Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Genetic Connective tissue diseases
Author(s): Yasir Al-Dojaily, Virginia Commonwealth University School of Medicine, Virginia, USA. July 2022. Minor update November 2025.
Previously: Dr Darshan Singh, Dermatology Registrar, New Zealand, 2001. Copy edited by Gus Mitchell.
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Pseudoxanthoma elasticum (PXE) refers to a group of rare inherited disorders that affect the elastic connective tissue of the skin, eyes, and blood vessels.
PXE, alternatively called Gronblad-Strandberg syndrome, was first described in 1881 and occurs when abnormal calcification and mineralization of elastic fibres in affected tissues occur. It is characterised by yellow papules and plaques (which may mimic xanthomas), skin laxity, and ocular manifestations that may incur vision loss at later stages.
PXE is an autosomal recessive disease. While the true epidemiology of PXE is not currently known, the following has been estimated:
PXE is caused by inactivating mutations in a gene called ABCC6. The disease is autosomal recessive, meaning both copies of the defective gene must be present for PXE to occur. Over 300 mutation variants have been identified. Two common variants account for half of all cases of PXE.
PXE involves progressive deposition of calcium and phosphorus on elastic fibres. Deposits accumulate in elastin-rich tissue such as the reticular dermis of the skin, Bruch’s membrane of the choroid, and tunica media/intima of arteries. Elastic fibres eventually become fragmented.
