Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2008. Updated by Thomas Stewart. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. April 2018.
Introduction
Origin
How it spreads
Clinical features
Cutaneous manifestations
Diagnosis
Treatment
Prevention
Outcome
Chikungunya is an arthropod-borne alphavirus transmitted by mosquitos. It causes an acute febrile illness accompanied by a rash, joint pain, and muscle pain.
Chikungunya virus (CHIK V) was first reported in Tanzania in 1952. Following the initial outbreaks in Africa and after more than three decades of quiescence, it made a resurgence and is currently endemic in several regions in Africa, India, South-East Asia, and the Western Pacific. Outbreaks have also become more frequent in the Indian Ocean and Pacific Island nations [1,2]. There have been no locally acquired cases in New Zealand or Australia; however, travellers can transport the virus after visiting endemic areas [3,4].
Chikungunya virus is transmitted to humans through the bite of an infected mosquito, mainly Aedes aegypti or A. albopictus. Mosquitos that are capable of spreading chikungunya virus exist in some parts of Australia but are not normally found in New Zealand [3,4].
Rarely, chikungunya spreads via the maternal-fetal route, through blood products, or organ transplantation [5].
Chikungunya virus typically has an incubation period of 3–7 days (range 1–12 days) [6,7].
The first clinical manifestations are sudden-onset high fever and chills followed by severe polyarthralgia.
A wide range of mucocutaneous manifestations occurs, affecting up to 75% of patients with chikungunya during the disease course [6,7].
These have mainly been reported during chikungunya outbreaks in India.
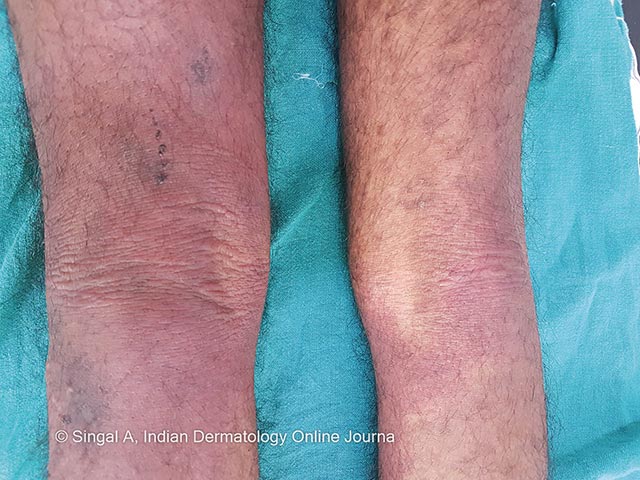
A morbilliform eruption arising with 3 days of fever in Chikungunya
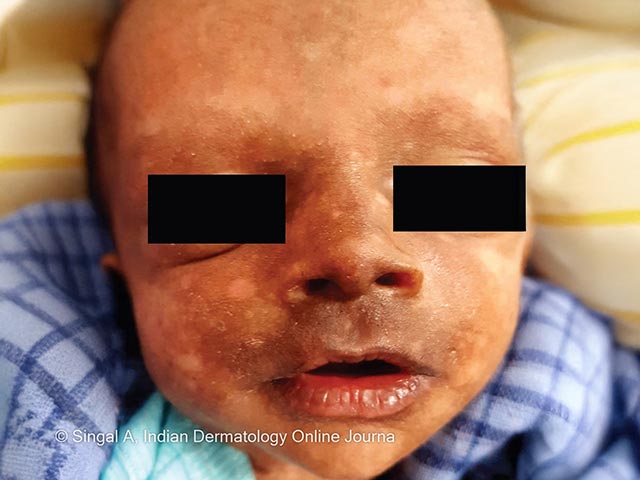
Facial hyperpigmentation around the nose and mouth in Chikungunya
Other cutaneous features of chikungunya may include:
Chikungunya fever should be suspected in a patient with acute-onset fever and polyarthralgia when living in an endemic area or following recent travel to an area where mosquito-borne transmission of chikungunya virus has been reported.
Chikungunya fever is usually self-limiting and no specific therapy is required or available.
No vaccine against chikungunya virus is currently available. Prevention relies primarily on avoidance of mosquitos (long-sleeved clothing, DEET insect repellents, insect screens and bed netting) [16].
The cutaneous manifestations of chikungunya typically resolve spontaneously within several weeks, without any need for specific dermatological treatment [8,9].
Patients with persistent arthralgia should be referred to a rheumatologist for additional workup and treatment [14].