Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2005. Updated by Dr Sara de Menezes, Basic Physician Trainee, Alfred Health, Melbourne, Australia, May 2016.
Introduction Demographics Causes Clinical features Complications Diagnosis Treatment Outcome
Erythromelalgia is characterised by intense burning pain, erythema (marked redness), and increased skin temperature, primarily of the feet and hands. It is classified into primary and secondary erythromelalgia.
Erythromelalgia is also known as erythermalgia. Primary erythromelalgia with positive family history is known as Weir-Mitchell disease.
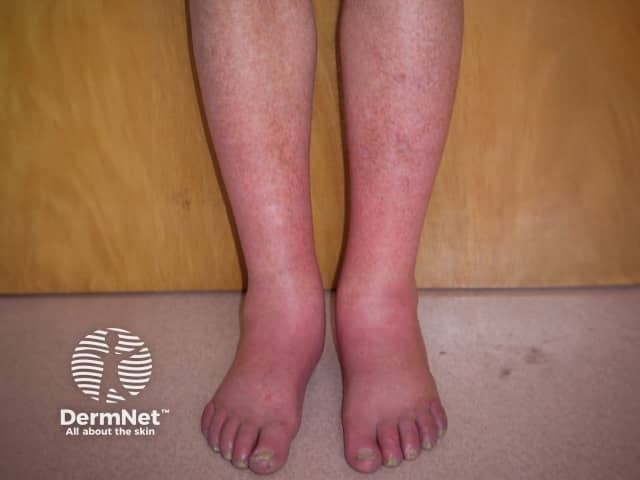
Erythromelalgia
Erythromelalgia is rare. Various studies have suggested that the combined prevalence of primary and secondary erythromelalgia is between 0.36 to 2 per 100,000 patients.
Primary erythromelalgia affects males less commonly than females (ratio 1:2.5) while the opposite is true for secondary erythromelalgia (ratio 3:2). Erythromelalgia affects a range of people of diverse backgrounds, eg, Chinese, American, European.
Primary erythromelalgia is caused by mutations in SCN9A, which encodes for the Nav1.7 type sodium channel receptor. Mutations are responsible for familial (inherited) erythromelalgia and sporadic forms of the condition. NAV1.7 is expressed in nociceptive neurons (these detect nerve-related pain) and normally amplifies the nociceptive pain signals. Mutations lead to dysregulation and ‘hyperexcitability’ of these neurons, with dilation of the small blood vessels that become congested with blood. In some individuals, symptoms are precipitated by puberty, suggesting a hormonal influence.
Secondary erythromelalgia is commonly associated with myeloproliferative disorders. In these disorders the bone marrow produces excessive numbers of cells, e.g. polycythaemia vera (increased red cells), and essential thrombocythaemia (increased platelets). Erythromelalgia presents before the appearance of the myeloproliferative disorder in 85% of cases. Occasionally it can occur in association with paraneoplastic disorders, autoimmune neuropathies and rarely diabetes, rheumatological and infectious diseases.
Primary erythromelalgia may develop at any age. Secondary erythromelalgia occurs most often in those over 40 years of age.
Lower extremities such as the soles of feet and toes are most commonly involved. Rarely does the pain extend up to include the knees. Upper extremity involvement includes the fingers and hands. Often both feet and hands are involved and both sides of the body (bilateral) are affected. It may affect one side of the body (unilateral), particularly in secondary cases. Less frequently, symptoms may also appear in the face, ears and other parts of the body.
The classic description of erythromelalgia is red, painful, warm hands or feet, brought on by warming or hanging the limb downward, and relieved with cooling and elevation.
Symptoms often become so bad that normal functioning and quality of life are greatly affected. Patients avoid warm weather and may even relocate to cooler climates. Many cannot wear socks or closed shoes even in winter. Some patients become virtually housebound by continuous flare-ups and pain.
It is possible to get ulceration, necrosis and gangrene as complications of erythromelalgia. Occasionally, wounds can become secondarily infected, which, if severe enough, may lead to amputation.
Primary erythromelalgia is a clinical diagnosis based on the presence of the triad of recurrent redness, burning pain and warmth of extremities. Family history of erythromelalgia can support a familial primary erythromelalgia versus sporadic cases. There are no specific guidelines for SCN9A genetic testing, but these can be considered in young patients in whom there is a positive family history and when secondary causes have been excluded. Genetic testing may have impact on family planning given 50% probability of heritability of the condition by offspring.
Investigation for underlying causes is essential to exclude secondary erythromelalgia. Erythromelalgia may be an early sign of polycythaemia (raised red cells) or thrombocythaemia (raised platelets), where symptoms may precede diagnosis of the myeloproliferative disorder by 2.5 years. These diseases are detected by full blood count. Further tests may be necessary.
Diagnosis is based fairly much on the clinical picture, hence is often difficult because of the intermittent nature of the disease. Provided the patient gives a good description of their symptoms, a tentative diagnosis may be made. If in doubt, a trial of immersing an affected area in hot water for 10–30 minutes may sometimes provoke an attack and support the diagnosis.
The underlying cause must be treated where possible in secondary erythromelalgia. The treatment of symptoms of both primary and secondary erythromelalgia is through general non-medical measures, drug therapy and surgical intervention.
Most cases of primary erythromelalgia are refractory to pharmacotherapy and response to pain therapeutics is variable. Most of these therapies have only been validated in case reports or smaller studies.
Patients respond quite variably and no single therapy has proved consistently effective.
In most patients with primary erythromelalgia, their symptoms remain refractory to sodium channel blockers and other treatment, and symptoms tend to progress over time. Quality of life can be greatly affected due pain and disability due to pain, secondary tissue damage (ulcers, necrosis, gangrene) or self-harming behaviours can be an issue.
Spontaneous remissions have also been known to occur.