Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. December 2016.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outlook
Crouzon syndrome is characterised by a variety of craniofacial and developmental symptoms.
It is a hereditary condition inherited in an autosomal dominant pattern (an abnormal gene from one parent can cause the syndrome). It is also known as Crouzon disease, craniofacial dysostosis, craniostenosis, Apert–Crouzon syndrome, acrocephalosyndactyly type II, Vogt cephalosyndactyly, and trigorhinophalangeal dysplasia.
It was first described by Crouzon in 1912.
Crouzon syndrome is rare, although it is still the most common craniosynostosis syndrome (where the fibrous joints of the skull prematurely close during infancy).
Crouzon syndrome is usually caused by mutations in the fibroblast growth factor receptor 2 (FGFR2) gene. The FGFR3 gene can also be involved.
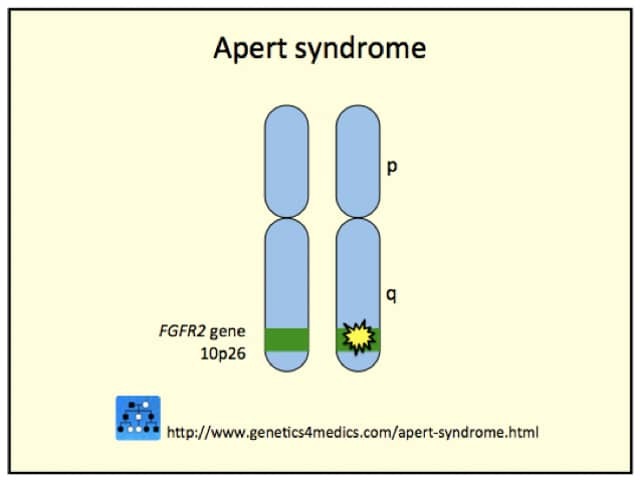
Crouzon syndrome genetics*
*Image courtesy Genetics 4 Medics
The clinical features of Crouzon syndrome vary widely, and range from mild to severe. The key feature is the premature closure of the skullcap and cranial base sutures, and craniosynostosis.
Related distinctive facial features include:
Visual defects associated with Crouzon syndrome include:
These visual defects are due to corneal injury, cataracts (a clouding of the lens of the eye or its surrounding transparent membrane), optic atrophy (deterioration of the optic nerve) and iris coloboma (a hole in the iris).
Other features associated with Crouzon syndrome include:
The main dermatological sign of Crouzon syndrome is acanthosis nigricans, in which there is thickened, hyperpigmented skin with a velvety feel affecting the neck, torso, and face. It usually occurs by the onset of puberty.
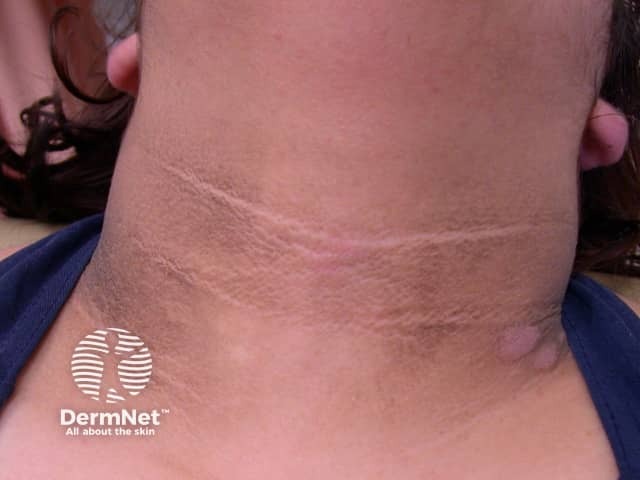
Acanthosis nigricans*
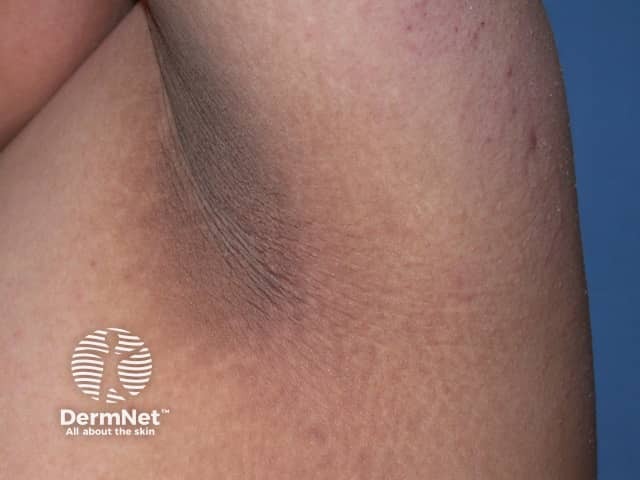
Acanthosis nigricans*
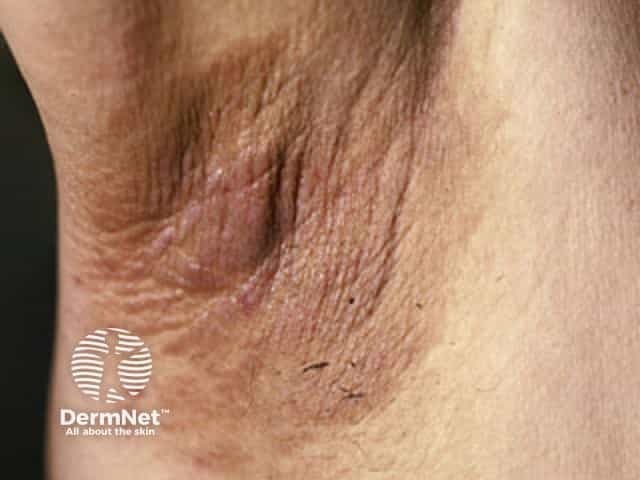
Acanthosis nigricans*
Crouzon is confidently diagnosed in a child with craniosynostosis when mutations on the FGFR2 gene are detected. The genes of the affected individual’s parents may also be tested to detect mosaicism (possessing cells of two or more genetically different types).
The standard treatment for Crouzon syndrome includes early craniectomy (the surgical removal of a portion of the skull) and cosmetic reconstruction to help promote normal facial growth.
Multidisciplinary care may involve medical and surgical assessment and management of symptoms. This can include:
Improvements in surgical techniques, specifically in craniofacial surgery, have greatly increased quality of life, intellectual and physical abilities, and social acceptance for children with Crouzon syndrome.
The lifespan for individuals with Crouzon syndrome is generally normal, but mortality can occur due to airway obstruction, acute respiratory distress, or increased intracranial pressure.