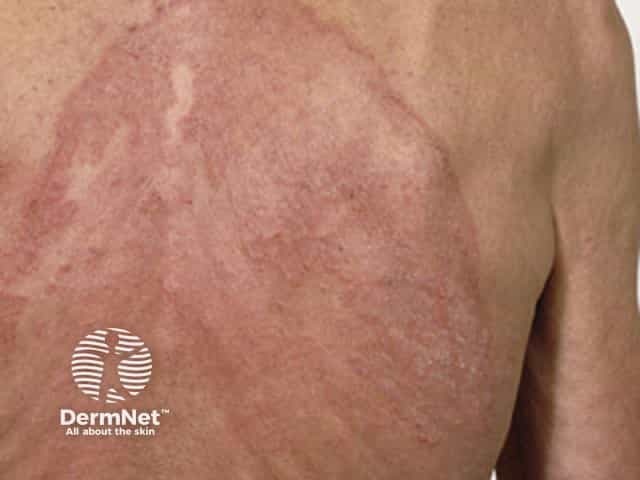
Extensive tinea corporis that has spread despite oral terbinafine should alert to antifungal resistance
As with anti-bacterial drug resistance, the molecular mechanisms can be either intrinsic or acquired resistance.
Terbinafine appears to be the antifungal agent with the most resistance, with mutations of the squalene epoxidase gene producing loss of function of squalene epoxidase, the enzyme that is critical in the mode of action of allylamine antifungals. Cross-resistance to other allylamines (butenafine, naftifine) has been reported.
Triazole drugs (eg, fluconazole, itraconazole, voriconazole) is increasingly reported and is thought to result from the overexpression of ABC transporters that transport drugs extracellularly. Some species of dermatophyte have alarmingly demonstrated resistance to both allylamine and triazole drugs.
Griseofulvin prevents fungal growth by inhibiting microtubule formation within the fungus. Resistance to griseofulvin has been rarely noted since the 1960s.
There is a belief that the widespread availability and use of fixed-dose combinations of potent topical steroids, antibiotics, and antifungal agents has resulted in the selection of resistant dermatophytes.
Terbinafine resistance has been identified in the following species:
There has been controversy regarding the precise taxonomy of the resistant dermatophyte species, with some arguing that a separate species of Trichophyton indotineae is predominant, with others asserting that this is a new variant of the Trichophyton mentagrophytes/interdigitale complex.
This is unknown because sensitivity testing is not routinely performed, but a large research study from centres around India found 71% of T. interdigitale cultures to be terbinafine-resistant.
They observed triazole resistance was more frequent in terbinafine-sensitive strains than in resistant ones.
It is becoming more common and recognised in non-endemic areas in Europe and the USA.
In endemic areas of the Indian subcontinent, resistant fungi cause:
In non-endemic areas, the clinical features may be similar but there is often a history of travel to, or close contact with, an individual who has resided in an endemic area.
Diagnosis is based on clinical suspicion and laboratory testing.
Clinical suspicion:
Culture and sensitivity testing (antifungal sensitivity testing):
Hot-spot gene mutation testing:
Management is yet to be clarified. Sensitivity testing is becoming standardised, more widely available in some countries, and should guide onward therapy choice.
For terbinafine resistance, itraconazole seems to be the favoured agent, and long courses at higher than standard doses have been advocated.