The pathophysiology of PXE is currently understood to be due to metabolic derangement. ABCC6 encodes an ATP-dependent efflux transporter that excretes inorganic phosphate (PPi), a strong inhibitor of mineralization. Research has shown that decreased levels of PPi in the blood due to loss-of-function mutations of ABCC6 likely drive abnormal calcification in PXE.
Skin is the first organ to be affected by PXE, beginning in childhood or adolescence. Findings include:
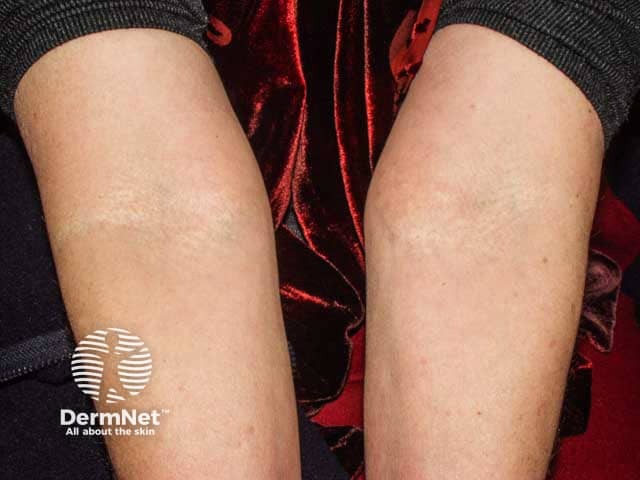
Yellow patches of pseudoxanthoma elasticum in the antecubital fossa
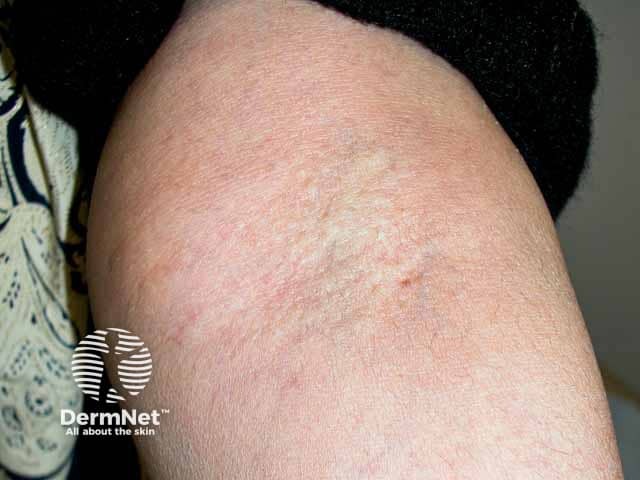
Yellow patches of pseudoxanthoma elasticum in the antecubital fossa
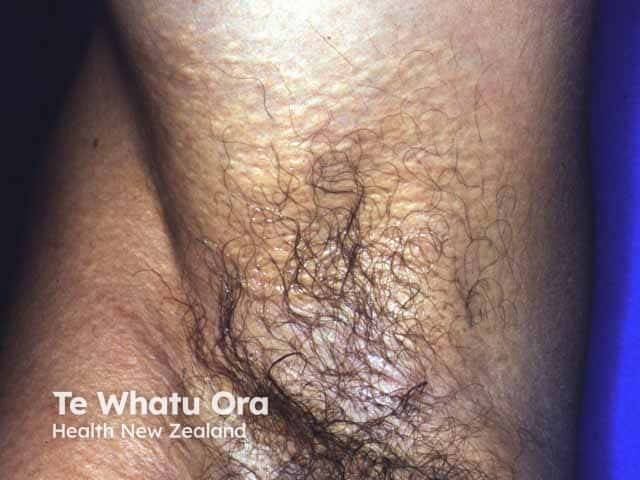
Yellow plaques and skin laxity in the axillae in PXE (PXE-patient2)
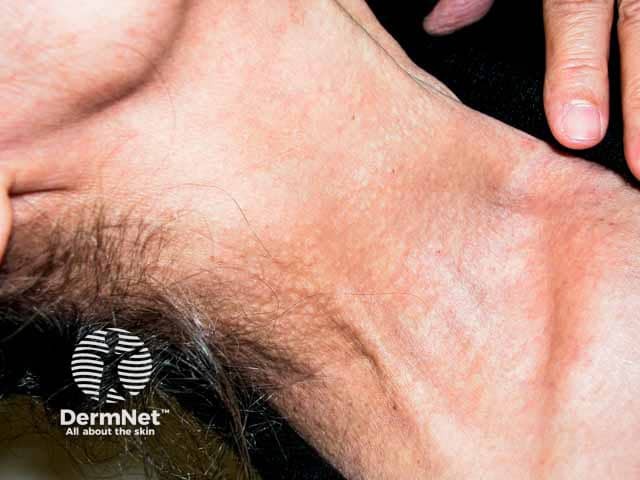
Yellow papules of PXE on the neck producing a "plucked chicken skin" appearance
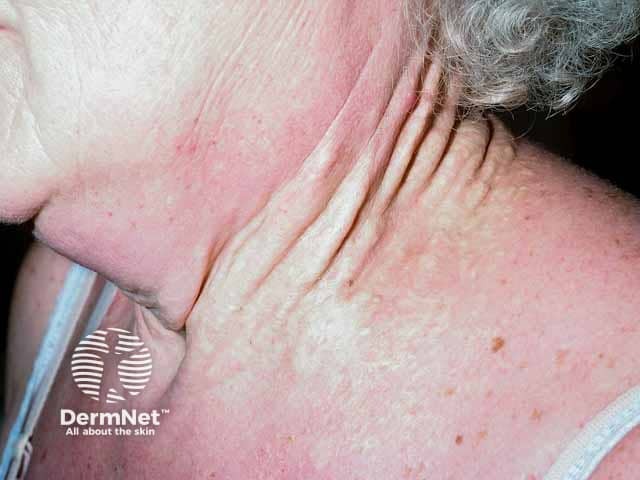
Longstanding neck pseudoxanthoma elasticum producing yellow plaques and skin laxity
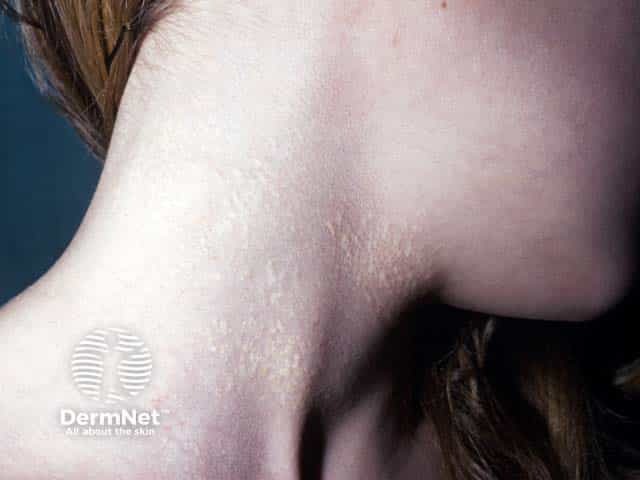
Yellow papules of PXE on the neck (PXE-patient3)
Bilateral ocular findings develop in all patients with PXE, beginning in childhood or early adolescence. Initial lesions are asymptomatic but may progress to vision loss with age.
