Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Assoc Prof Patrick Emanuel, Dermatopathologist, Auckland, New Zealand, 2013.
Introduction Histology Special studies Differential diagnoses
Graft versus host disease (GVHD) usually follows bone marrow transplantation. Solid organ transplantation, blood transfusions, and maternal-fetal transfusions have also been reported to cause GVHD.
In acute GVHD, there is usually a sparse interface or lichenoid lymphocytic infiltrate which infiltrates the epidermis (figures 1a, 2a) and involves adnexal structures (figures 2a, 2b). There are hydropic changes in the basement membrane. Characteristically, the lymphocytes in the epidermis surround keratinocytes which subsequently undergo necrosis.
Attempts have been made to grade the severity of acute GVHD depending on the degree of lymphocytic infiltration and epidermal necrosis. Grade 0 = no inflammation, Grade 4 = dense infiltrate with separation of the epidermis from the dermis.
In chronic GVHD, the features usually resemble lichen planus with a denser infiltrate than seen in acute phase lesions. There is usually impressive keratinocyte necrosis associated with the infiltrate (figure 3). Later chronic GVHD resembles scleroderma or morphoea with thickened collagen bundles arranged parallel to the epidermis.
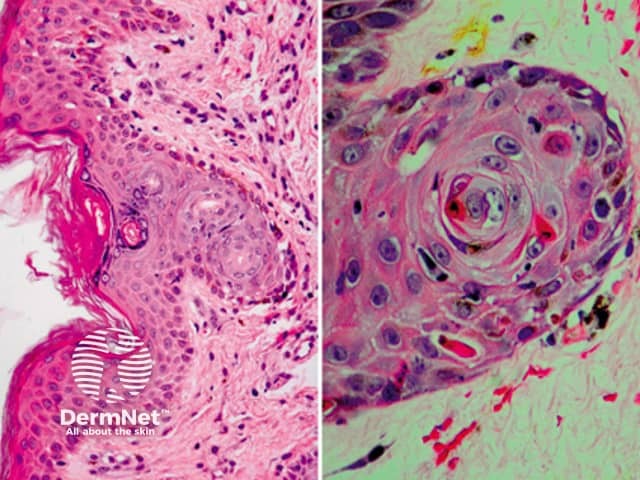
Figure 1
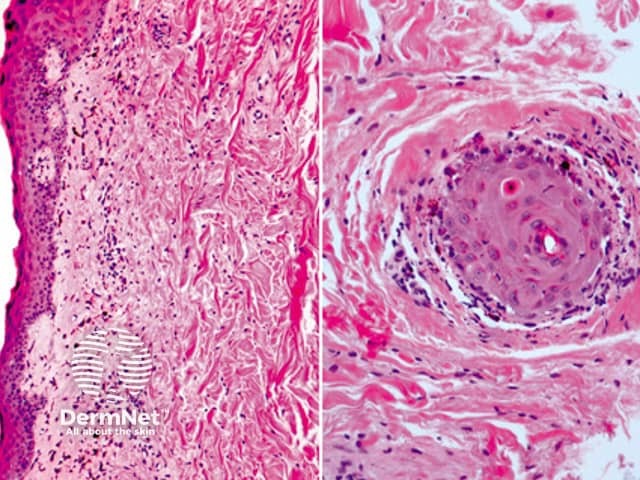
Figure 2
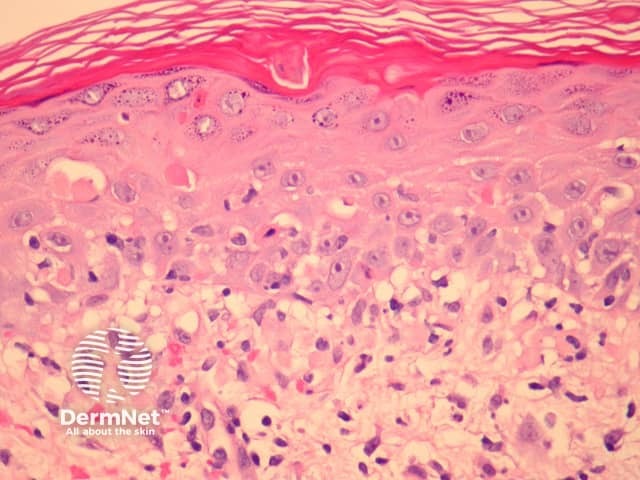
Figure 3
None are generally needed.
The clinical history is generally needed to make the diagnosis.
Drug eruption – Dermal eosinophils and a lack of adnexal involvement favour a drug eruption but distinction may be impossible in some cases.
Other lichenoid reactions – Lichen planus, paraneoplastic pemphigus, and erythema multiforme may exhibit similar features. Clinical correlation can be extremely helpful.