Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, October 2015.
Introduction Causes Signs and symptoms Complications Diagnosis Treatment
DiGeorge syndrome is a rare primary immunodeficiency disorder with a wide range of presenting signs and symptoms. It is due to chromosomal defects that arise early in gestation.
DiGeorge syndrome is also called velocardiofacial syndrome, shprintzer syndrome, CATCH22 and 22q11.2 deletion syndrome.
DiGeorge syndrome is caused by dysfunctional development of certain cells and tissues in utero. Approximately 90% of the patients with DiGeorge syndrome have a deletion of a segment of 30–40 genes on chromosome 22. Generally, this is considered to be the consequence of a random event in either the egg or the sperm, but more rarely it can be passed on from parent to child.
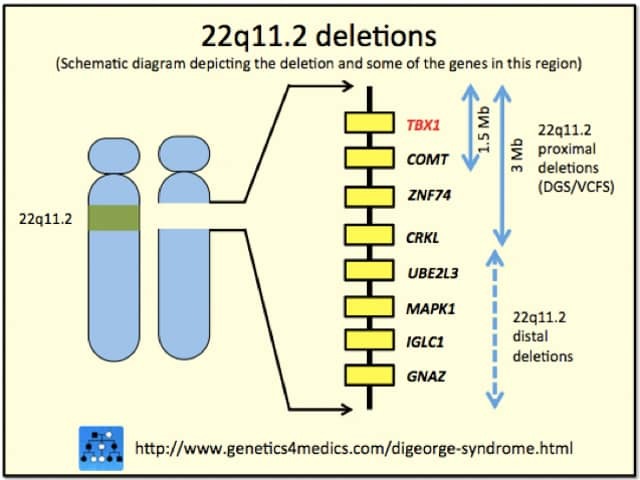
DiGeorge syndrome
*Image courtesy Genetics 4 Medics
Because there is great phenotypic variability associated with this syndrome, one patient may present with vastly different symptoms from another. Possible symptoms include:
DiGeorge syndrome patients also generally present with distinctive facial characteristics, including:
Possible complications arising from DiGeorge syndrome are varied and may include:
DiGeorge syndrome is diagnosed based on patient signs and symptoms, the presence of a heart defect (though this by itself is not diagnostic), and genetic testing, fluorescence in situ hybridisation (FISH), is used to determine deletion in chromosome 22.
There is no cure for DiGeorge syndrome. Treatment is based on correcting or managing secondary problems wherever possible. This can include: