Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. December 2016.
Introduction
Demographics
Causes
Clinical signs
Diagnosis
Treatment
Outlook
Autoimmune polyglandular syndrome type 2 (APS2) is the most common of the immunoendocrinopathy syndromes.
APS2 is also known as Schmidt syndrome.
APS2 is inherited in an autosomal dominant pattern; that is, an abnormal gene from one parent can cause disease and this happens even when the matching gene from the other parent is normal. A parent with an autosomal dominant condition has a 50% chance of having a child with the condition.
Researchers theorise that APS2 develops when a person with genetic susceptibilities is exposed to an autoimmune trigger. Initially, autoimmune activity is asymptomatic. Progressive organ damage and inflammatory infiltration occur over time.
The clinical signs of APS2 include the signs of Addison disease, autoimmune thyroid disease and/or diabetes mellitus type 1 and most commonly appear in people aged 20–30 years.
The signs and symptoms of APS2 vary depending on the specific clinical manifestations seen in an individual; they may include:
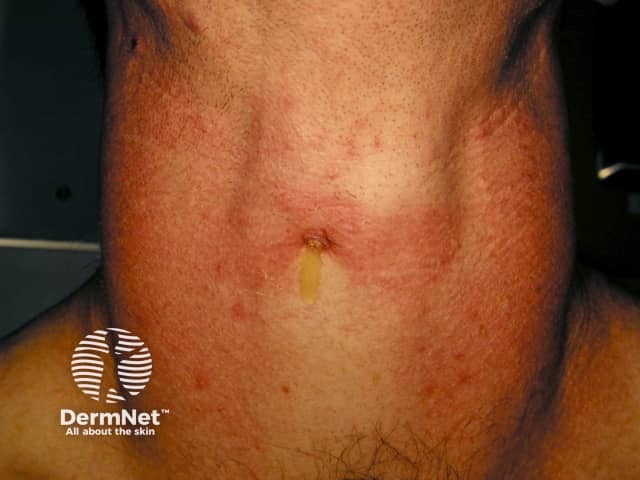
Thyroid goitre
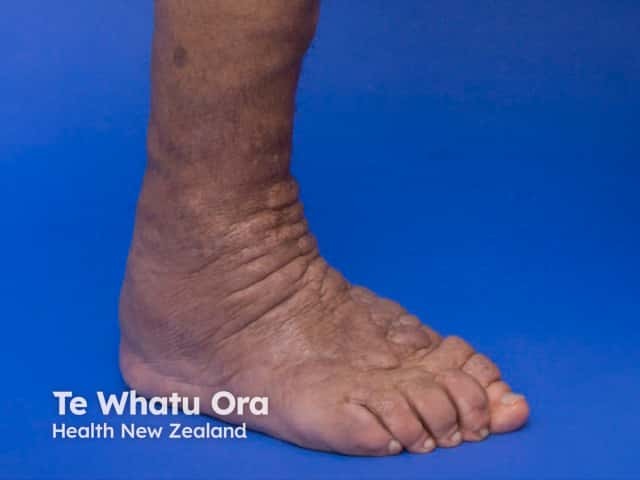
Pretibial myxoedema in Graves disease
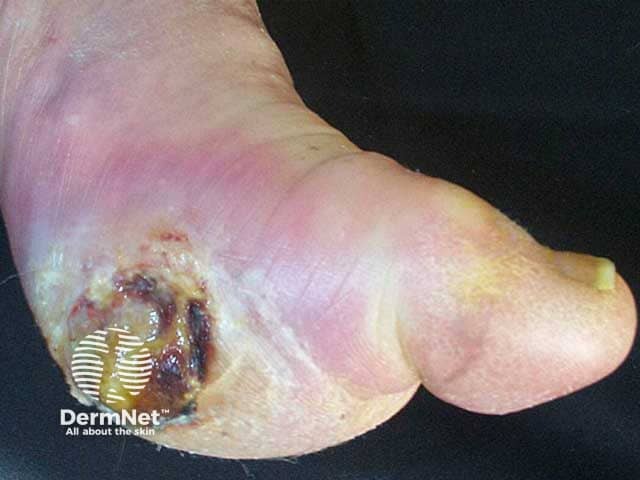
Ulcer due to diabetic neuropathy
APS2 is diagnosed in an individual who has multiple autoimmune diseases. Tests used to diagnose APS2 may include:
Other tests may include gonadotropin levels, thyroid tests (thyroid-stimulating hormone [TSH], triiodothyronine [T3] and thyroxine [T4]), plasma renin activity, serum electrolytes, fasting blood glucose and a complete blood count.
The treatment for APS2 depends upon which organs are affected, and may include:
The outlook for APS2 is variable and depends upon which specific organs or glands become affected by the syndrome.