Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. December 2016.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outlook
Cornelia de Lange syndrome is a rare, genetic disorder that affects virtually every bodily system and leads to an array of physical and cognitive deficits. Most children with this syndrome are diagnosed at birth.
It has a number of other names, including de Lange syndrome, Amsterdam syndrome, Brauchman–de Lange syndrome, Amsterdam dwarf, degenerative amstelodamensis typus, and Bruck–de Lange syndrome. It was first described by Cornelia de Lange in 1933, although Brauchman wrote up a similar case in 1915.
Cornelia de Lange syndrome is rare.
Cornelia de Lange syndrome is a genetic disorder.
Cornelia de Lange syndrome has complex manifestations, which can range from mild to severe. These manifestations include:
Skin disorders found in Cornelia de Lange syndrome include:
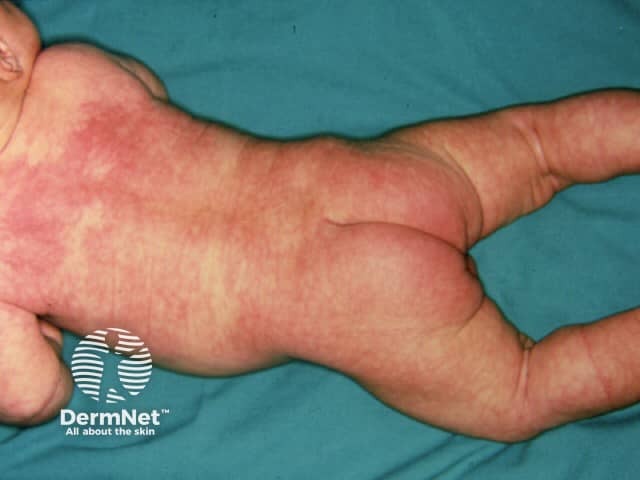
Cutis marmorata
The diagnosis of Cornelia de Lange syndrome is based on clinical findings of its characteristic signs and symptoms as evaluated by a physician. Genetic studies may be performed by specialist laboratories.
Treatment for Cornelia de Lange syndrome is lifelong and can be complex, with differences depending on each specific case. Treatment can include:
Patients with Cornelia de Lange syndrome may survive into adulthood with the right care and treatment. However, they are vulnerable to a number of serious conditions.
In one review of 295 cases of this syndrome, causes of death, in order of frequency, included: