Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Mark Duffill MBChB FRCP, Dermatologist, New Zealand (2001)
Reviewing dermatologist: Dr Ian Coulson (2023)
A milker's nodule is an infection of the skin caused by a virus that infects the teats of cows. It is sometimes called cowpock although it is important to note this is a different condition from cowpox (in recent reports from Europe, cowpox has been acquired from cats and small rodents rather than cows).
Milker's nodule is a farmyard pox and is also called paravaccinia, pseudocowpox, and milkers' node.
Milker's nodule is caused by a parapoxvirus. It produces mild infections of the teats of cows ie, ring sores, as well as ulcers in the mouths of calves. It is similar to bovine papular stomatitis virus, which affects the same sites in cattle. The two viruses are variants. Both can produce lesions on the hands of dairy farmers or vets who examine the mouths of animals. Human infection is from contact with infected lesions on the animals. Any human-to-human spread appears not to have been recorded. Orf is another parapoxvirus that affects sheep and goats.
After an incubation period of 5-14 days small, red, raised, flat-topped spots develop. Within a week they appear as red-blue, firm, slightly tender blisters or nodules (lumps), usually between 2 and 5 in number although they may be solitary or more numerous. The nodules are usually on the hands, particularly the fingers, but occasionally the face. The top of the nodules often develops a greyish skin and a small crust. Secondary bacterial infection can develop. Many patients develop red streaks up the lymph channels on the arms (lymphangitis) and some enlargement of the lymph glands.
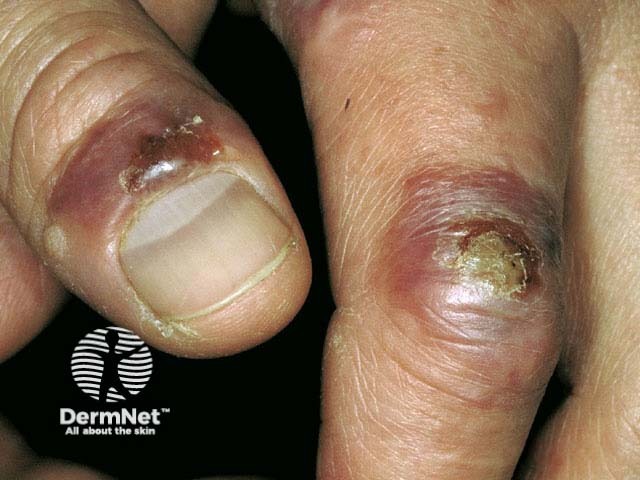
Milker's nodule
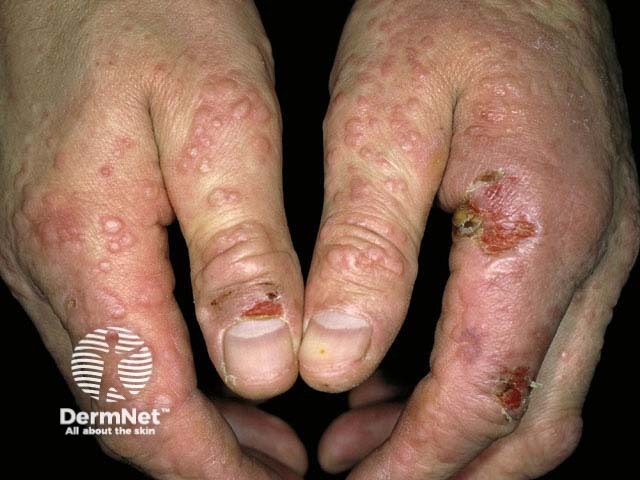
Milker's nodule
It is difficult to reliably distinguish milker's nodules from orf, the related condition in sheep, but the appearance of the nodules, number of lesions and whether cows or sheep are being mainly contacted is a guide. Similar lesions have recently been reported in humans infected with a distinct orthopox virus endemic in camels (camel pox) in India.
One or two weeks after the appearance of the milker's nodules, some patients develop erythema multiforme. This presents as an eruption of small raised spots or blisters on the hands, arms, legs and neck. This rash fades in 1–2 weeks.
In those at risk of the infection by their occupation, the diagnosis is made by the typical appearance of the lesions. Identification by electron microscopy and PCR is possible. A skin biopsy may be necessary. The characteristic pathological features of farmyard pox are epidermal hyperplasia, marked swelling of the dermis, intraepidermal and subepidermal blistering, and a dense mixed inflammatory infiltrate.
Milker's nodules can just be left to resolve spontaneously over 4-6 weeks. They should be covered to prevent contamination of the environment and also potential spread to other people. Gloves should be worn if milking. Any secondary bacterial infection should be treated.
Milker’s nodules may be more serious in those who have had stem cell transplantation; a case complicated by erythema multiforme and an exacerbation of chronic graft versus host disease has been reported.
Bera BC, Shanmugasundaram K, Barua S, et al. Zoonotic cases of camelpox infection in India. Vet Microbiol. 2011;152(1-2):29-38. doi:10.1016/j.vetmic.2011.04.010 Journal
Hansen SK, Mertz H, Krogdahl A, Veien NK. Milker's nodule--a report of 15 cases in the county of North Jutland. Acta Derm Venereol. 1996;76(1):88. doi:10.2340/000155557688 Journal
Slattery WR, Juckett M, Agger WA, Radi CA, Mitchell T, Striker R. Milkers' nodules complicated by erythema multiforme and graft-versus-host disease after allogeneic hematopoietic stem cell transplantation for multiple myeloma. Clin Infect Dis. 2005;40(7):e63-e66. doi:10.1086/428619 Journal