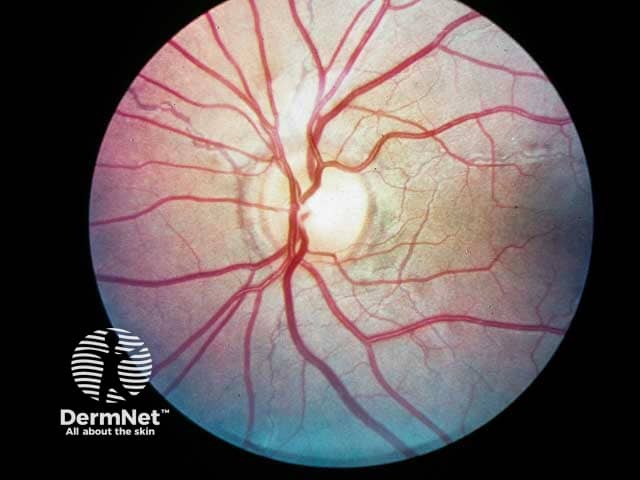
Angioid streaks extending from the fundus at 6 and 10 o'clock
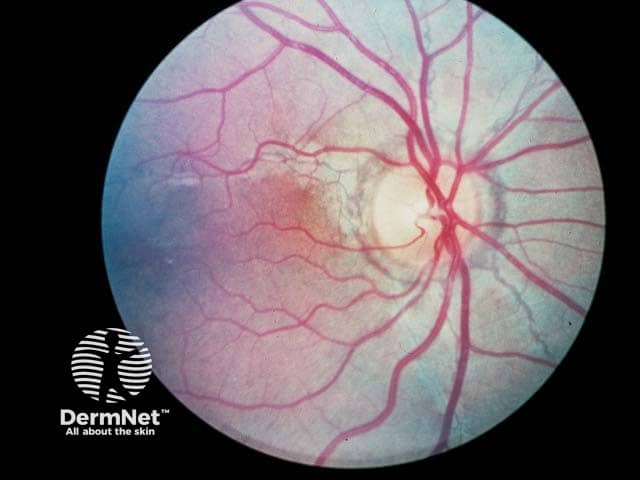
An angioid streak extending from the fundus at 5 o'clock
Other systemic features occasionally observed in PXE include:
Not much is known about the clinical features of PXE across different skin types. Certain mutation variants of ABCC6 have racial/ethnic associations and may cause varying disease phenotypes.
PXE is one of several conditions that can cause the skin condition elastosis perforans serpiginosa.
PXE may be diagnosed from its characteristic skin findings; histological confirmation is often useful. Ophthalmologists may perform a fundoscopy to diagnose pathognomonic ocular features.
Histopathology may be utilised in the diagnosis of PXE. Different staining techniques are used to reveal calcium deposits, shortened and fragmented elastic fibres, and deformation of collagen fibres.
Genetic testing for ABCC6 mutation homozygosity or compound heterozygosity is the gold standard test for PXE. Over 90% of patients have detectable mutations. Genetic testing can also rule out PXE-like conditions.
The most important aspect of treatment is to ensure that complications from blood vessel involvement are prevented or dealt with speedily by the appropriate specialist.
There is no current treatment targeting the underlying disease process of PXE. However, treatments exist for various disease manifestations:
PXE is not currently preventable but is a potential candidate for gene therapy. Genetic counselling may be helpful.
Individuals with PXE typically have a normal life expectancy. The extent of ocular or cardiovascular complications determines the morbidity and mortality of disease.