Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Adhar Mehta, medical student, University of Auckland, Auckland, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. April 2017.
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
Outcome
Ramsay Hunt syndrome is a rare peripheral facial neuropathy. It is a type of shingles due to reactivation of the varicella zoster virus (VZV) in the geniculate ganglion of cranial nerve VII, which supplies the facial nerve.
Ramsay Hunt syndrome is also known as herpes zoster oticus, geniculate ganglionitis, Ramsay Hunt disease and Hunt syndrome. The name was coined by neurologist James Ramsay Hunt in 1907.
Ramsay Hunt syndrome occurs in individuals with a previous history of varicella (chickenpox).
After primary infection by VZV (ie, chickenpox), there is a latent period where VZV remains dormant in the neurones of the cranial nerves, the dorsal root ganglion and autonomic ganglia. The reactivation of VZV in the geniculate ganglion of cranial nerve VII is what leads to the syndrome. VZV can also spread down the axons of other cranial nerves that share a blood supply with the geniculate ganglion.
Reactivation of VZV is more likely for:
The distinctly characteristic features of Ramsay Hunt syndrome are unilateral facial nerve paralysis and a painful vesicular rash on the ear and the mucous membrane of the oropharynx or palate. About 20% of patients develop facial nerve palsy several days before the blisters appear. About 10% of patients with Ramsay Hunt syndrome do not develop any blisters.
Other symptoms of Ramsay Hunt syndrome can include:
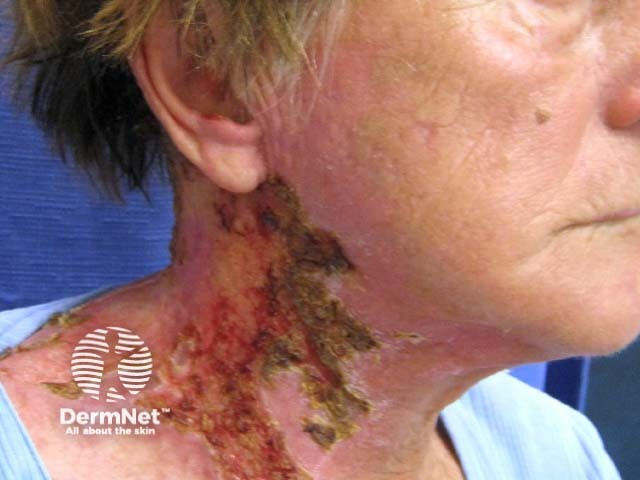
Herpes zoster
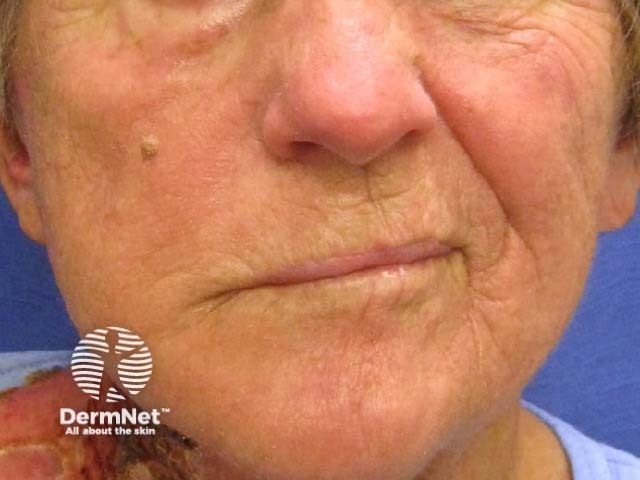
Facial nerve palsy
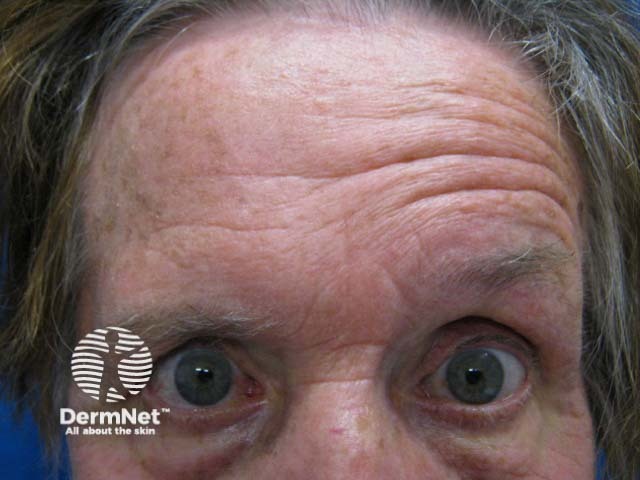
Facial nerve palsy
The diagnosis of Ramsay Hunt syndrome is usually made clinically. The diagnosis can be confirmed via testing with a VZV polymerase chain reaction assay (using ear exudate). This test is particularly useful to distinguish the zoster sine herpete variation of Ramsay Hunt syndrome from Bell palsy (idiopathic acute facial nerve palsy).
Magnetic resonance imaging (MRI) may be undertaken if there are polycranial neurological symptoms.
Full recovery is more likely if antiviral treatment is started within 72 hours of onset of symptoms. Treatment options for Ramsay Hunt syndrome are:
Symptomatic treatment during acute Ramsay Hunt syndrome may include:
Topical capsaicin can be used for post-herpetic neuralgia but is not well tolerated on facial skin.
Ramsay Hunt syndrome is associated with a poorer prognosis than Bell palsy; that is, complete recovery is less likely, particularly if antiviral treatment is not started within 72 hours of the onset of symptoms.
The House–Brachmann Scale, which correlates with the degree of facial nerve dysfunction, can be used as a prognostic tool.
Poor prognostic factors include:
Complications may include: