Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2002. Updated by Dr Thomas Stewart, General Practitioner, Sydney, Australia, November 2017.
Introduction
Demographics
Causes
Differential diagnoses
Diagnosis
Treatment
Cradle cap, or pityriasis capitis, is infantile seborrhoeic dermatitis affecting the scalp.
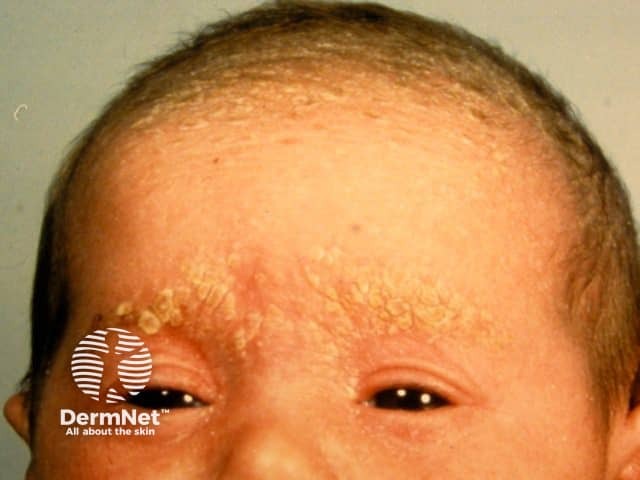
Cradle cap
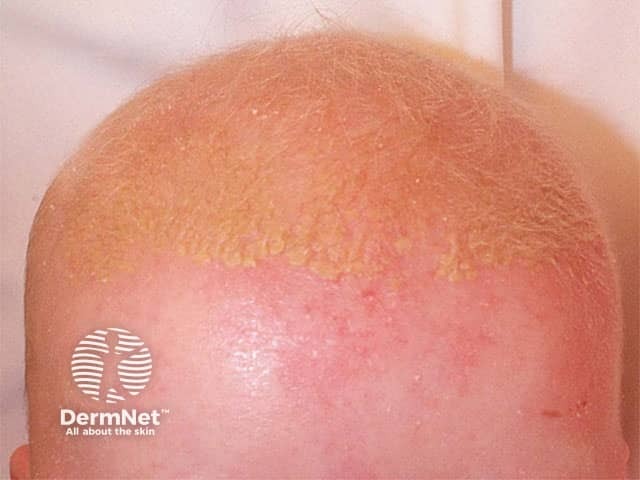
Seborrhoeic dermatitis
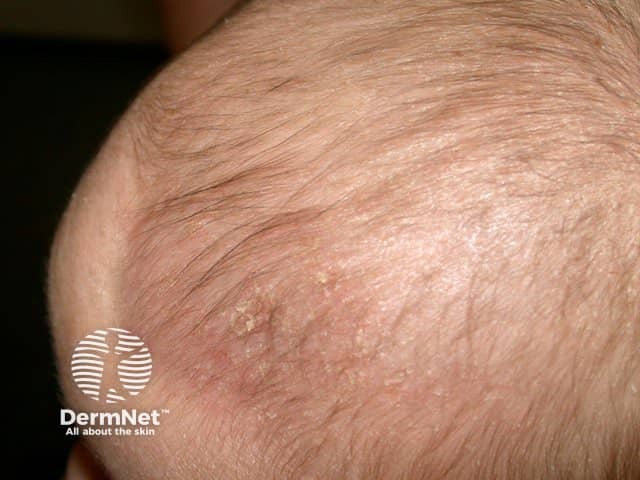
Cradle cap
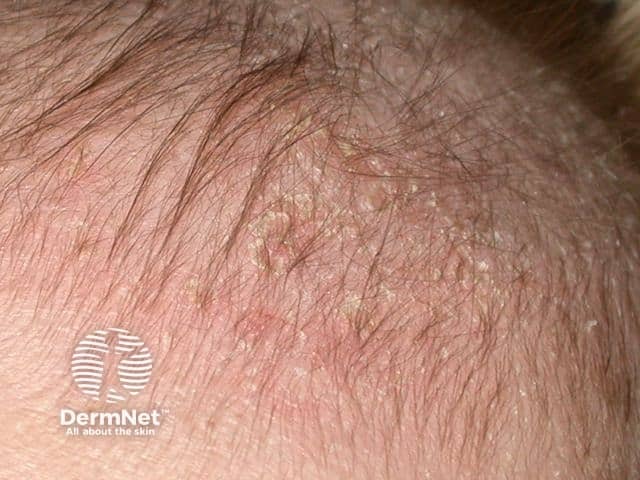
Cradle cap
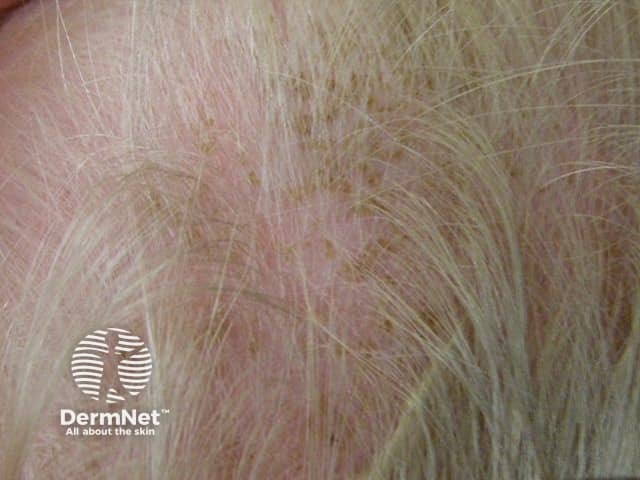
Cradle cap
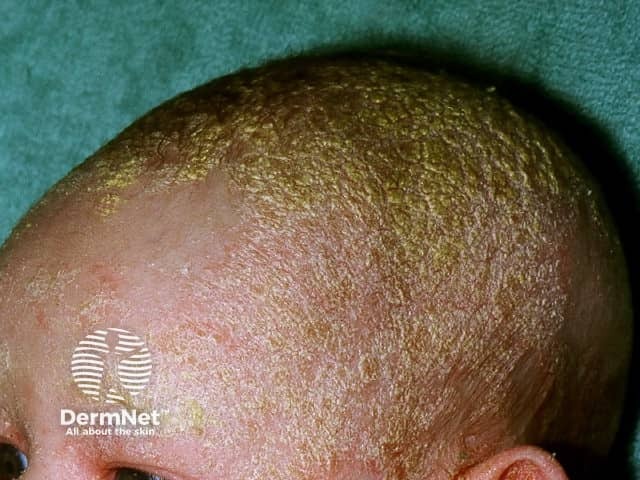
Cradle cap
Cradle cap is extremely common with an estimated prevalence of 9.5–10%. It is seen most commonly in infants aged between 3 weeks and 12 months with peak prevalence at 3 months of age [1]. There is no sex or racial predilection.
The cause of cradle cap is not known. It may be related to hyperactivity of sebaceous glands responsive to residual circulating maternal androgens. Malassezia has also been implicated although its exact role is not clear.[2,3]
Classically, there is a non-inflammatory eruption of greasy yellow scales on the scalp. The vertex and frontal areas are most commonly affected. Cradle cap is usually not pruritic and infants are otherwise generally well.
Other scalp conditions that may resemble cradle cap are:
Diagnosis is usually made clinically based on recognition of typical lesions on the scalp of an infant.
The initial approach, especially in mild and localised disease, should be conservative, involving either application of gentle emollient or repeated shampooing, followed by careful removal of scales using a soft toothbrush or comb.
More extensive or resistant disease may be treated with a low-potency topical steroid (eg, hydrocortisone 1%) or azole (eg ketoconazole 2%) for 1–2 weeks. Topical steroid may be preferred if there is a significant inflammatory component.[4,5]
Cradle cap is benign and self-limiting. It usually resolves without intervention over the course of weeks to several months. If disease persists beyond 12 months, the diagnosis should be reconsidered.