Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, November 2015. Revised November 2020
Introduction
Introduction
Causes
Clinical features
Complications
Diagnosis
Treatment
Endometriosis is the growth of endometrial tissue (tissue that lines the womb and is shed as menstrual flow) outside the uterus (womb). It usually arises close to the uterus within the pelvis — the lower part of the abdomen. The mass is also called an 'endometrioma'. Endometriosis outside the pelvis occurs in about 12% of women with endometriosis.
Cutaneous endometriosis is endometriosis in the skin and is rare. It was first described by Villar in 1860. It commonly occurs in a surgical incision from a previous gynaecological or abdominal surgery, such as caesarean section, hysterectomy or laparoscopic surgery but can also develop spontaneously. It also called 'scar endometriosis'.
The most common sites for cutaneous endometriosis are the abdominal wall, umbilicus, vulva, and the extremities.
There are two theories regarding the cause of spontaneous cutaneous endometriosis.
Women with cutaneous endometriosis can present with the following signs and symptoms.
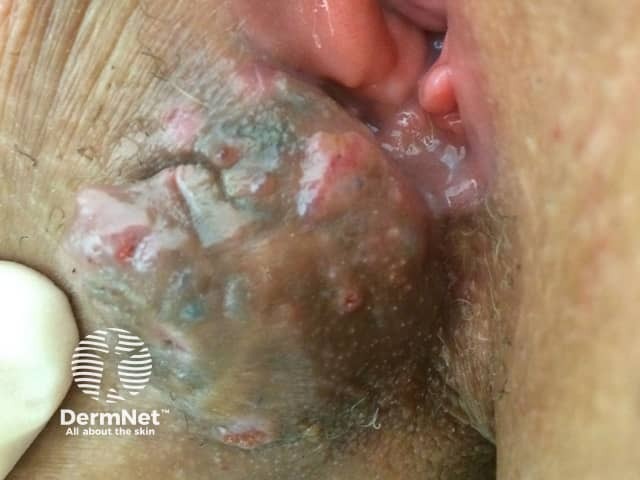
Complications from cutaneous endometriosis include:
Malignancy should be suspected if the mass is abnormally large, has grown rapidly, or has recurred after previous excisions.
Diagnosis of cutaneous endometriosis is based upon:
Cytology on fine needle aspirate or histopathology on skin biopsy or excision specimen is the key to accurate diagnosis and detects endometrial glands, stroma, and haemosiderin.
Diagnosis is often delayed due to confusion with other conditions, including haematoma, neuroma, hernia, and neoplastic tissue.
The main treatment for cutaneous endometriosis is surgical excision of the mass, preserving the umbilicus if relevant.
Medical therapy uses the hormones danazol, progesterone, and gonadotrophin releasing hormone (GnRH).