Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Rajan Ramji, 5th Year Medical Student, University of Auckland, New Zealand; Chief Editor: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. April 2016.
Introduction Demographics Clinical features Diagnosis Treatment
A leiomyoma is a benign tumour composed of smooth muscle. It is capable of arising wherever smooth muscle is present. One form of leiomyoma arises from uterine smooth muscle, and is otherwise known as uterine fibroids.
Cutaneous leiomyomas may be classified into three types:
Each type arises from smooth muscle in specific tissues or organs and has distinct clinical or histological features.
Uterine leiomyomas represent 95% of all reported leiomyomas. Cutaneous leiomyomas represent 75% of all extra-uterine leiomyomas.
Leiomyomas are often painful.
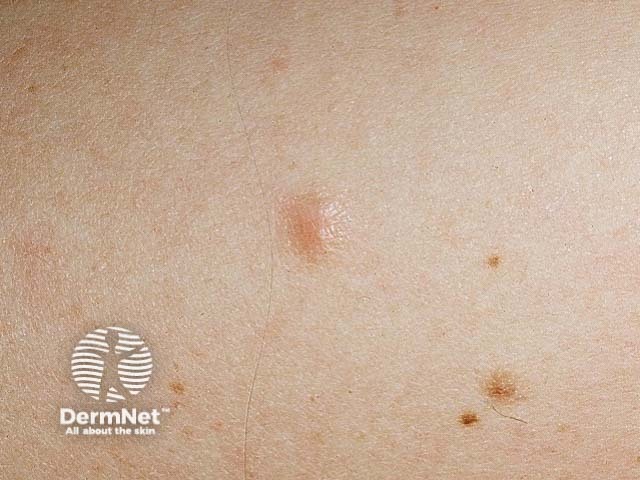
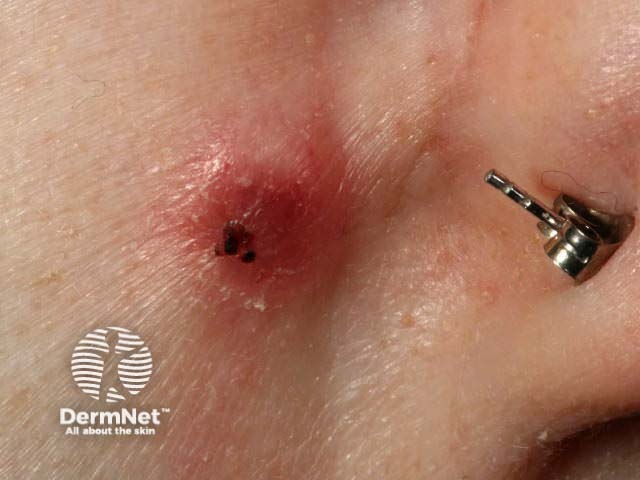
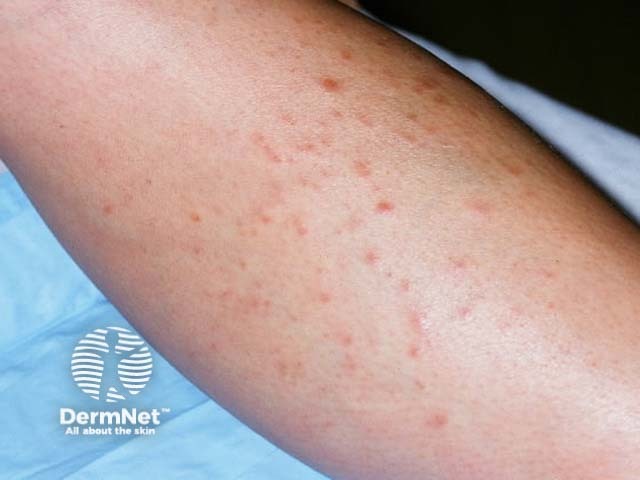
Leiomyomas
Cutaneous leiomyomas are usually diagnosed by skin biopsy. Each type of leiomyoma has unique histology.
Surgical excision is the definitive treatment for single lesions. Multiple cutaneous leiomyomas have a high rate of recurrence (~50%) within weeks to years – especially if part of HLRCC or Reed syndrome.
Medical treatment is not curative, but nifedipine, phenoxybenzamine and gabapentin may provide relief of pain.